667555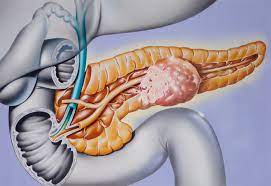 Pancreatic neuroendocrine less than 2-4% of all pancreatic cancers, with a incidence of less than 1 per 100,000 individuals.
Pancreatic neuroendocrine less than 2-4% of all pancreatic cancers, with a incidence of less than 1 per 100,000 individuals.
Incidence estimated to be 4 per million individuals per year in the U.S.
Gastroenteropancreatic neuroendocrine carcinomas represent roughly 55% of all extrapulmonary high-grade neuroendocrine tumors, the majority being metastatic at the time of diagnosis.
5-year survival rate of 44-71%.
Presumed earlier presentation of functional tumors, particularly insulinomas, associated with a better prognosis than non-functional tumors.
Thought to arise from islet cells of the pancreas and are known to have different outcomes based on grade, stage, and clinical presentation.
The overall incidence of neuroendocrine neoplasms have been steadily increasing along with improvement in overall survival overtime.
Definition of benign versus malignant bases on tumor size, lymph node involvement or the presence or development of distant metastases.
WHO classification utilizes size, presence of metastases, and grade related criteria, such as mitotic rate, perineural invasion, vascular invasion, and proliferative indexes.
Classified as grade 1, grade 2, and grade 3.
Grade is determined by both mitotic count and KI- 67 labeling index.
Generally slowly progressive lesions.
Pancreatic endocrine neoplasms-for patients who suffer recurrences unlikely to be cured.
Rates of 5-year survival for node negative nonmetastatic disease approximately 80%.
Rates of 5-year survival for patients with synchronous nodal or distant metastases 43%.
They generally do not respond to the standard treatments utilized, such as somatostatin analogues, everolimus, Sunitinib, and interferon.
Pancreatic neuroendocrine tumors can secrete a variety of peptide hormones, including gastrin, insulin, glucagon, somatostatin, and vasoactive intestinal peptide, that should be measured if there is concern for an associated clinical syndrome such as refractory peptic ulcer disease, episodic hypoglycemia, necrolytic migratoryerythema and diabetes mellitus, or persistent diarrhea.
The majority of pancreatic neuroendocrine tumors or not functional but still produce measurable levels of substances, including chromogranin A and AFP.
About 40% of patients who have pancreatic NETs present with local regional disease.
Mutations of chromatin remodeling genes MEN1, DAXX, and ATRX are common in pancreatic NETs and correlate with prognosis.
Histone methyltransferase and mammalian target of rapamycin (mTOR) pathways (PTEN, TSC2) are also common in pancreatic NETs.
Surgical resection of pancreatic NETs is the mainstay of therapy except for high-grade tumors, symptomatic or functional tumors, and tumors measuring at least 2 cm.
For patients with larger tumors in whom lymph node metastasis is strongly suspected a Whipple procedure is the preferred approach.
Surgical resection of primary disease and disease debulking along with systemic therapy may play a role in the management of symptomatic and functional pancreatic NETs.
Targeted therapy with everolimus (Afinitor) and sunitinib (Sutent) is approved by the FDA in unresectable, locally advanced or metastatic PanNETs.
Combining several medicines, particularly doxorubicin with streptozocin and fluorouracil is often effective.
Capecitabine/temozolomide combination is effective.
Radionuclide therapy with LU 177 is efficacious.
Although marginally effective in well-differentiated PETs, cisplatin with etoposide is active in poorly differentiated neuroendocrine cancers.
