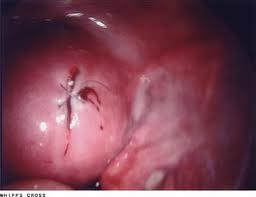
 Uterine perforation is a potential complication of any intrauterine procedure.
Uterine perforation is a potential complication of any intrauterine procedure.
It may be associated with injury to surrounding blood vessels or viscera such as the bladder or intestine.
The risk of perforation during gynecological procedures range to 0.1 to 4%, with the risk of perforation highest during postpartum procedures, lower doing operative hysteroscopies (1%) and lowest in diagnostic hysteroscopies or procedures, with pre-menopausal patients.
If not diagnosed it can occasionally result in massive hemorrhage or sepsis.
The majority of uterine perforations are sub-clinical and safely resolve by themselves without treatment and do not cause any significant long-term damage.
Risk factors include cervical stenosis during trans-cervical procedures or decreased strength of the myometrial wall as in pregnancy or menopause.
Prevention requires careful preop evaluation, the use of appropriate instruments, the use of appropriate intraoperative techniques, and adequate training and experience of the surgeon.
Appropriate preoperative imaging, assesses the anatomy, and can identify potential risk factors,
Pre-operative factors, include cervical preparation with prostaglandins or osmotic dilators, and consideration for treating vaginal atrophy.
Most perforations occur at the beginning of the procedure with insertion of cervical dilators, hysteroscope, or sharp instruments.
The incidence of perforation can be reduced by a bimanual examination prior to an dilation, placement of a tenaculum on the cervix to straighten the cervical canal, and specialized instrument utilization to identify and dilate the cervical canal use of ultrasound aid with difficult endometrial access, and the proper use of energized instruments.
The risk of uterine perforation is increased with cervical stenosis, or severe anteflexion/retroflexion.
Menopause, prior myomectomy, or pregnancy increase the risk because these conditions weaken the uterine wall.
The number of perforations that occurs likely to be higher than reported as many are not recognized or reported.
Uterine perforation is confirmed when either direct visualization, or when fat with bowel is visualized during the procedure or in a suction instrument or curettage specimen.
Uterine perforation should suspected intraoperatively if there’s unexplained, excessive, bleeding, hypotension, or hematuria.
If hemodynamic instability exists, patients may require transfusion.
For hemodynamically stable patients treatment depends on the location of the perforation.
Uterine perforation can occur in lateral, fundal, anterior, or a posterior aspect of the uterus.
Fundal perforations can be managed expectantly, otherwise abdominal exploration is necessary to exclude bowel injury and assess for bleeding.
Anterior or posterior perforations may require proctoscopy or cystoscopy to evaluate for bowel and bladder injury and immediate repair would be necessary.
Lateral perforation, are evaluated for bleeding, and should be managed immediately by laparoscopic care.
Delayed recognition of a complex uterine perforation is serious consequences, and is associated with significant mobility, including additional surgery.
Intrauterine adhesions, and infertility may occur as long-term complications of uterine perforation.
