 Tinea nigra, is a superficial fungal infection, a type of phaeohyphomycosis rather than a tinea.
Tinea nigra, is a superficial fungal infection, a type of phaeohyphomycosis rather than a tinea.
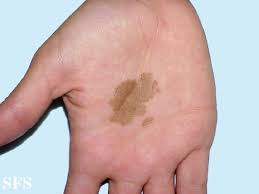
TN causes usually a single 1–5 cm dark brown-black, non-scaly, flat, painless patch on the palms of the hands and the soles of the feet of healthy people; there may be multiple spots.
Tinea nigra is extremely superficial and can be removed from the skin by forceful scraping.
The macules occasionally extend to the fingers, toes, and nails.
Lesions have been reported on the chest, neck, or genital area.
Skin lesions can present with multiple macules that can be mottled or velvety, oval or irregularly shaped.
The macule size can be anywhere from a few mm to several cm in size.
People of all ages can be infected.
Ot is generally more apparent in children and younger adults.
Females are three times more likely than males to become infected.
The fungus Hortaea werneckii, is the causative agent of tinea nigra.
Hortaea werneckii, is pigmented fungus, which is a dark yeast found in sewage, soil, rotting vegetation and wood and in places with a high salt content such as moldy salted fish and on beaches, where contact with sand may result in transmission.
Generally occurs in tropical and subtropical countries of Central and South America, the Caribbean, Europe, South East Asia, Australia and the Far East.
It is typically not found in the United States or Europe, although cases have been documented in the Southeastern United States.
Infection is by direct contact and the fungus enters and remains in the outer dead layer of skin with little or no skin inflammation.
The infection does not invade deeper tissues.
Diagnosis is by visualization, dermoscopy, and microscopy and culture of skin scrapings.
Differential diagnosis: Addison’s disease, syphilis, pinta, yaws, melanoma, lentigines, lichen planus of the palms, and junctional melanocytes nevus.
Treatment is with salicylic acid ointment.
Topical antifungals or oral itraconazole are other options, and scraping the lesion can be curative.
It can be prevented by improved hygiene measures.
Lesions tend to appear in areas where eccrine sweat glands are highly concentrated.
About 2–7 weeks post inoculation, lesions generally start to appear on the skin
H. wernickii produces darkly-colored, brown macules on the skin due to the production of a melanin-like substance, that remains localized in one spot or region.
H. wernickii has the ability to tolerate high salt concentrations and acidic conditions allows it to flourish inside the stratum corneum.
Diagnosis: based on microscopic examination of stratum corneum skin scrapings.
Such scrapings are mixed with potassium hydroxide (KOH), which lyses the nonfungal debris.
Cultured skin scrapings are cultured and allowed to grow for about a week when H. werneckii can generally be distinguished due to its two-celled yeast form and the presence of septate hyphae with thick, darkly pigmented walls.
Treatment consists of topical application of shampoo, which contains selenium sulfide, over the skin.
Topical antifungal imidazoles such as ketoconazole, itraconazole, and miconazole may also be used.
It is the same treatment plan for tinea or pityriasis versicolor.
Other treatments: epidermal tape stripping, Undecylenic acid, and other topical agents such as ciclopirox.
Once eradicated it is not likely to reoccur.
