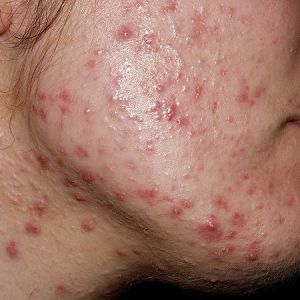
Acne vulgaris affects 40-50 million people in the U.S.
Affects up to 87% of adolescents.
Affects approximately 9% of the population worldwide, and approximately 85% of those age 12 to 24 years.
Affects more than 50% of the people age 20 to 29 years and approximately 43% of people age 30 to 39 years.
Approximately 18% of women and 8% of men develop acne after age 25.
It negatively affects quality of life and self-esteem and is associated with increase risk of anxiety, depression, suicidal ideation, and physical scarring.
A multifactorial disorder of the pilosebaceous unit.
Most common skin condition in the US.
Associated with pain, itching, soreness and impared quality of life.
A disease of pilosebaceous unit-the hair follicle in the skin associated with an oil gland.
A localized skin inflammation as a result of overactivity of oil glands at the base of hair follicles.
The inflammation can appear in the the form of a superficial pustule, a pimple, a deeper cyst, congested pores, whiteheads, or blackheads.
Associated with obstruction of the follicular orifice, with an increase in sebum production, and overgrowth of Propoonbacterium acnes.
Lesions are comedomes, which are whiteheads and blackheads, papulopustules, nodules and cysts.
Acne skin lesions are graded in severity from I to IV
Grade I: mainly comedones
Grade II: mixture of comdeomes and few inflammatory lesions
Grade III: inflammatory papules and pustules
Grade IV: nodulocystic acne, often with scarring
Clinical features include seborrhea, non-inflammatory lesions, inflammatory lesions and scarring.
Patients present with the spectrum of lesions including open and closed, referred to as blackheads and whiteheads, respectively, erythematous papules and pustules, and cystic nodules.
Clinically varies from mild non inflammatory comedonal acne to fulminant disease.
Noninflammatory lesions are open and closed comedomes.
Inflammatory lesions include papules and pustules.
Typically begins at puberty and is often the first sign of increased sex hormone production, especially testosterone.
85-90% of all teenagers have some degree of acne.
Generally resolves by age 25, but great variability in age of onset and resolution exists, with acne persisting into the 20s and 30s in 64% and 43% of individuals, respectively (Bhate K).
At age 40, lesions persist in 5% of women and 1% of men.
May appear in decades beyond adolescence with manifestations during the third or fourth decades and sometimes persists into the fifth decade of life.
In women acne often flares before menses and is referred to as female hormonal acne.
Worsening with menstruation occurs in up to 40% of women.
Distribution of lesions corresponds to highest density of pilosebaceous units-the face, neck, upper chest, shoulders and back.
Four processes lead to acne: inflammation my mediators releases into the skin, keratinisation leading to comedones, increased and altered sebum production by androgen control or altered andrgen receptor receptivity, and follicular colinization by Propionbacterium acnes.
Sebacious glands produce antimicrobial peptides, neuropeptides, and antibacterial lipids.
Sebaceous gland functions act like an endocrine organ influenced by corticotropin releasing hormone , reflecting the link between stress and acne exacerbations.
Sebaceous follicles containing a comedome provides an anaerobc and lipid rich environment allowing P acnes proliferation.
P acnes resistance to oral antibiotics affects treatment responses.
P acnes proliferation augments lipogenesis.
Various P acnes strains colonize different pilosebaceous units and induce inflammation by activating toll-like receptors in keratinocytes and macrophages.
Noted to some degree in 54% of women and 40% of males older than 25 years.
Some degree affects almost all people aged 15-17 years, and moderate to severe in about 15-20%
Highest incidence occurs in the middle to late teenage years in both boys and girls, but may persist through the fourth decade of life in as many as 10-12 percent of the population.
