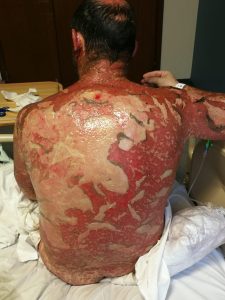
 Both are rare and can be a medical emergency.
Both are rare and can be a medical emergency.
Caused by the same medications and have essentially identical histologic findings.
Distinguished by proportion of the body-surface area that it affected.
The Stevens-Johnson syndrome diagnosis is made when skin eruptions cover 30% or less of the body surface area.
The diagnosis of Toxic Epidermal Necrolysis is made when more than 50% of the body surface area is involved.
Stevens-Johnson syndrome-Toxic Epidermal Necrolysis overlap refers to disease that involves 30-50% of the body surface area.
Skin sloughing occurs in less than 10% of the body surface area with Stevens-Johnson syndrome, and in greater than 30% in toxic epidermal necrolysis.
Most common drugs are antibiotics, anticonvulsants, no steroidal anti-inflammatory agents and allopurinol.
Skin eruptions are preceded by fever and influenza like symptoms for a few days, with a macular erythematous rash with atypical target lesions usually staring on the face and trunk and progressing rapidly to involve the trunk and mucosal surfaces.
Following the above bullae formation occurs and subsequent desquamation.
May be associated with hydroxychloroquine.
Carbamzine induced SJ Sx and toxic epidermal necrolysis associated with HLA-B15:01 and HLA-31-01.
