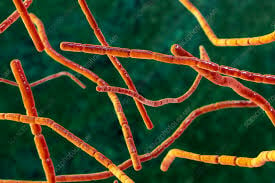
 Ubiquitous saprophytic bacteria in soil and water.
Ubiquitous saprophytic bacteria in soil and water.
Gram positive, aerobic bacteria.
Family Norcardiaceae.
Aerobic actinomycetes in decaying organic matter.
Environmental organisms found in soil, decaying vegetation, and aquatic environments.
Human infections are typically acquired to inhalation or direct inoculation.
Found in soil, water decomposing vegetation, fresh and salt water
May appear in tissues associated branching or beaded rods.
On microscopy appears as filamentous bacterium with hyphae-like branching.
Typically weakly acid-fast on traditional staining.
Cutaneous inoculation can cause lymphocutaneous norcardiosis.
Estimated 500-1000 cases of infection each year in the U.S.
Inhalation most common route of infection with the lung the most frequently involved organ.
Usually manifests as an opportunistic infection in immunocompromised patients, but up to one third of patients are immunocompetent.
Uncommon source of infection in patients with HIV.
Infrequent cause of lung cavitation.
Lungs most common organ affected.
Has a predilection for the CNS.
CNS most frequent extra pulmonary disease site.
Bacteremia associated with central venous catheters can occur.
N. asteroides accounts for 80-90% of cases of norcardiosis with N. brasiliensis. N. farcinia, N. nova and N. transvalensis accounting for the rest.
At least 30 species identified with at least 13 reported to cause disease.
Regarded associated an opportunistic infection with one third of patients immunocompromised.
The immune response to nocardia begins with neutrophil and macrophage phagocytosis, which helps contain the infection until T cell mediated bactericidal response can be activated.
Nocardia possesses virulence factors that allow it to evade immune defenses, including resistance to phagocytosis through filamentous growth and the production of enzymes, such as superoxide dismutaseand inhibition of phagosome-lysosome fusion with macrophages.
Increased risk with the use of corticosteroids, after organ transplant, cancer, diabetes, alcoholism and AIDS.
Up to 1/3 of Nocardia infections occur in patients who are not obviously immunocompromised.
May be an acute, subacute and chronic infectious process occurring in cutaneous, pulmonary and disseminated forms.
Primary cutaneous disease manifests as cellulitis or cellulitis lymphocutaneous infection, or subcutaneous infection.
Pleuropulmonary disease can be acute, subacute or chronic pneumonia and is usually seen in immunoincompetent patients, although it has rarely been seen in individuals with normal immune status.
While disseminated disease may involve any organ it most commonly involves the brain and meninges.
Traumatic inoculation related to cutaneous, subcutaneous and lymphocutaneous forms of disease.
Cutaneous, subcutaneous and lymphocutaneous disease not necessarily associated with immunosuppression, but dissemination more likely in immunocompromised patients.
Pleuropulmonary disease related to inhalation.
Dissemination occurs via hematogenous spread, usually from a lung process.
Most cases of disseminated disease occur in immunosuppressed individuals.
Gram staining of sputum may be helpful in the diagnosis
Diagnosis requires ability to demonstrate organisms on culture from a suspected site, which appear 2-7 days after culturing on most bacteriologic mediums.
Sulfa antibiotics are the standard of care, with alternatives such as minocycline, linezolid, imipenem and amikacin.
Antibiotic treatment is generally given for 6-12 months.
The choice of antibiotic depends on the susceptibility, severity, and distribution of the disease, as well as the immune status of the patient.
Isolated disease that is not severe can be treated with oral trimethoprim/sulfamethoxazole with monotherapy, whereas critical disseminated disease requires susceptibility testing and intravenous trimethoprim/sulfamethoxazole with one or more additional intravenous agents, imipenem or Amikacin, and other options include linezolid and ceftriaxone.