28-61% of 10-12 year olds, 79-95% of 16-18 year olds are affected.
In a study of 2000 adults more than 3% of men and 5% of women have mild acne at the age of 40-49 years.
Typically starts in early puberty with increased facial grease, mid-facial comedomes, and followed by inflammatory lesions.
Factors contributing to the pathogenesis of acne include increased androgen levels causing sebaceous hyperplasia, altered keratinocyte proliferation and differentiation, follicle colonization by Propionibacterium acnes, and immune response causing inflammation.
A chronic disease that can persist for long periods of time.
Acne of early onset, before age 12 years, is usually more comedonal than inflammatory.
Expansion of Propionibacterial facial skin and nares flora occurs earlier in children who develop acne than in children who do not.
Predictors of acne severity include early onset of comedonal acne, and number of family members with history of acne.
Gradual decrease in prevalence after age 20 years.
Mild disease, decreases or disappears in the majority of acne patients in their teens.
Incidence is lower in nonindustrialized societies compared to westernized civilizations.
Flares associated with stress, menstrual cycle, and manipulation.
A diet of higher saturated fat and refined grains is linked to a greater risk of adult acne.
High glycemic diet may exacerbate acne by increasing insulin and insulin like growth factor 1, which can induce lipogenesis and proliferation of keratinocytes and sebocytes, stimulate androgen synthesis and decrease production of sex hormone binding globulin.
Studies suggest an association between dairy products and acne.
The NutriNet-Sante study was a survey of health and demographic information administered to over 170,000 initial participants.
This study is focused on adult acne, not adolescent acne.
In those in the animal products and refined cereals group were just 3% more likely to have current acne.
The greater intake of meats, fish, vegetables, or fruits were associated with a slight-to-moderately lower risk of acne.
Drinking milk or sugary beverages as well as consuming fatty and sugary products were more significantly associated with greater risk of adult acne.
A greater intake of meats, fish, vegetables, or fruits were associated with a slight-to-moderately lower risk of acne, drinking milk or sugary beverages as well as consuming fatty and sugary products were more significantly associated with greater risk of adult acne.
Medications that can worsen acne include steroids, progestins, lithium, phenytoin, and iodides.
Medications that can worsen acne include: corticosteroids, progestins, lithium, phenytoin, and iodides.
Results from hyperkeratinization and obstruction of sebaceous follicles, androgen stimulation of sebum production and skin colonization by Propionbacterium acnes.
As teens age, cytokines that induce comedogenic changes in the follicular infundibulum decrease resulting in remission.
Adults with adult acne related to circulating androgens occurs most commonly in women after the age of 25 years.
Hormonal related acne may benefit from spironolactone therapy.
Spironolactone is an inexpensive generic oral agent that is generally well tolerated and modulates one of the fundamental defects leading to acne: testosterone stimulation.
Characteristic of polycystic ovary syndrome in which patients have excess androgen levels.
A positive family history significantly increases risk of the development of acne.
Process appears earlier in girls, but more boys are affected during mid-teens.
Can occur occur at younger ages and more comedonal in black children (Do JE et al).
Hyperinsulinemia increases the synthesis of sebum and the development of acne.
Increased insulin resistance and high serum dehydroepiandersterone reflect the presence of acne in paitients with polycystic ovarian syndrome.
Smoking increases risk of severe acne.
Worsened by sweating, occlusion of skin by pomades, and clothing.
Associated with depression, suicidal ideation, anxiety, psychosomatic problems, embarrassment, and social inhibition.
Can be a disfiguring process resulting in permanent scarring and significant psychosocial disability, with the quality of life in patients with acne similar to patients with chronic medical conditions such as asthma, epilepsy, diabetes, and arthritis.
Associated with tyrosine kinase inhibitors.
Antiepileptic agents and anabolic steroids can be related.
Treatments works by preventing new lesions rather than treating active lesions.
It can be effectively treated in almost all patients.
Treatment may require months to be effective.
