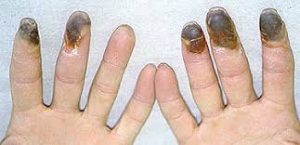
Thromboangiitis obliterans (TO) an inflammatory vasculopathy.
It is also known as Buerger’s disease.
It is characterized by an inflammatory endarteritis that causes a prothrombotic state and subsequent vaso-occlusion.
Inflammation is initiated within the tunica intima.
TO affects small and medium-sized arteries as well as veins of the upper and lower extremities.
The condition is strongly associated with heavy tobacco use.
Its progression is closely linked to continued use of smoking.
Moderate-to-severe claudication can progress to critical limb ischemia featuring rest pain or tissue loss.
Acute limb ischemia with associated pain, paresthesia, palor, mottling,coldness , paresis, and pulselessness are common signs and symptoms encountered in the emergency setting.
Pharmacologic therapy is generally ineffective in TO.
Abstinence from tobacco is the only measure known to prevent disease progression.
Because of involvement of the small and medium-sized vessels, surgical or endovascular revascularization may not be possible.
Amputation may be the only viable treatment option.
TO patients exhibit: hypersensitivity to intradermally injected tobacco extracts, increased cellular sensitivity to collagen types I and III, elevated serum anti–endothelial cell antibody titers, and impaired peripheral endothelium-dependent vasorelaxation.
A genetic component is considered with a higher prevalence of human leukocyte antigen (HLA)–A9, HLA-A54, and HLA-B5.
As the prevalence of smoking has decreased so has that of To.
Most patients with TO are aged 20-45 years.
It does not occur in pediatric or elderly patients.
TO male-to-female ratio is 3:1.
The incidence in women is increasing, as a consequence of the growing frequency of smoking among women.
The disease is relatively less common in people of northern European descent.
Natives of India, Korea, and Japan, along with Israeli Jews of Ashkenazi descent, have the highest incidence of TO..
eMedicine
Death from TO is rare.
Among patients who stop using tobacco, 94% avoid amputation.
Among patients who stop using tobacco before progression to critical limb ischemia, the amputation rate is near 0%.
Among patients who continue using tobacco, there is an 8-year amputation rate of 43%.
Thromboangiitis obliterans diagnostic criteria:
Age younger than 45 years
Current, or recent, history of tobacco use.
Presence of distal extremity ischemia; claudication, pain at rest, ischemic ulcers, or gangrene documented by noninvasive vascular testing.
Exclusion of autoimmune diseases, hypercoagulable states, and diabetes mellitus.
Exclusion of a proximal source of atheroemboli by echocardiography and arteriography.
Consistent arteriographic findings in the clinically involved and noninvolved limbs.
70-80% of patients with TO present with distal ischemic rest pain or ischemic ulcerations on the toes, feet, or fingers.
Progression of TO may lead to involvement of more proximal arteries, but involvement of large arteries is unusual.
Patients may present with claudication of the feet, legs, hands, or arms and often describe experiencing the ((Raynaud’s phenomenon)).
Late in the course patient may experience foot infections and occasionally associated sepsis.
Patients can develop painful ulcerations or gangrene of the digits.
The hands and feet of patients with the disease are usually cool and mildly edematous.
Superficial thrombophlebitis occurs in almost half of patients with TO.
With severe TO patients May experience paresthesias of numbness, tingling, burning, and hypoesthesia of the feet and hands and impaired distal pulses in the presence of normal proximal pulses.
More than 80% of patients present with involvement of three or four limbs.
Potential complications of TAO include:
Ulcerations
Gangrene
Infection
Need for amputation
Rare occlusion of coronary, renal, splenic, or mesenteric arteries
Differential diagnosis:
Acrocyanosis
Peripheral neuropathy
Ergotism
Livedo reticularis
Trauma
CREST (calcinosis cutis, Raynaud phenomenon, esophageal motility disorder, sclerodactyly, and telangiectasia) syndrome
Systemic lupus erythematosus
Rheumatoid vasculitis
Kawasaki disease
Wegener granulomatosis
Mixed connective-tissue disease
Antiphospholipid-antibody syndrome
Hyperhomocysteinemia with atherosclerosis
Popliteal artery entrapment syndrome
Repetitive vibration exposure
Hypothenar hammer syndrome
Frostbite
Giant Cell Arteritis
Polyarteritis Nodosa
Infrainguinal Occlusive Disease
Peripheral Arterial Occlusive Disease
Raynaud Phenomenon
Reflex Sympathetic Dystrophy
Scleroderma
Systemic Lupus Erythematosus (SLE)
Takayasu Arteritis
Thoracic Outlet Syndrome
Type 1 Diabetes Mellitus
Type 2 Diabetes Mellitus
No specific laboratory tests confirm or exclude the diagnosis of thromboangiitis obliterans.
