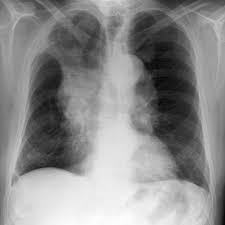
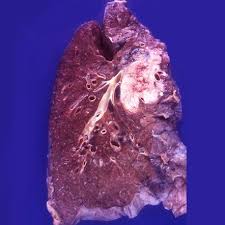
 Most often centrally located. Non-Small Cell Carcinoma of the Lung (NSCLC).
Most often centrally located. Non-Small Cell Carcinoma of the Lung (NSCLC).
Tends to occur centrally near a bronchus.
Associated with smoking and derived from bronchial epithelial cells.
Most express high molecular weight keratin, CK 5 and CK 6 but do not express TTF-1.
p63 is a marker of squamous differentiation.
Patients with squamous cell carcinoma are unlikely to have EGFR mutations and testing in this population is not recommended.
Histopathology shows keratinization or intracellular bridges.
Most commonly shows infiltrating malignant squamous cells with central necrosis and often cavitation.
Squamous-cell carcinoma of the lung
It is the second most prevalent type of lung cancer after lung adenocarcinoma and it originates in the bronchi.
Its tumor cells are characterized by a squamous appearance, similar to the one observed in epidermal cells.
Squamous-cell carcinoma of the lung is strongly associated with tobacco smoking, more than any other forms of NSCLC.
Squamous-cell lung carcinoma share most of the signs and symptoms with other forms of lung cancer.
These include worsening cough, including hemoptysis, chest pain, shortness of breath and weight loss.
Symptoms may result from local invasion or compression of adjacent thoracic structures such as compression involving the esophagus causing dysphagia, compression involving the laryngeal nerves causing change in voice, or compression involving the superior vena cava causing facial edema.
Distant metastases may also cause pain and show symptoms related to other organs.
Squamous-cell carcinoma of the lung is closely correlated with a history of tobacco smoking: Nurses’ Health Study, the relative risk of SCC is approximately 5.5, both among those with a previous duration of smoking of 1 to 20 years, and those with 20 to 30 years, compared to never-smokers.
The relative risk increases to approximately 16 with a previous smoking duration of 30 to 40 years, and approximately 22 with more than 40 years.
It most often arises centrally in larger bronchi.
It often metastasizes to locoregional lymph nodes, particularly the hilar nodes, early in its course, and generally disseminates outside the thorax somewhat later than other major types of lung cancer.
Large tumors may undergo central necrosis, resulting in cavitation.
A squamous-cell carcinoma is often preceded for years by squamous-cell metaplasia or dysplasia in the respiratory epithelium of the bronchi, which later transforms to carcinoma in situ.
Squamous-cell lung carcinoma is one of the tumor types with the highest number of mutations since smoking, the main driver of the disease, is a strong mutagenic factor.
Inactivating mutations in lung SCC affect many tumor suppressor genes such as TP53 (mutated in 81% of cases), MLL2 (20%), CDKN2A (15%), KEAP1 (12%) and PTEN (8%).
Recurrent loss-of-function mutations have been observed also in NOTCH1 (8%), suggesting a tumor suppressive role in lung SCC for this gene.
Recurrent gain-of-function mutations have been found in oncogenes such as PIK3CA (16%) and NFE2L2 (15%).
Common oncogene copy number amplifications have been found in SOX2, PDGFRA, EGFR, FGFR1 and CCND1.
Deletions were observed in tumor suppressors such as CDKN2A, PTEN and NF1.
Some alterations such as the ones affecting TP53 and CDKN2A are shared by lung SCC and the other most common type of NSCLC, lung adenocarcinoma.
Conversely, the two main driver oncogenes of the latter, EGFR and KRAS, are rarely mutated in lung SCC.
Many gene mutations and copy number alterations occur in pathways whose deregulation seems to be important for the initiation and progression of the tumor.