When considering treatment for disease morphology, severity, patient characteristics including age, skin color, psychological burden, and patient motivation are considered.
Many treatments topical and oral or contraindicated during pregnancy or lactation.
First line therapies are topical retinoids, benzoyl peroxide, azelaic acid, or combinations of topicals.
For more severe disease, oral anabiotic such as doxycycline or minocycline, hormonal therapy such as combination oral contraceptive agents or spironolactone, or isotretinoin are most effective.
Oral antibiotics are commonly used to induce rapid control of moderate to severe inflammatory acne, generally in combination with a topical retinoids and benzoyl peroxide.
Oral antibiotic use should not be as a monotherapy and there should be limits to the duration of treatment for 3 to 4 months.
The most commonly used oral antibiotics are tetracyclines including second generation tetracyclines, doxycycline, and monocycline.
Accutane (isotretinoin) is only indicated for treatment of severe recalcitrant nodular acne that is not responsive to conventional therapy including antibiotics.
Isotretinoin is approved for treating severe recalcitrant nodular acne, but is often used to treat resistant to persistent moderate to severe acne, as well as acne producing scarring or significant psychological distress.
Topical treatments work at the site of application to reduce new lesion development and should be applied to a whole affected area rather than to specific lesions.
Benzoyl peroxide is a topical treatment applied at 2.5 or 5% to affected areas, and is as affective as oral antibiotics.
Benzoyl peroxide associated with skin irritation.
Benzoyl peroxide penetrates the stratum corneum and it enters the pilosebaceous unit where C acne’s resides, generating free radicals to damage the cell wall of the pathogenic bacteria.
Benzoyl peroxide has mild anticomedolytic and anti-inflammatory properties, and limits the development of bacterial resistance to topical and oral antibiotics, and provides increased efficacy in comparison with topical antibiotics alone.
Topical retinoids are antiinflammatory and act on abnormal keratinisation and are useful for comedomal and inflammatory acne.
Topical retinoids, either as monotherapy or in topical combinationare the first line therapies of acne.
Retinoids are vitamin A derivatives that bind to retinoic acid receptors and retinoid X receptors in the keratinocyte cytoplasm and translocate to the nucleus to initiate transcription changes.
Retinoids stimulate epidermal cell liberation, loosing connections among cells in the stratum corneum, accelerate elimination of sebum in sebaceous ducts, and promote micro comedone clearance.
Retinoids reduce the amount of sebum produced by the sebaceous glands.
Topical antibiotics act on P acnes and reduce inflammation,by inhibiting the complement pathways and impairing neutrophil chemotaxis.
Topical antibiotics are more effective for inflammatory lesions than comedones, but reduce biofilm reducing microcomedones.
Bacterial anabiotic resistance with both tropical and systemic use occurs as quickly as six weeks and therefore antibiotics as monotherapy is not recommended.
Topical salicylic acid, dapsone and azelaic acid have been utilized.
Systemic treatments available for acne include antibiotics, contraceptive pills, and isotretinoin.
Isotretinoin is the only acne medication with potential to result in a complete remission of the process.
Isotretinoinso is highly efficacious, comedolytic, decreases sebum production, reduces abundance of C. acnes in sebaceous follicles, and has anti-inflammatory properties.
Relapse after isotretinoin therapy is common.
Isotretinoin usual dosage guideline starts at a dose of 0.5 mg per kilogram per day for the first four weeks, increases to 1 mg per kilogram per day thereafter until a cumulative dose of 120-950 mg/kilogram is given, which may take up to 4-6 months.
Hormonal therapy using antiandrogens, such is spironolactone suppresses ovarian androgen production and blocks the effects of androgens on sebaceous glands, decreasing sebum production and improving acne.
Spironolactone is effective against acne in female patients.
Spironolactone has similar efficacy as oral antibiotics.
Limited studies suggest laser, chemical peels, Photodynamic therapy, intralesional steroid injections may be of benefit.
