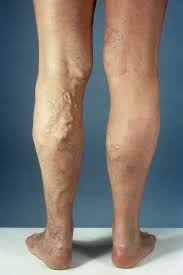
 Most common manifestation of chronic venous insufficiency in the lower extremities caused by valvular incompetence or postthrombotic syndrome.
Most common manifestation of chronic venous insufficiency in the lower extremities caused by valvular incompetence or postthrombotic syndrome.
Varicose veins and spider veins occur in the lower extremities due to the upright position and hydrostatic pressure.
Prevalence in general population is 50-55% in women and 40-50% in men.
Effects approximately 24 million Americans.
Medical costs approximately $1 billion/year, primarily for ulcerative changes.
The difference of spider veins, reticular veins, and varicose veins is dependent on size, with a varicose vein being at least 3mm in diameter.
Chronic venous insufficiency affects 2-5% of Americans.
A study In 1994 found half of the adult population have minor stigmata of venous disease and fewer than half have visible varicose veins.
More common in women and with age.
Approximately 23% of adults have varicose veins in the US.
An estimated 22 million women and 11 million men between the ages of 40 and 80 years have varicose veins.
Of the above, 2 million develop skin changes.
Expanding the definition of VV to include cosmetic telangiectasias would increase their presence in 79% of men in 88% of women.
The cause of primary varicose veins is incompetent venous valves resulting in venous hypertension.
The weight of the blood continuously pressing against the closed valves causes them to fail, leading to vein distention.
Classified using class, etiology, anatomy, and pathophysiology.
Risk factors include female gender, prolonged standing, increased height, congenital valvular dysfunction, venous hypertension of obesity, and multiple prior pregnancies.
Uncomplicated varicose veins not independent risk factors for DVT, except for individuals greater than 65 years of age.
Uncomplicated varicose veins may be a marker for thrombosis (Sobreira ML et al).
Occasional patients with recurrent superficial thrombophlebitis or greater sapheinous vein thrombus may have a hypercoaguable state.
Considered an autosomal dominant illness with incomplete penetrance.
If both parents have varicose veins, offspring have a 90% chance of having them as well.
Secondary varicose veins result from deep venous thrombosis and its complications or congenital anatomic abnormalities.
The etiology classified into three groups: Primary, secondary and congenital.
Primary disease is due to valvular insufficiency of the superficial veins, most commonly at the saphenofemoral junction.
Secondary disease mainly caused by deep vein thrombosis that leads to chronic deep venous obstruction or valvular insufficiency, catheter induced, pregnancy related and trauma induced.
Congenital disease includes any venous malformations.
Varicose veins refer to dilated, tortuous veins of the subcutaneous/superficial venous system.
Natural history of VV is progressive.
Pregnancy causes increasing symptoms and physical findings that remit with end of pregnancy.
Two venous systems are found in the lower extremity, the deep and superficial.
The deep system leads backs to the inferior vena cava and then heart.
The superficial system is found within the subcutaneous tissue.
Superficial veins drain into the the greater saphenous vein and the short saphenous vein.
Can be caused by congenital absence or damage to the venous valves in superficial and communicating systems.
Thrombi formation in veins can cause chronic venous insufficiency.
Varicose veins are rarely associated with the development of pain the popliteal fossa in some patients.
Majority of patients never develop stasis ulcers.
Palpable thrombosed vessels are superficial veins, but an associated DVT may exist in as many as 40% of patients with superficial phlebitis.
Surgical removal or obliteration of varicose veins may be achieved for cosmetic reasons alone or for pain, fatigability, heaviness, recurrent superficial thrombophlebitis, bleeding or for skin or subcutaneous tissue changes, such as lipodermatosclerosis, atrophie blanche, ulceration, or hyperpigmentation.
Sclerotherapy and thermal ablation techniques such as endovenous laser ablation are alternatives to surgery for the treatment of varicose veins.
In a randomized trial, quality-of-life five years after treatment was better after laser ablation or surgery than after foam sclerotherapy (Brittenden J)
In a randomized trial comparing foam, laser, and surgical treatments for varicose veins, generally similar quality of life results with the exception of slightly worse disease specific quality life in the foam group than in the surgery group (Brittenden J et al ).
In the above study the treatments had similar clinical efficacy, and complications were less frequent after laser treatment and ablation rates were lower after foam treatment.
Conservative treatment with stockings and external compression is the initial treatment but in the presence of worsening cutaneous findings or symptoms surgical management may be needed.
Conservative management includes: compression stockings, weight loss, leg elevation, and medications.
Compression stockings that compress at 20-30 mmHg help with pain and edema.
With venous stasis ulcers compression stockings are used with a pressure of 30-40 mmHg.
Patients who cannot remain active enough to reduce the risk of postoperative deep vein thrombosis (DVT) should not undergo surgery for varicose veins.
Surgery during pregnancy is not indicated because many varicose veins of pregnancy spontaneously regress after pregnancy.
