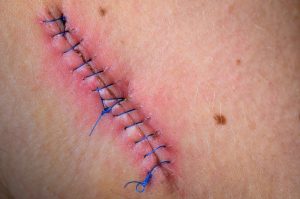
A surgical site infection is defined as infection following an operation at an incision site or adjacent to the surgical incision.
Surgical site infections affect approximately 0.5 to 3% of patients undergoing surgery and are associated with longer hospital stays than patients with no surgical site infections.
Surgical site infections occur in nearly a quarter of patients in low and middle income countries.
Microorganisms that colonize the skin are considered the major source of causative pathogens.
Classified as incisional or organ/space infections.
Incisional type infections can be classified as superficial, involving the skin or soft tissue, or deep, involving the deep soft tissues.
Surgical site, infections are categorized into three groups: superficial incisional, involving the skin or subcutaneous layers of the incision, deep incisional involving muscle, or connective tissue layers of the incision, and organs/spaces deep to the incision.
Surgical site surveillance for infection continues for 30 days for most procedures and 90 days for specific procedures involving implanted materials.
Surgical site infections are associated with delayed healing, wound dehiscence, long-term risk of hernia, longer inpatient stays, increased hospital readmissions with higher healthcare costs.
Pathogens that cause infection vary by surgical location.
In the most common pathogens are components of skin flora such a Staph aureus and Streptococcus species.
Infections following gastrointestinal procedures are typically associated with enteric organisms, such as Enterococcus species, and E. coli.
Overall S aureus is the most common cause of infection and is associated with 24% of non-superficial surgical site infections.
MRSA surgical site infections lead to worse clinical outcomes in those caused by less resistant pathogens.
E. coli and Enterococcus species respectively causes approximately 9.5% and 5.1% of all surgical site infections.
Defined as either superficial confined to the skin and subcutaneous tissue, deep involving the muscle or fascia layers, or organ space involving the internal anatomic region where the operation was performed.
Organ/space infections involve areas that are disturbed during surgery other than the incision site.
SSI occurs in up to 5% of patients following an inpatient surgical procedure.
SSIs or among the most prevalent healthcare acquired infections and occur in approximately 0.5 to 3% of patients undergoing surgery.
Surgical site infections affects up to 40% of patients after emergency laparotomy.
A surgical site infection increases the average hospital length of stay by 9.7 days, and the risk of mortality by 2-11 fold, and cause hospitalization by more than $20,000 per admission.
Surgical site infection acquisition depends on exposure to bacteria and the host’s ability to control the inevitable bacterial contamination of the incision.
SSIs are typically caused by bacteria inoculated into the surgical site at the time of surgery.
Approximately 70 to 95% of cases are caused by the patients endogenous flora.
Surgical procedures disrupt the balance between an intact immune system and the integrity of the skin and mucous membranes resulting in an increased risk of surgical site infections from endogenous flora.
Infections must occur within 30 days of surgery for incisional or organ/space infections and 1 year for infections with an implant left in place.
The median time to diagnosis of a surgical site infection varies play procedure: S aureus infection is typically diagnosed a median of 14 days after plastic surgery, 24 days at the general orthopedic surgery, and 28 days after orthopedic surgery, we are prosthetic device was inserted.
A SSI is suspected when purulent drainage is present at the incision site when there is evidence of an abscess involving the surgical bed.
Avoiding razors for hair removal, maintaining normothermia, use of chlorhexidine gluconate plus alcohol based skin preparation agents, decolonization with intranasal anti-staphylococcal agents and anti-skin antiseptics for high risk procedures, controlling perioperative glucose concentration, and using negative pressure wound therapy can reduce the rate of surgical site infections.
Physical examination, findings in SSI include systemic signs of infection with fevers, rigors, local, erythema, wound dehiscence, pain, non-purulent drainage, or induration.
Incisions through the skin disrupt the normal barrier that prevents invasion and infection of underlying tissues by allowing organisms to penetrate into areas inaccessible before the incision.
Risk of surgical site infections are dependent on the skill of the surgeon, the degree of contamination related to the surgery, and the patients status with coexisting diseases and carriage Staphylococcus aureus.
Staphylococcus aureus most prevalent SSI pathogen.
The most common organisms or staphylococcus, aureus, coagulase, negative, staphylococcus, and E.coli.
The introduction of as few as 100 colony forming units of bacteria into the surgical site can cause infection.
During surgery exaggeration sources of contamination from surgical personnel or heater/cooler units can lead to infections.
SSIs most common reason for re admission after surgery, accounting for 20% of unplanned readmissions.
A surgical site infection increases a patient’s stay by approximately 10 days and costs and additional $ 2,000.00.
Approximately 500,000 cases annually with 88,000 deaths.
Approximately 20 to 30% of such infections caused by Staphylococcus aureus and over half of these arise from endogenous flora.
