 Primary immunodeficiency disorder.
Primary immunodeficiency disorder.
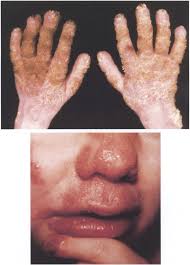
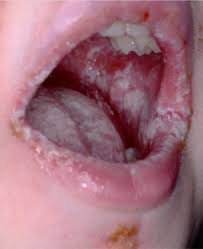
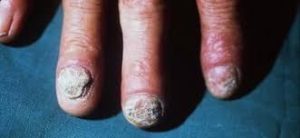
May be manifested by persistent or recurrent infections of the oral mucosa, skin, genital mucosa and nails with candida species.
Patients typically present with signs and symptoms of the diagnosis at a median age of one year, and or an increased risk of that viral, bacterial, and fungal infections.
These patients often have hypothyroidism due to autoimmune thyroiditis and they have other autoimmune conditions such as type 1 diabetes, autoimmune cytopenia, and systemic lupus erythematosus.
Several subtypes: autosomal recessive autoimmune polyendocrinopathy candidiasis with ectodermal dystrophy (APECED), autosomal dominant CMC with or without thyroid disease, and autosomal recessive, isolated CMC.
APECED resides in the autoimmune regulator AIRE which has a key role in immunotolerance.
In patients with APECED susceptibility to candida infection due to autoantibodies to interleukin-17 and interleukin-22, since type 17 helper T cells crucial for mucosal immunity.
Impaired clearance of fungal infections and results in colonization and infections of the mucosa or skin, predominantly with Candida albicans.
Associated with clinical processes such as HIV, or the use of corticosteroids, but can be related to a primary immunodeficiency.
Aside from Candida albicans patients may be susceptible to to dermatophytes.
Rarely can be associated with invasive infections with Candida species, Histoplasma or Cryptococcus.
Patients with a lack of T cell reactivity to Candida species.
TH1-Interferon gamma responses are defective in patients with autosomal dominant CMC.
Autosomal dominant CMC mutations in the coiled-coil domain of STAT1 underlies the defective Th1 and TH17 responses which explain the increased susceptibility to fungal infections.
More than half of CMC cases are due to variants in the signal transducer and activator of transcription transcription (STAT1) gene.
Patients with STAT1 gain of function variants are at increased risk of cerebral aneurysm and squamous cell carcinoma of the skin and esophagus.
Frequently associated with endocrine disorders.
Can be associated with hypothyroidism and adrenocortical insufficiency.
Most cases are sporadic, but familial involvement suggesting a recessive inheritance.
CMC is common in patients with autoimmune poly endocrinopathy candidiasis ectodermal dystrophy (APECED), which classically presents with a triad of CMC, hypo parathyroidism, and adrenal insufficiency.
APECED results from a variant in the auto immune regulator (AIRE) gene.
Normal B and T cell function and the diagnosis made by specific T cell challenge.
Differential diagnosis includes: other T cell deficiency diseases that cause chronic candidiasis such as HIV, severe combined immunodeficiency, CARD9 deficiency, CD 25 deficiency, and hyper immune globulin E syndrome.
These conditions typically are associated with invasive candida infections.
Diagnosis of CMC is usually made based on recurrent abnormalities of the skin, nails, and mucosa and by the identification of Candida species on fungal culture of skin scrapings or skin biopsy.
Definitive diagnosis came made by genetic analysis of peripheral blood mononuclear cells to identify a disease causing variant: whole exome sequencing can identify heterozygous STAT1 gene gain of function function variant.
Treatment with antifungal agents.
Chronic suppressive antifungal therapy can prevent recurrences, but drug resistance frequently develops with long-term treatment.
in patients with STAT1 gain of function variants who also have autoimmune or auto inflammatory disease a Janus kinase inhibitor such as ruxolitinib ot tofacitinib have had results of resolution of lesions.
