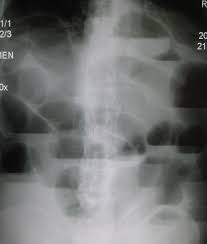
 Leading cause is postoperative adhesions.
Leading cause is postoperative adhesions.
Accounts for approximately 20% of all acute surgical admissions.
The incidence increases with the number of laparotomy is performed.
Incarcerated groin hernias are the second most common cause.
Malignant tumors make up approximately 20% of cases, hernias 10%, inflammatory bowel disease 5%, volvulus 3% and miscellaneous causes 2%.
In pediatric patients SBO may be related to congenital abnormalities, intussusception and pyloric stenosis.
Procedures most closely associated with SBO are appendectomy, colorectal surgery, gynecologic surgery and upper gastrointestinal surgical procedures.
Pelvic and lower abdominal procedures lead to SBO more often than do upper gastrointestinal procedures.
Classified as: partial, complete, strangulated or nonstrangulated.
Strangulated SBOs require emergency correction to prevent vascular compromise and bowel ischemia.
About 40% of patients have strangulated SBOs.
Strangulated lesions are most commonly associated with adhesions with the bowel twisting on its mesenteric pedicle with arterial occlusion leading to bowel ischemia and necrosis.
Strangulation, if unattended leads to bowel peroration with peritonitis and risk of death.
Untreated strangulation is associated with 100% mortality.
Surgery for strangulated SBO if performed within 36 hours the mortality rate is 8%, and up to 25% if the procedure is performed beyond 36 hours.
SBO associated with dilation of the proximal intestine with accumulation of intestinal secretions and air.
Bowel obstruction leads to increased fluid secretion and accumulation with increasing peristalsis above and below the obstruction.
Early in the course of SBO increased loose stool frequency and flatus may occur.
With proximal small bowel obstruction vomiting may occur.
Bowel distension can compress mucosal lymphatics with resulting lymphedema of the bowel wall.
As intraluminal bowel hydrostatic pressure increases, it increases the hydrostatic pressure in the capillary beds causing third spacing of fluid, electrolytes and proteins into the intestinal lumen.
Intraluminal accumulation of fluid may lead to dehydration with secondary complications.
Bacterial proliferation occur in the proximal and increase the risk of bacteremia with E. coli.
Most patients present with abdominal pain, which is cramping in nature and intermittent.
Abdominal pain, more common in simple obstruction.
Colicky pain of short duration and associated with bilious vomiting suggests a proximal lesion.
Distal obstruction is suggested by pain lasting several days and which is progressive in nature and with increasing abdominal distention.
The onset of chronic pain indicates progressive difficulties associated with a strangulated bowel with ischemia.
Patients frequently have nausea, vomiting, diarrhea, constipation, fever, tachycardia, and previous history of abdominal or pelvic surgery, previous radiation, and a previous history of malignancy.
Duodenal and proximal SBO associated with less abdominal distention than when the obstruction is in the distal bowel.
Early in the process hyperactive bowel sounds occur in an attempt to overcome the obstruction, and hypo-active bowel sounds occur later.
Evaluation includes, excluding hernias of the groin, femoral triangle, and obturator foramina.
Pelvic and rectal examinations are essential in the evaluation of such patients.
The presence of fever, tachycardia and peritoneal signs suggest complications and intestinal ischemia.
Serial abdominal examinations are necessary for proper evaluation.
Small bowel obstruction is a medical emergency that involves blockage in the small intestine.
Immediate medical attention is necessary.
Management of small bowel obstruction typically involves: a physical examination, diagnostic tests, such as X-rays, CT scans, or ultrasounds, to confirm the diagnosis and determine the severity and location of the obstruction.
Patients with small bowel obstruction are usually instructed to take nothing by mouth (NPO).
Intravenous fluids are required to maintain hydration and electrolyte balance, fluids may be administered intravenously.
A nasogastric tube may be inserted through the nose into the stomach to decompress it and relieve pressure.
Hospitalization is often required for close monitoring to assess if the obstruction can resolve on its own or if surgery is necessary.
If the obstruction doesn’t resolve with conservative measures or if complications like ischemia or perforation occur, surgery may be required.