Risk factors for surgical site infection include: older age, the presence of immunosuppression, obesity, diabetes, effectiveness of anti-microbial prophylaxis, surgical site tissue condition, and degree of wound contamination.
The skin and mucous membrane microbiome is the source of organisms that caused most surgical site infections.
Failure to control the microbiome is related to surgical site infections.
The goal of preventing surgical site infections is to reduce the burden of the microbiome below the infectious dose at the time of surgery.
Approach is to prevent surgical site infections include washing out any open wound, the use of perioperative antibiotics, the instilling of intranasal antibiotics or antiseptics that target Staph aureus and the application of topical anti-septics to the incision site, including alcohol solution containing either chlorhexidine gluconate or iodine povacrylex.
In a randomized clinical trial that included surgical site infections after cardiac or abdominal surgery: A povidone iodine group had 5.5% surgical siie infections and chlorhexidine gluconate group had 5.1% infections, indicating a difference between the two groups that povidone iodine was not inferior in preventing surgical side infections after cardiac or abdominal surgery (Widmer A).
Risk of surgical site infections, increased in mastectomy with obesity, and with laparoscopic cholecystectomy.
Modifiable risk factors for surgical site infections, including controlling, hyperglycemia, obesity, and tobacco use.
Most common nosocomial infection in surgical patients and the third most common nosocomial infection in hospitalized patients.
Most common preventable adverse outcome after a major surgical procedure.
SSIs after colorectal surgery, occur with rates from 15-30%.
SSIs after colorectal surgery reduces survival, increase costs, and is a leading cause of hospital readmission.
Accounts for 20% of nosocomial infections, leading cause of infections in surgical patients (38%), and the second leading cause of hospital infections.
Morbidity and mortality higher in hospitalized patients when compared to matched controls.
Associated with dehiscence, hernia, and a 2-3 times higher mortality.
If onset occurs associated an outpatient they are associated with increased outpatient visits, emergency visits and readmissions.
Patients 60% more likely to require admission to an ICU than noninfected patients and have a mortality rate of two times patients without infections.
Estimated that 40-60% of such infections are potentially preventable.
The patients endogenous flora is the most common source of infection.
May be caused by a remote infection or exogenous contamination of the surgical site.
The operative type field determines the type of flora that will be involved in infections.
Antiseptic showers before surgery significantly reduces skin flora.
Staphylococcus aureus colonization in nares of patients undergoing cardiac surgery is a major independent risk factor for SSI.
The incidence of sternal or mediastinal wound infections after cardiac surgery ranges from 0.5-3% and is associated with prolonged hospitalizations or readmission for surgical debridement and lengthy antibiotic therapy is often required.
The mortality rate of patients with sternal surgical site infections ranges from 14-42%.
Coronary artery bypass graft surgery include sternal and vascular harvest site incisions that can result in SSIs at different sites.
Vascular harvest site infections are common after CABGs surgery with a rate of 15% (Trick WE et al).
The incidence of superficial SSIs in sternotomies is approximately 2%.
The incidence of SS Is in patients undergoing CABGs has decreased in recent decades.
A trial of gentamicin-collagen sponge in a large multicenter did not demonstrate effective prophylaxis for sternal wound infections (Bennett-Guerreo E).
Surgical site infections following stoma reversal are associated with fascial dehiscence, thick subcutaneous fat, colostomy, and white race: with none of these factors there is a 0% risk of SSI and 100% with all 4 risk factors (Llang MK et al).
Staphylococcal aureus is implicated in approximately half of surgical site infections after cardiac surgery, with coagulation negative staphylococci, gram-negative bacilli and yeast organisms less frequently.
MRSA intervention programs with the use of intranasal mupirocin and patients colonized with MRSA receiving vancomycin prophylaxis has resulted in a near complete illumination of MRSA wound infections after cardiac surgery (Walsh EE et al).
Staphylococcus aureus and coagulase negative staphylococci are the leading pathogens since they are endogenous skin flora that can be introduced into the surgical site after incision.
Guidelines recommend administering 1st or 2nd generation, cephalosporin antimicrobial agents, such as Cefazolin at the time of hip or knee arthroplasty to prevent infection.
Head covering dramatically reduce airborne and wound contamination but facemasks and sterile barriers may not.
Shaving prior to surgery may increase skin trauma and exacerbate bacteria and should be discouraged.
Clipping of hair rather than shaving, maintaining normothermia, normoglycemia along with appropriate surgical technique decreases risk of SSI.
In a randomly assigned study of adults undergoing clean-contaminated surgery in six hospitals to pre-operative skin preparation waved either chlorhexidine-alcohol scrub or povidone-iodine scrub and paint: results indicated that the use of chlorhexidine-alcohol was superior to cleansing with povidone-iodine for preventing surgical site infection after cleaning-contaminated surgery(Darouiche RO).
