 Life threatening reaction to an offending agent manifested by respiratory, cardiovascular, cutaneous and gastrointestinal symptoms.
Life threatening reaction to an offending agent manifested by respiratory, cardiovascular, cutaneous and gastrointestinal symptoms.
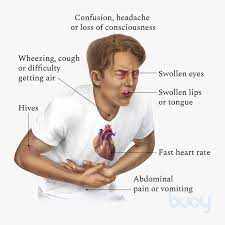
An acute onset of an illness within minutes to hours that occurs at the same time as skin or mucosal tissue involvement, or both, which could include generalized hives, or flushing, or swollen lips, tongue, uvula, and at least one of the following: respiratory signs or symptoms, wheeze, broncospasm, strider, hypoxemia, dyspnea, and reduced blood pressure or end organ dysfunction of hypotonia, syncope, incontinence, and gastrointestinal symptoms including frequent vomiting and abdominal pain with severe cramping, after an individual is exposed to unknown or highly probable allergen.
The differential diagnosis of anaphylaxis includes: acute bronchospasm, syncope, anxiety, and or panic attacks.
Etiologies include: drugs, foods, insect stings, radiographic contrast media, latex rubber, blood products, and physical factors.
Factors that contribute to a lower threshold to develop food induced allergic symptoms include: concurrent illness, fever, exercise, alcohol consumption, menstruation, and aspirin and other non-steroid anti-inflammatory drugs.
1 in every 3000 hospitalized patients suffers an anaphylactic reaction.
Almost always unexpected process.
1% of patients with anaphylaxis die.
Most common with antibiotics, especially penicillin and with radiocontrast media with a rate of 1 per 5000 exposures.
Penicillin accounts for 75% of fatal anaphylactic cases in the U.S. each year accounting for 1500 deaths per year.
Anaphylaxis accounts for about 40 deaths per year due to insect venom.
An estimated 150 people die annually from anaphylaxis due to food allergy.
More common than generally appreciated affecting 1.2% to 15% of the U.S. population.
Risk factors include age, atopy, preexisting asthma, mastocytosis and activating mutations of mast cells.
Mediators include histamine, tryptase, Carboxypeptidase A, prostaglandin D2, leukotrienes, and platelet activating factor which are released from mast cells and basophils.
A serum tryptase test obtained 90 minutes to 4 hours after a suspected food induced anaphylaxis event shows an increase by at least 1.2 times the patient’s basedline value +2 ng/mL is highly suggestive of mass cell degranulation, and helps confirm the diagnosis.
Approximately 100 food-related anaphylactic deaths occur each year.
Mediated by immunoglobulin IgE.
Leads to release of mast cell and basophil immune mediators.
Most common signs and symptoms include urticaria, angioedema dyspnea, wheeze, dizziness, syncope, nausea, vomiting, diarrhea, flush, upper airway edema, headache, change in mental status, rhinitis, substernal chest pain, pruritus and seizure.
Agents for management include aqueous epinephrine 0.2-0.5 mL of 1:1,000 dilution every 5 to 15 minutes up to a maximum of 1mg (1mg) per dose (adults), and .01 mL (0.01 mg)/kg body weight up to a maximum of 0.5 mL (0.5 mg) per dose of 1:1,000 weight to volume dilution.