KEAP1 and NFE2L2 belong to the oxidative stress response pathways, and alterations in these genes tend to occur in a mutually exclusive fashion.
The oxidative stress response pathways, is overall altered in more than 30% of the cases.
The squamous cell differentiation pathway, whose components include SOX2, TP63 and NOTCH1, is altered in 44% of the tumors.
Alterations in the receptor tyrosine kinase pathway are also common but not as widespread as for the adenocarcinoma type.
Four mRNA expression subtypes (primitive, basal, secretory, and classical) within squamous-cell carcinoma correlates with worse patient survival.
Diagnosis
Early squamous-cell carcinoma of the lung (squamous-cell carcinoma in situ) is asymptomatic and may only appear as an incidental imaging finding on CT scan or a lung biopsy.
Squamous tumors range from well differentiated, showing keratin pearls and cell junctions, to anaplastic, with only minimal residual squamous-cell features.
Squamous cell lung carcinomas into 3 categories: keratinizing, non-keratinizing and basaloid.
Keratinizing SCC harbor features of keratinization; non-keratinizing SCC lack such features but show other squamous markers, such as p40 and p63.
Basaloid SCC is a rare subset of poorly differentiated squamous cell lung carcinoma.
There is no clear evidence of prognostic significance to the subtyping of lung squamous cell carcinoma.
Treatment
Treatment of lung squamous-cell carcinoma depends on many factors including stage, resectability, performance status and genomic alterations acquired by the individual tumor.
Early stage (I, II and IIIA) lung SCC are typically resected surgically, and cytotoxic chemotherapy and/or radiation may be used as an adjuvant therapy following surgery.
Advanced, metastatic or recurrent lung SCC are given first-line systemic therapy with a palliative intent consisting of cytotoxic chemotherapy, most commonly a platinum-based doublet.
Either cisplatin or carboplatin is used as the platinum backbone.
Targeted therapies has been less rapid for lung SCC with respect to adenocarcinoma, as ALK rearrangements and EGFR mutations targetable with receptor tyrosine kinase inhibitors are much less frequent in the former compared to the latter.
Immunotherapy is showing promising results for NSCLC, and anti-PD-1 have been approved by the US Food and Drug Administration (FDA) for lung SCC.
Lung squamous-cell carcinoma is the second most common histologic type of lung cancer after adenocarcinoma.
The relative incidence of the former has been steadily decreasing in favor of the latter due to the decreasing smoking rates in the last few years.
As much as 91% of lung SCC has been found to be attributable to cigarette smoking. Incidence is greater in men than in women.
Combination of pemetrexedand cis-platinum have poorer overall survival compared with gemcitabine and Cisplatin in patients with squamous cell lung cancer with the median overall survival of 9.4 months versus 10.8 miles, respectively.
Nivolumab is approved for treatment of patients with metastatic squamous cell carcinoma of the lung who progressed on or after platinum based chemotherapy.
In a study of randomly assigned 272 patients to receive Nivolumab at a dose of 3 mg/kg every 2 weeks or docetaxel every 3 weeks: Among previously treated squamous cell NSCLC overall survival, response rates, progression free survival were significantly better with Nivolumab, regardless of PD-L1 expression level.
In the above study the overall one year survival rate was 42% with Nivolumab versus 24% with docetaxel.
In the above study nivolumab response rate was 20% versus 9% with docetaxel.
Necitumumab (Portrazza)-SQUIRE trial, conducted in 1093 patients, which showed a 1.6-month improvement in overall survival (OS) when necitumumab was added to a regimen of gemecitabine and cisplatin. The median OS was 11.5 months, compared with 9.9 months on the doublet of gemcitabine and cisplatin.
In the phase three KEYNOTE-407 study on squamous NSCLC, chemotherapy with pembrolizumab had a significantly longer overall survival and progression severe free survival than with chemo therapy alone.
Bevacizumab, an antibodiy to the vascular endothelial growth factor, is contraindicated in patients with squamous cell carcinoma of the lung because there is a higher risk of fatal or life threatening hemoptysis.
