 Spinal cord stroke is a rare type of stroke with compromised blood flow to any region of spinal cord owing to occlusion or bleeding, leading to irreversible neuronal death.
Spinal cord stroke is a rare type of stroke with compromised blood flow to any region of spinal cord owing to occlusion or bleeding, leading to irreversible neuronal death.
It is classified into two types, ischemic and hemorrhagic.
Ischemic accounts for 86% of all cases, a pattern similar to cerebral stroke.
It arises spontaneously from aortic illnesses or postoperatively.
Dysfunction includes motor or sensory function, and sometimes both.
Infarction usually occurs in regions perfused by anterior spinal artery, which spans the anterior two-thirds of spinal cord.
Preventions of the spinal cord stroke disease include, decreasing risk factors and maintaining enough spinal cord perfusion pressure during and after surgery..
Diagnosis of ischemic and hemorrhagic spinal cord stroke includes MRI and CT scans.
Treatments for spinal cord stroke are determined by the symptoms and the causes of the disease.
Antiplatelet and corticosteroids might be used to reduce the risk of blood clots in ischemic spinal stroke patients.
Rapid surgical decompression is applied to minimize neurological injuries in haemorrhagic spinal stroke patients.
Signs and symptoms of a spinal stroke are related to the portion of spinal cord affected, and occur below the level of lesion.
Abrupt onset of pain at the back or neck marks the location of ischemia or hemorrhage.
Temporary paresis in limbs may occur days before the onset of spinal ischaemic stroke.
It takes minutes for ischemic spinal stroke to develop the symptoms, but the time could be extended to days and weeks in hemorrhagic spinal stroke.
Infarction occurs predominantly in arteries, and their watershed region.
The thoracic spinal cord here, is susceptible to ischemic attack.
Patients with a male gender, younger age, lower body mass index, hypertension, diabetes mellitus, renal insufficiency and chronic obstructive pulmonary disease are predisposed to higher risks of severe spinal cord stroke.
Anterior spinal cord syndrome is related to losing motor function such as voluntary movement, reflexes and coordination as a result of compromised anterior and lateral corticospinal tract, anterior grey matter and spinocerebellar tract.
Also a loss in nociception and thermosensation as a result of interrupted spinothalamic tract occurs.
The posterior spinal cord syndrome manifests with impaired sensory functions namely vibration, fine touch, and proprioceptiom, which are associated to the dorsal column.
Unlike anterior spinal cord stroke, motor functions are not handicapped in posterior spinal cord stroke.
In the central spinal cord syndrome, impairment of motor function in the upper body is considerably more severe than that of lower body, which is related to hyperextension of corticospinal tracts and spinocerebellar tract in cervical spinal cord, accompanied by dysfunction in urinary bladder and sensational loss at a varying degree.
Brown-Séquard syndrome is only the subtype that affects the spinal cord unilaterally, either anteriorly, posteriorly, or both.
With the Brown-Séquard syndrome ipsilateral loss of vibration, fine touch, body position perception and fine movement control, as well as contralateral loss of axial muscles and movement coordination are found.
Spasticity followed by dysfunctinoal regulation of muscle tone also exists.
Death of cells at the complete transverse level is presented clinically as lower paraplegia or quadriplegia, sensory loss below the lesion, urinary incontinence, and disturbances in autonomous nervous system and hormonal system.
Aortic diseases are widely contributor sof spontaneous spinal cord ischemia, represented by rupturing of thoracic aortic aneurysm, arterial occlusion by aortic intima separated from endothelial wall in aortic dissection, and aortic coarctation.
Other factors include:embolism, meningeal inflammation at spinal cord, global ischemia and abusing nicotinic drugs.
Aortic surgeries contribute to many iatrogenic spinal cord ischemic events, although its percentage is much lower than that of spontaneous type.
Cases of spinal stroke following operations like aortography, spinal anesthesia and lumbar spine surgery are reported.
Abnormalities in blood vessels including arteriovenous malformations, arteriovenous fistulas and cavernomas can present as ischemic and occasionally hemorrhage manifestations.
The fusion between arteries and veins increases blood pressure in radiculomedullary vein and coronal venous plexus, which can cause a venous congestive myelopathy and infarction.
Prolonged compression on the blood network by vertebral diseases such as cervical spondylosis and protruded intervertebral disks can be attributed to acute ischaemia in spinal cord.
