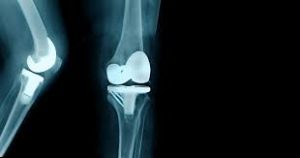
 Arthroplasty is an orthopedic surgical procedure where the articular surface of a musculoskeletal joint is replaced, remodeled, or realigned by osteotomy or some other procedure.
Arthroplasty is an orthopedic surgical procedure where the articular surface of a musculoskeletal joint is replaced, remodeled, or realigned by osteotomy or some other procedure.
It is an elective procedure, done to relieve pain and restore function to the joint after damage by arthritis or some other type of trauma.
An estimated 1.5 million total hip and knee arthroplastiess are performed each year in the US.
The most successful and common form of arthroplasty is the surgical replacement of arthritic or destructive or necrotic joint or joint surface with a prosthesis.
Other types of arthroplasty:
Interpositional arthroplasty, previously a popular form of arthroplasty, with interposition of some other tissue like skin, muscle or tendon to keep inflammatory surfaces apart.
Excisional or resection arthroplasty the joint surface and bone is removed, and
the remaining ends are attached, or left to give time for scar tissue to fill in the gap.
Resurfacing arthroplasty, where one or both bone surfaces are trimmed and replaced with a smooth metal covering.
Mold arthroplasty
Silicone replacement arthroplasty
Osteotomy to restore or modify joint congruity
Prostheses selected must be nontoxic, resistant, compatible and durable.
Prosthesis usually will not last 10–20 years.
75% of artificial knees will last 20 years and 90% will last 10 years.
In recent years the technology has been improved with a porous-coated prosthesis which allows for stronger bonding to the body, and computer-assisted design and manufacturing.
Complications of arthroplasty,
Blot clots or deep vein thrombosis
Infection
Bleeding
Periprosthetic fracture
Loosening
Mechanical wear
Failure
Deaths from pulmonary embolism previously affected about 3% of patients after total hip and knee arthroplasty, and now affects less than 0.2% of patients after these procedures related to the routine use of thromboprophylaxis.
Aspirin is increasingly prescribed after total joint arthroplasty because it is effective in primary and secondary prevention of venous thromboembolism and because fatal pulmonary embolism is less common in the contemporary period.
Aspirin is more convenient, less costly and perceived to have a lower risk of bleeding then parenteral agents used for prophylaxis.
Recent comparative randomized trials examining extended prophylaxis with aspirin, after at least five days of initial anticoagulant prophylaxis,was not inferior to either low molecular weight heparin or rivaroxaban in preventing symptomatic DTE in patients undergoing total joint or thrust arthroplasty.
