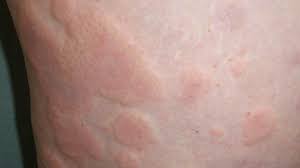
Raised, erythematosus wheals accompanied by pruritus.
Also know as hives.
Specific causes are wide ranging, but an estimated 20-30% of cases of chronic type urticaria are due to physical urticaria.
Physical urticaria refers to the presence of pruritic wheel and flare skin reaction precipitated by external physical stimuli.
Chronic urticaria is classified as inducible if symptoms are elicited reproducibly specific external triggers, such as cold, skin pressure, friction, light, and contact with wheal inducing agents, such as plant or animal products or metals.
Subtypes of physical urticaria characterized by the nature of the stimulus, including dermatgraphism,, vibratory urticaria, contact urticaria, cold contact urticaria, solar urticaria, aquagenic urticaria, and cholinergic urticaria.
Cholinergic urticaria is induced by active or passive heating of the body and accounts, for approximately 5% of cases of chronic urticaria and up to 30% of the inducible form.
Exercise can provoke urticaria in patients with cholinergic urticaria or in a separate defined88r6 group.
There are two types of exercise induced urticaria and anaphylaxis: one type is provoked by exercise; and the other type develops with exercise that coincides with the ingestion of food.
In approximately 20 to 30% of patients with chronic urticaria, cutaneous exacerbations are provoked by the use of nonsteroidal anti-inflammatory drugs, including aspirin.
Spontaneous urticaria in which urticarial, angioedema or both occur in an unprompted fashion.
Inducible urticarial previously, designated is physical urticarial, in which urticarial angioedema or both are elicited by factors such as cold, heat, or pressure.
15-25% of people experience urticaria at some point.
50% of cases involves not only the dermis but also subcutaneous or submucosal tissues, or both, resulting in angioedema.
Hives characterized by localized mast cell degranulation and increased dermal vascular permeability resulting in pruritic edematous wheal lesions.
Most often occurs between ages 20-40, although all ages susceptible.
Lesions fade within hours and episodes may last for days to months.
Lesions may coalesce.
Most common sites are the trunk, distal extremities and ears.
Majority of cases no etiology identified.
Most cases related to antigen induced release of vasoactive mediators from mast cells through sensitization by IgE antibodies.
Lesions results from degranulation of cutaneous mast cells, which leads to the release of histamine, the major mediator pruritic wheals and angioedema, as well as the release of cysteinyl leukotrienes, prostaglandins, platelet activating factor, and other substances.
Pro-inflammatory cytokines and vasoactive chemicals are also released with vasodilatation and plasma leakage from vasculature around the skin.
IgE dependent degranulation can follow exposure to pollen, food, drugs and other antigens and results from bridging of mast cells bound to IgE by multivalent ligand.
Simple urticarial lesions are pruritic, edematous, evanescent plaques that last generally less than 24 hours.
Urticarial vasculitis tends to be painful, burning and generally last longer than 24 hours, and often leads to hyperpigmentation, particularly after repeated episodes.
Chronic idiopathic urticaria, also known as chronic spontaneous urticaria, is defined as itchy hives lasting for at least six weeks, with or without angioedema, and have no apparent trigger.
Chronic urticaria may occur at any age, but mostly affects women and patients both sexes tend to be over 40 years of age.
There is an estimated 500,000 people in the US with chronic urticarial, a prevalence of 0.23%.
Chronic urticaria has substantial effects on daily life with intense pruritus that disrupts sleep, and restricts physical and emotional functioning.
Chronic spontaneous urticaria is a benign process with symptoms that adversely affect quality of life including disrupted sleep, distracting pruritus and unsightly wheals.
Chronic idiopathic urticaria can last for up to 1 to 5 years, and can persist in 11-14% of patients for greater than five years.
In chronic urticaria has a higher rate of coexisting psychiatric conditions than in the general population.
In chronic idiopathic urticaria mast cells are associated along with basophils and IgE in its pathophysiology.
Some patients with chronic urticarial have an underlying systemic disorder such as rheumatologic disease, infection or a hematologic malignancy, but this is rare as most do not have an identifiable exogenous cause.
Chronic urticaria has been reported in infections such as hepatitis B and C, Epstein-Barr virus infection, herpes simplex virus infection, mycoplasma infection, Helicobacter pylori infection, and helminthic infestations, rheumatologic diseases such as SLE and rheumatoid arthritis, thyroid diseases, neoplasms particularly lymphoreticular cancers and other lymphoproliferative disorders, ovarian tumors, and oral contraceptive use.
Chronic urticaria is characterized by pruritic wheals with circumferential erythema on any part of the body.
Lesions range from a few millimeters to several centimeters in diameter and resolve in less than 24 hours, without residual changes.
2/3 of patients have both urticaria and angioedema with the remaining 1/3 having only one or the other.
Angioedema which is characterized by a similar pathogenesis but occurs in the deeper dermis and subcutaneous tissues, may also be present and typically affects the face, the extremities, or torso.
