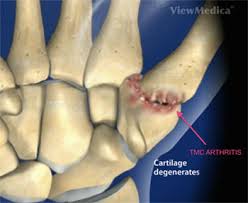
 Thumb CMC joint arthritis also known as some basal joint arthritis.
Thumb CMC joint arthritis also known as some basal joint arthritis.
The CMC joint of the thumb or the first CMC joint, also known as the trapeziometacarpal (TMC) joint, differs significantly from the other four CMC joints.
The carpometacarpal joint of the thumb (pollex), also known as the first carpometacarpal joint, or the trapeziometacarpal joint (TMC) because it connects the trapezium to the first metacarpal bone, plays an irreplaceable role in the normal functioning of the thumb.
Thumb carpometacarpal CMC) joint arthritis is characterized by progressive degenerative changes that occur within the cartilage between the trapezium and thumb metacarpal base.
These changes cause subluxation and symptomatic disability.
The most important joint connecting the wrist to the metacarpus, osteoarthritis of the TMC is a severely disabling condition; up to twenty times more common among elderly women than in average.
It is suspected ligamentous deterioration surrounding the CMC joint is the underlying pathophysiologic process.
Pronation-supination of the first metacarpal is especially important for the action of opposition.
The movements of the first CMC are limited by the shape of the joint, by the capsulo-ligamentous complex surrounding the joint, and by the balance among involved muscles.
If the first metacarpal fails to sit well ‘on the saddle’, the first CMC joint tends to be subluxated towards the radius.
Ligament disruption results in subluxation of the metacarpal base within the joint, which alters the joint mechanics and causes instability and pain.
The capsule is sufficiently slack to allow a wide range of movements and a distraction of roughly 3 mm, while reinforcing ligaments and tendons give stability to the joint.
There are three intracapsular and two extracapsular ligaments that are most important in stabilizing the thumb:
The Anterior oblique ligament (AOL) is a strong, thick, and intracapsular ligament originating on the palmar tubercle of the trapezium to be inserted on the palmar tubercle of the first metacarpal.
It is taut in abduction, extension, and pronation, and has been reported to have an important retaining functin.
It is elongated or absent in CMC joint arthritis.
the Ulnar collateral ligament (UCL) is an extracapsular ligament, located ulnarly to the AOL.
It originates on the flexor retinaculum and is inserted on the ulnopalmar tubercle of the first metacarpal.
It is taut in abduction, extension, and pronation, and often elongated in connection to CMC joint arthritis.
The First intermetacarpal ligament (IML) connects the bases of the second and first metacarpals.
IML this inserts onto the ulnopalmar tubercle of the first metacarpal where its fibers intermingle with those of the UCL.
It is taut in abduction, opposition, and supination.
It has been reported to be the most important restraining structure of the first CMC joint.
Approximate prevalence in adults is approximately 1.4%, with 0.62% in men and 2.2% in women.
For adults older than 50 years the prevalence is 8% in men and 25% in women.
Factors associated with some CMC joint arthritis include advanced stage, female sex.
6% of post menopausal women affected according to radiographic imaging results.
Approximately 20% of patients with CMC osteoarthritis require treatment.
Patient’s present with pain at the thumb metacarpal base which is exacerbated by turning, pinching, or gripping.
Diagnosis is based on history and physical exam with confirming x-rays.
Clinical exam shows tenderness to palpation around the thumb CMC joint.
In patients with severe disease there may be dorsoradial prominence of the metacarpal base because of joint subluxation, with or without a hyperextended metacarpophalangeal joint.
Clinical testing maneuvers to identify CMC joint arthritis include: axial grind test which applies axial pressure on the metacarpal while rotating it back-and-forth; and the traction shift test where traction on the metacarpal and alternating subluxation with reduction of the metacarpal base.
TREATMENT:
Early treatment is typically non-operative and includes avoiding activities that exacerbate symptoms, using tools instead of hands, modifying equipment to decrease stress with joints, oral pain medications, immobilization, and corticosteroid injections.
Splinting is associated with improved pain.
Operative management in refractory patients includes hyaluronic acid, autologous fat injection, metacarpal wedge osteotomy, arthroscopic debridement, arthroplasty, trapeziectomy with ligament reconstruction, joint fusion, and joint denervation.
All surgical interventions have similar advocacy.
Complications of surgery care in 1.3% of the patients include sensory nerve disturbances, migration of the thumb metacarpal, joint replacements are associated with implant failure and fusion operations are associated with nonunion.
