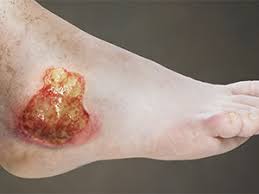
 See ((Pressure ulcers))
See ((Pressure ulcers))More than 2.8 million cases per year in the U.S.
Refers to lesions that have not undergone an orderly healing process.
It is largely the burden on older adults, for whom the incidence of chronic wounds for exceeds that of the younger population.
Prevalence for most wounds is greatest in patients 75 years or older.
Treatment variable as no consistent response to treatment occurs.
When wounds fail to undergo the usual complicated sequence of events for healing a chronic open wound results.
Have no anatomical or functional integrity.
May be associated with undue pressure, trauma, diabetes, venous insufficiency, arterial insufficiency and prolonged immobilization
Prevalence of pressure injuries in the US care facilities is estimated at 8.8% (2015).
Are not always infected.
Infected chronic wounds are diagnosed clinically by the presence of purulent exudate, swelling, heat and erythema, but many of these features may be absent and diagnosis depends on deep tissue biopsy culture.
Chronic wounds that are infected have significantly decreased flap repair survival.
Classic wound infection signs: none particularly helpful in diagnosing chronic wound infections.
When clinical suspicion of a chronic wound infection is present, a quantitative swab culture should be performed.
With Venous ulcers significant maceration and drainage are usually present at the malleoli or calf.
Underlying conditions that cause chronic venous ulcers associated with leg edema include: venous insufficiency, heart failure, cirrhosis, chronic kidney disease, and deep vein thrombosis.
Calcium channel blockers, NSAIDs, and certain oral hypoglycemics can cause leg edema and lead to chronic venous ulcers.
The primary prevention and treatment of venous ulcers is to control edema, and this can be accomplished by mechanical compression which can improve healing outcomes and shorten time to healing.
Among strategies to reduce edema: mechanical compression, wraps/bandages, stockings, and boots there’s insufficient evidence to definitively recommend a gold standard strategy.
Sound care in the management of venous ulcers includes dressings that are nonadherent, and absorbent to avoid wound maceration.
Debridement of necrotic tissue is typically a component of venous ulcer care.
Pentoxifylline when combined with compression treatment increases rates of complete healing versus compression alone.
Neuropathic ulcers commonly occur in the feet of patients with sensory loss, often caused by peripheral neuropathy. These lesions are frequently found on the toes or metatarsal heads, and may be preceded by callus formation in the areas of pressure.
Neuropathic ulcers frequently occur with diabetes.
Management of neuropathic ulcers includes complete offloading, with total contact casting being in the gold standard message to accomplish this.
Definitive which footwear and custom orthotics may be appropriate for long-term management.
Ongoing infections such as cellulitis, osteomyelitis or septic arthritis should be treated with appropriate antimicrobial agents.
In patients with nonhealing or chronically infected neuropathic ulcers are considered for amputation.
Local treatments includes debridement of ulcer and callus.
Hyperbaric oxygen therapy is a consideration.
Ischemic ulcers of the leg is most often seen in the context of peripheral arterial disease.
Management for ischemic ulcers is primarily an attempt at reestablishing arterial blood flow.
Local wound care for ischemic ulcers have limited benefit for ulcer healing.
Wound healing is a highly organized and complex process involving hemostasis, inflammatory response, proliferation and remodeling.
For wound healing to occur there must be: adequate tissue perfusion, an intact immune system, appropriate wound hydration, removal of necrotic/non-viable tissue, and management of infection if present.
Factors in wound care include protecting periwound skin, forming an effective bacterial barrier that conforms to the wound shape, producing minimal pain during dressing changes, avoiding non-biodegradable fibers being placed into the wound, and maintaining optimal wound temperature and pH.
Dressings do not heal the wound, the body does.
