 Plaque psoriasis is a multi system inflammatory disease that affects children and adults.
Plaque psoriasis is a multi system inflammatory disease that affects children and adults.
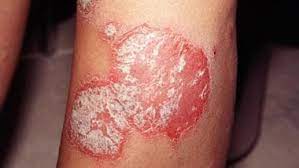
Skin lesions in PP are the most prominent manifestations, appearing as localized a widespread red plaques with silvery scales.
interleukin-23 plays a critical role in the pathogenesis of T cell activation in psoriasis.
Psoriasis, which manifests most often as plaque psoriasis, is a chronic, relapsing, inflammatory skin disorder with a strong genetic basis.
Plaque psoriasis is rarely life threatening, but it often is intractable to treatment.
Psoriasis may be associated with arthritis, obesity, metabolic syndrome, psychiatric disease, impaired quality of life, and increase cardiovascular disease risks.
Treatment depends on body surface area affected, the thickness, location of the lesions, the presence of symptoms such as itch and pain, and comorbidities.
Topical regimens using several different types of drugs are often prescribed because different body sites have unique characteristics of skin thickness, hair, skin to skin occlusion, they require a different vehicle formulation of creams, ointment, oils, and foam, and alternating treatment schedules to increase effectiveness and reduce toxicity.
Psoriatic plaques are characterized as follows:
Raised and easily palpable due to to the thickened epidermis, expanded dermal vascular compartment, as well as infiltrate of neutrophils and lymphocytes
Irregular to oval in shape.
One to several centimeters in size
Well defined, with sharply demarcated boundaries
Very distinctive rich, full red color; lesions on the legs sometimes carry a blue or violaceous tint
Typically have a dry, thin, silvery-white or micaceous scale
Skin lesions range in number from a few to many.
Skin lesions mostly often located on the scalp, trunk, and limbs.
Lesions have a predilection for extensor surfaces, such as the elbows and knees.
Skin lesions are symmetrically distributed.
Smaller plaques may coalesce into larger lesions, especially on the legs and sacral regions.
Manifestations of plaque psoriasis include:
Pruritus
Nail psoriasis
Inverse psoriasis – A variant of psoriasis that spares the typical extensor surfaces and affects intertriginous areas (ie, axillae, inguinal folds, inframammary creases) with minimal scale.
Psoriatic arthritis – Occurs in approximately 10-20% of all cases of plaque psoriasis
Manifestations of psoriatic arthritis:
Red, warm, tender, and inflamed joints,
joint deformity, dactylitis, sausage digits.
In children
Plaque psoriasis lesions in children are not as thick or scaly as in adults
Psoriasis lesions often appear in the diaper region in infancy, and in flexural areas in children.
Childhood plaque psoriasis affects the face more often in children than it does in adults.
The diagnosis of psoriasis is almost always made clinically.
Uncommonly skin biopsy is needed
to confirm the diagnosis of plaque psoriasis.
Histology:
Mitotic activity of basal keratinocytes is increased almost 50-fold.
There is keratinocyte migrating from the basal to the cornified layers in only 3-5 days rather than the normal 28-30 days.
The epidermis becomes thickened in appearance, and the rete ridges increase in size.
Abnormal keratinocyte differentiation is noted throughout the psoriatic plaques, as manifested by the loss of the granular layer.
Collections of neutrophils are sandwiched between layers of parakeratotic stratum corneum, which is virtually pathognomonic for psoriasis.
Histologic dermal findings: inflammation throughout the dermis, marked hypervascularity and an increase in the size of the dermal papillae occur,
activated CD3+ lymphocytic infiltrate is noted around blood vessels. and
an aggregation of neutrophils in the dermis occurs that extends up into the epidermis.
Management
Topical therapy
Corticosteroids
Coal tar
Calcipotriene
Tazarotene
Roflumilast topical
Phototherapy
The two main forms of phototherapy are as follows:
Ultraviolet B (UVB) irradiation – UVB therapy is usually combined with one or more topical treatments.
Psoralen plus ultraviolet A irradiation (PUVA) – This treatment uses the photosensitizing drug methoxsalen (8-methoxypsoralen) in combination with UVA irradiation to treat patients with more extensive disease
Systemic treatment is initiated only after topical treatments and phototherapy have proved unsuccessful., and for active psoriatic arthritis, as well as for patients whose disease is physically, psychologically, socially, or economically disabling.
Biologic therapy:
Targeting of activated T cells,
Prevention of further T-cell activation, and elimination of pathologic T cells
Blockage of interactions that lead to T-cell activation or migration into tissue
Alteration of the balance of T-cell types
Inhibition of proinflammatory cytokines, such as tumor necrosis factor (TNF), [6] interleukin (IL)–12, IL-17, and IL-23.
A number of biological agents affect interleukin-23, three target p19 subunit of IL-23, and one targets a p40 sub unit, which is present in both Interleukin – 23 and interleukin-12.
Selective blockade of the interleukin-23 receptor with targeted oral peptide icotrokinra resulted in significant higher incidence of skin clearance at week 16 than placebo among adults and adolescents with moderate to severe plaque psoriasis.