Microscopic findings of lesions include a lymphocytic infiltrate in acute and chronic urticarial lesions along with some eosinophils and neutrophils.
Chronic urticaria is classified as spontaneous if symptoms appear without a known specific trigger, and can occur as a single episode or repeated episodes.
Chronic spontaneous urticaria affects approximately one percent of the global population, most commonly females age 30 to 50 years.
Symptoms of chronic spontaneous urticaria last for at least three years in approximately 66% of patients.
Most patients with chronic spontaneous urticaria develop only wheals(57%) , 37% have wheals and angioedema, and 6% have only angioedema.
In some patients with chronic spontaneous to carry the disease can be exacerbated by stress, nonsteroidal, anti-inflammatory drugs and infections.
Because spontaneous attacks occur without identifiable triggers prevention is not possible.
Chronic spontaneous urticaria has skin mast cells as its primary driver.
In most patients with spontaneous chronic urticaria IgG and IgE immunity can occur and contribute to the activation and degranulation of skin mast cells.
Less than 35% of patients with chronic spontaneous urticaria have no autoantibodies.
The linking of IgG and IgE autoantibodies on skin mast cells activate cytoplasmic signaling proteins, resulting in the release of vasoactive substances, including histamine, the major contributor to urticaria symptoms, and cytokines, leading to activation of sensory nerves, vasodilation, and increased vascular permeability and migration of immune cells, such as eosinophils, T lymphocytes, and basophils into the skin.
The susceptibility to chronic urticaria may be determined by genetic factors, gut microbiome alterations and levels of short chain fatty acid producing bacteria.
With chronic spontaneous or a carrier patients develop individual wheals, ranging from a few millimeters to several centimeters in diameter and typically appear and disappear within a single day, usually within a few hours, whereas angioedema typically lasts one to three days.
In acute urticaria, a cause such as a drug, food or infection can usually be identified.
In the chronic form of urticaria there is usually no identifiable cause, as lesions may be provoked by physical stimuli, leading to the release of histamine with a pruritic wheal-flare response that is characteristic of chronic urticaria.
The initial evaluation includes a history of the timing, frequency, and nature of episodes and whether the appearance of lesions is consistent with chronic urticaria.
If lesions are painful, and persistent for more than 24 hours, or leave a bruise suggests an alternative diagnosis of vasculitis.
The diagnosis of chronic urticaria can be confirmed by provocative challenge testing, with the two most common forms of chronic inducible urticaria being dermatographia and cholinergic urticarial.
Differential diagnosis for chronic urticarial: hereditary angioedema, erythema multiforme, urticarial pigmentosa, auto inflammatory syndromes and bullous pemphigoid.
A number of factors can lower the threshold for breakthrough episodes include: alcohol, stress, opiates, and menses.
Patients should avoid nonsteroidal anti-inflammatory drugs can utilize acetaminophen as an analgesic or antipyretic medication if one is needed.
Certain complications of hives may require immediate medical attention:
Trouble Breathing
Trouble Swallowing
Joint Pain- urticarial vasculitis.
Sudden Cough
Slurred Speech
Hoarseness
Swollen Eyes
Hives After Taking Medication
Abdominal Pain or Vomiting
Treatment goal is complete remission.
Remission results in elimination of the itch-scratch dermatographism-itch feedback loop that may result in cutaneous scarring.
Non-sedating H1-antihistamines are the mainstay for treatment.
Onitial treatment consists of second generation anti-histamines, to minimize the central and peripheral side effects observed with first generation antihistamines.
To achieve control of chronic urticaria medications should be taken on a regular basis rather than as needed, until remission of chronic urticaria occurs.
Control of chronic urticaria is achieved at step one in fewer than 50% of patients.
Escalation of the dose of second generation anti-histamines up to four times dose approved by the FDA, provides satisfactory control with generally causing limited side effects.
The majority of patients with chronic idiopathic urticaria, however, do not respond to the usual doses of H1antihistamines.
For patients who do not respond to H1-antihistamines options include H2-antihistamines, leukotriene-receptor antagonists, steroids, cyclosporine, hydroxychloroquine, dapsone, methotrexate, intravenous immune globulin, and sulfasalazine: No agent, however has been specifically approved for this process.
The use of long-term steroids should be avoided.
Omalizumab, a monoclonal antibody for moderate to severe persistent allergic asthma reduces the level of free IgE and high affinity for the Fc region of the IgE which are essential for mast cell and basophil activation.
Omalizumab has efficacy in refractory chronic idiopathic urticaria (Maurer M et al).
Omalizumab Can result in complete remission in 35-53% of patients, and partial remission in up to 70% of patients with few side effects.
Ligelizumab is associated with a higher percentage of complete control of symptoms of chronic spontaneous urticaria than with omalizumab or placebo.
Studies show that after one year of treatment 35% of patients with chronic urticarial were free of symptoms, and 29% had reduced symptoms, while remission occurred in almost half of the patients with chronic spontaneous urticaria, but in only 16% of those with chronic inducible urticaria.
A prolonged duration of chronic urticaria is associated with angioedema, greater disease severity, and autoimmune thyroid disease.