In the chlorhexidine-alcohol vs.Povidone- iodine antisepsis indicated the former was significantly more protective against superficial, incisional infections( 4.2 vs. 8.6%), and deep incisional infections (1 vs. 3%), but not against organ space infections(Dariouche RO).
In the above study the application of chlorhexidine-alcohol reduced the risk of surgical site infection by 41% compared to aqueous povidone-iodine the most common practice.
The infection rates correlate with the time interval from shaving to surgery so that the infection rates are 20% when accomplished more than 24 hours before surgery ,7.1% when done the night before surgery, and 3.1% when done in the operating room.
Tight perioperative glucose control results in lowered risk of SSI’s in diabetics.
Postoperative hyperglycemia is associated with increased risk of surgical sight infections in patients with and without diabetes.
Preventive strategies for surgical site infections, include preventing hyperglycemia.
Continuous infusions of intravenous insulin associated with decreased risk of cardiovascular surgical site infections indicating tighter control lowers rates of deep sternal wound infection.
Surgical Infection Prevention Project and the Surgical Care Improvement Project recommend initial administration of perioperative antibiotics within one hour prior to surgery, they use of preoperative hair clippers or no hair removal, and the maintenance of normothermia during surgery(Bratzler DW).
Removing hair with a razor is associated with an increased risk of surgical site infections.
Hair removal with clippers does not increase the risk of surgical site infection.
In a study combining perioperative warming, high intraoperative oxygen delivery, avoidance of preoperative mechanical bowel preparation, intraoperative fluid restriction, and use of a surgical wound protector did not reduce the rate of SSIs, and in fact had higher rates 45% vs. 24%, respectively (Anthony T et al).
SSIs can be reduced by decolonization in which patients are treated with intranasal antimicrobial, skin anti-septic agent, or both to eliminate or temporary reduce S aureus colonization prior to surgery.
Decolonization is typically focused on orthopedic, cardio, thoracic, or high risk procedures, such as spine and brain surgeries.
Prevention measures for SSI includes: IV antibiotics within 30 minutes of colorectal surgery, use of ertapenem, preop bowel surgery with oral antibiotics, chlorhexidine with alcohol skin prep, normoglycemia, intra operative normothermia, smoking cessation, improve nutrition, lap surgery rather than open surgery.
Guideline recommendations to reduce SSI: parenteral anti-microbial prophylaxis, alcohol-based skin preparation, perioperative glycemic control, temperature regulation to normothermia, and maintenance of normal tissue oxygenation.
Guidelines recommend that surgical site antisepsis should be performed with a product that contains alcohol and another anti-septic agent – chlorhexidine gluconate or povidone iodine: the combination of two topical agents is associated with lower rates of infection than either agent alone.
Alcohol provides no residual activity after application, whereas iodophor and chlorhexedine exhibit prolonged bacthermostatic activity on the skin.
Recommendations are for the discontinuation of prophylactic antibiotics after skin closure in patients at low risk for surgical site infection.
Additional recommendations include preop bowel preparations, the use of care bundles, and the application of negative pressure wound dressings.
Incisional negative pressure wound therapy-wound dressing systems that continuously or intermittently apply subatmospheric pressure to the system, can reduce the risk of surgical site infection by promoting reduction in fluid accumulation in the wounds and accelerating primary wound healing.
The widespread use of antistaphyloccal antibiotics, such as mupirocin may ultimately increase the rates of resistance to Staph aureus infections
Surgical-site infection (SSI) after total joint arthroplasty (TJA) continues to pose a challenge and place a substantial burden on patients, surgeons, and the healthcare system.
Estimated 1.0% to 2.5% annual incidence of surgical-site infection after total joint arthroplasty.
Advances in surgical technique, sterile protocol, and operative procedures have minimized SSIs.
In contrast to postoperative glucose control no randomized control studies have found a clear association between a specific hemoglobin A1c cutoff and surgical side infections.
Preoperative skin preparation have shown varying outcomes after TJA.
Preoperative antibiotic guidelines are that they should be given within 60 minutes of the incision to maximize tissue concentration of the antibiotic.
The duration of prophylactic antibiotics is not known, and prolonged antimicrobial prophylaxis can increase patient harm.
Guidelines recommend stopping prophylactic antibiotics when the surgical wound is closed.
Preoperative patient optimization of nutritional status, immune function, and metabolic control are essential to prevent infection.
Intraoperative infection prevention measures include: skin preparation, gloving, surgical drapes, OR staff traffic and ventilation flow, and antibiotic-loaded cement.
Revision procedures for infection after total hip arthroplasty are associated with more hospitalizations, more operations, longer hospital stay, and higher outpatient costs in comparison with primary total hip replacement or revision surgeries for aseptic loosening.
SSI that develops into a periprosthetic infection, can be disastrous.
Recommendations are that surgical site infection control by identifying high volume, high risk procedures, and implementing a system for collecting and storing data with periodic reports, with provision of education can reduce surgical site infections.