TAO; also known as Buerger disease.
Arteriographic abnormalities consistent with TO are sometimes seen in limbs that are not yet clinically involved.
Arteriography of all four limbs may be required to evaluate patients with TO.
In patients thought to have TO studies should exclude a proximal source of thromboemboli or atheroemboli as the cause of distal vessel occlusion.
The primary goal of a laboratory workup in patients thought to have the disease is to exclude other disease processes in the differential diagnosis.
The hallmark angiographic findings in patients with TO are nonatherosclerotic, segmental occlusive lesions of the small and medium-sized vessels;digital, palmar, plantar, tibial, peroneal, radial, and ulnar arteries, with formation of distinctive small collateral vessels around areas of occlusion, known as corkscrew collaterals.
Corkscrew collaterals represent dilated vasa vasorum of the occluded arteries.
Corkscrew collaterals are not pathognomonic, because similar lesions can be observed in patients with scleroderma, CREST (calcinosis cutis, Raynaud phenomenon, esophageal motility disorder, sclerodactyly, and telangiectasia) syndrome, systemic lupus erythematosus, rheumatoid vasculitis, mixed connective-tissue disease, antiphospholipid-antibody syndrome, and even diabetes mellitus.
Histologically acute phase, TO is characterized by highly cellular, segmental, occlusive, inflammatory thrombi, with minimal inflammation in the walls of affected blood vessels.
Spread to contiguous veins and nerves is often observed.
A polymorphonuclear leukocyte predominant inflammatory cellular aggregate may form microabscesses and multinucleated giant cells.
In its subacute phase, intraluminal thrombosis progressively organizes.
The end-stage phase of TO is characterized by mature thrombus and vascular fibrosis.
The integrity of the normal structure of the vessel wall is maintained, distinguishing TO from arteriosclerosis and from types of systemic vasculitis, in which disruption of the internal elastic lamina and the media can be extensive.
Management: except for absolute tobacco avoidance, no forms of therapy are definitive.
Pharmacologic approaches, are for the most part, ineffective.
Surgical revascularization usually is not feasible, because of the lack of a distal target for revascularization.
Endovascular options are available.
Patients may require one or more amputations.
Pharmacologic treatment of infection or pain.
No dietary restrictions are needed.
Cardiovascular exercise is encouraged.
restricted only by symptoms.
Absolute discontinuance of tobacco use is the only strategy proven to prevent the progression of TO.
Intravenous (IV) iloprost, a prostaglandin analogue, is somewhat effective in improving symptoms, accelerating resolution of distal-extremity trophic changes, and reducing the amputation rate.
IV iloprost therapy slows progressive tissue loss and reduces the need for amputation in patients with critical limb ischemia.
Improved healing of ischemic ulcers and relief of rest pain has been associated achieved by using intramuscular gene transfer of vascular endothelial growth factor (VEGF).
NSAIDs and narcotic analgesics can be administered to palliate ischemic pain.
Antibiotics can be used to treat distal extremity ulcers.
Surgical revascularization for TO usually is not feasible because of o
Its diffuse segmental nature and the disease’s predilection for small and medium-sized arteries.
Efforts, however, should be made to improve distal arterial flow in patients with TO, y autologous vein bypass of coexistent large-vessel atherosclerotic stenoses.
Additional treatment measures,
Sympathectomy
Intra-arterial infusion of reserpine
Spinal cord stimulator implantation
Distal limb amputation for nonhealing ulcers, gangrene, or intractable pain are considered.
Autologous bone marrow–derived progenitor cell implantation into ischemic limbs for potentiation of angiogenesis has been performed as an experimental option.
Endovascular treatment of occlusive lesions have moderate- and long-term success seen in selected patients.
Percutaneous transluminal angioplasty (PTA) for the treatment of critical limb ischemia (CLI) has achieved clinical efficacy.
Prevention of complications from TO
Well-fitting protective footwear to prevent foot trauma and thermal or chemical injury
Early and aggressive treatment of extremity injuries to protect against infections.
Avoidance of cold environments
Avoidance of drugs that lead to vasoconstriction