Trauma is a common cause of spinal cord hemorrhage for all four subtypes, namely haematomyelia, subarachnoid hemorrhage, subdural hemorrhage and epidural hemorrhage.
There is a correlation between anticoagulating drugs and hemorrhagic stroke.
The pathophysiology of spinal stroke is similar to its counterpart in brain.
The decreased blood flow hampers oxygen and glucose delivery to neurones, causing a huge decline in ATP production and failure of calcium pump.
The rising intracellular calcium level activates a series of enzymes like phospholipase A2 (PLA2), COX-2, calcineurin, calpain, mitogen-activated protein kinase, nitric oxide synthase, matrix metalloproteinases (MMPs) to produce proinflammatory and proapoptotic chemicals.
There are also activation of cytokines and changes in transcription factors, while glutamate is released to extracellular space and binds to its excitatory receptors, further exacerbating calcium influx and a cascade of events involving mitochondrial, cell membrane damage, and production of reactive oxygen species.
Such excitotoxicity is closely associated with the eventual neuronal cell death and loss of tract function.
Modifiable risk factors that contribute to the common strokes such as hypertension and heart disease, are found less commonly in the formation of spinal cord stroke.
Diabetes mellitus, peripheral artery disease, smoking and cholesterol are associated more with such disease: prevention and treatment of these modifiable risk factors could reduce the likelihood of spinal cord stroke.
Somatosensory evoked potential monitoring or motor evoked potential monitoring is necessary to early detect the spinal cord ischemia in anesthetized patients for quick intervention.
Cerebrospinal fluid drainage is used to decrease intraspinal pressure and increase blood flow to the spinal cord to avoid hypotension, thus reducing the risk of spinal cord ischemia.
Probability of postoperative spinal cord stroke is linked to both aneurysm extent, and length of graft, which highlights the importance of postoperative management.
Increasing the spinal cord perfusion as an immediate intervention may increase the chance of successful treatment.
Diagnosis:
Assessment of the clinical symptoms such as paralysis, sensory loss and urinary and bowel dysfunction, to determine whether it is a possibility for a spinal stroke.
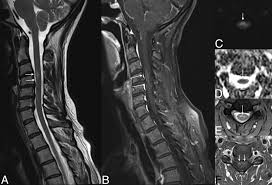
Different MRI protocols including axial and sagittal T1 and T2-weighted sequences and diffusion-weighted imaging.
Non-contrast CT and spine CT angiography are ineffective as imaging modalities, and MRI is used to confirm the diagnosis.
MRI findings: including pencillike hyperintensities on T2-weighted sagittal images and “owl’s”or “snake eyes” sign on T2 axial images, indicate the infarction is predominately in the watershed area of the gray matter of ventral horn as a result of an anterior spinal artery infarct.
A posterior paramedian triangular hyperintensity in T2 hyperintensity indicates posterior spinal artery infarct.
A routine MRI may show no abnormality especially for those patients in the acute phase.
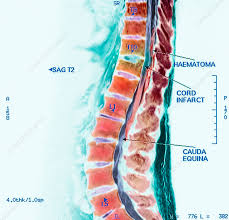
MRI with and without gadolinium enhancement is the preferred imaging to identify a hematoma in the spinal cord
CT can also identify hemorrhage and provide evidence of pathology of spinal cord damage.
It is necessary to differentiate between subdural and epidural hematomas.
Treatment:
Symptomatic treatment of associated complications is applied.
Ischemic spinal cord stroke:
If global hypoperfusion is present, maintaining enough blood pressure to maintain adequate spinal perfusion is needed.
Anticoagulant and antiplatelet agents have been prescribed to prevent vascular occlusion or embolism.
Corticosteroids are prescribed in situations of vasculitis or aortitis.
With acute hemorrhagic spinal cord stroke, surgical decompression to relieve pressure on the spinal cord is the goal.
There is a substantial link between the time from bleeding to surgical decompression and neurological outcome, with the greatest results coming from individuals who had surgery within 12 hours after symptom onset.
Administration of large dose corticosteroids are provided to
reduce edema and secondary cord compression.
Reversal anticoagulation is used to reduce the risk of bleeding by using suitable antidotes various anticoagulants associated with spinal cord hemorrhage.
Spinal cord ischemia patients could have a full recovery.
The mortality rate after spinal cord ischemia is relatively high at 23%.
58% of survivors are ambulating with or without gait assistance.
Patients with total paraplegia and sensory loss at nadir can, however, progress significantly over months to years.
