Skin cancers is most common of all cancers.
One in five Americans will have skin cancer in their lifetime.
Skin cancers is the most common cancers in White population, and the risks include: ultraviolet radiation, leading to cutaneous carcinogenesis by inducing genetic damage, suppressing antitumor immune responses, and depleting cellular ATP, thereby inhibiting DNA repair.
Annual cost for skin cancer care is estimated at $8.1 billion.
UVB is the major contributing factor.
One-in-five lifetime risk of having skin cancer.
More than 3.5 million cases of basal and squamous cell cancer are diagnosed each year.
90% of all lesions are directly related to UV radiation.
Skin cancer is less common in people with darker skin tones, but when such cancers do occur they may be more aggressive, possibly because of latest stage diagnosis.
1 million new cases of basal cell carcinomas and squamous cell carcinomas diagnosed each year.
An estimated 186-420,000 cases of dermally invasive cutaneous squamous cell carcinoma are diagnosed annually in the US.
The greatest mortality from skin cancers is among transplant recipients because of their immunosuppression.
Women with history a non-melanoma skin cancer have more than 2 times risk of having a second tumor compared the women without a history of skin cancer.
Presents as an erythematous papule, plaque, or nodule on sun-exposed skin.
Black women with non-melanoma skin cancer have a greater than 7-fold increase risk of a second malignancy than black women without a skin cancer.
Regular sunscreen use prevents cutaneous squamous cell carcinoma and melanoma (Robinson JK et al)
Immunosuppressed patients commonly have cutaneous cancers in sun exposed skin that are more aggressive than similar lesions in non-immunosuppressed patients.
In basal cell cancers of the skin mutations in the tumor suppressor PTCH gene system found on chromosome 9q are frequent.
In cutaneous squamous cell carcinoma mutations in the tumor suppressor gene p53 is a common event.
Genetic syndromes that predispose individuals to skin cancer include albinism, xeroderma pigmentosum and nevoid basal cell carcinoma syndrome.
More then 95% of basal and squamous cell cancers involve only local disease.
Clinical risk factors for basal and squamous cell cancers include tumor location, size, status of tumor borders, whether the tumor is a primary lesion or a recurrent one, the presence of immunosuppression, and cancers developing in previously irradiated sites.
Skin cancers, squamous cell or basal cell, that developed in the region of the head and neck have higher recurrence rates than lesions developing on the trunk and extremities.
Squamous cell cancers involving the genitalia, mucosa, and the ear are at greater risk of metastasizing then similar cancers from other sites.
In the estimated 186-420,000 cases of dermally invasive cutaneous squamous cell carcinoma are diagnosed annually in the US.
Lesions greater than 2 cm in diameter are associated with increased risk of recurrence for squamous cell cancers.
For basal cell cancers high risk sites for recurrence correspond to the mask areas of the face.
For basal cell cancers recurrences are significantly more common when tumors in high-risk locations are 6 mm or more in diameter and when the tumors in middle risk locations are 10 mm or more in diameter.
Patients are at significant risk for development of squamous cell skin cancers when they are immunosuppressed, such as with organ transplantation or with the long-term use of psoralen and ultraviolet A light (PUVA).
Patients on immunosuppressive drugs have a greater likelihood of having metastatic squamous cell disease, suggesting more aggressive tumor behavior.
Perineural involvement is associated with increased risk of recurrence for basal or squamous cell carcinoma and increased risk of metastases for squamous cell cancers.
Patients with well differentiated tumors have a better prognosis than those with poorly differentiated lesions.
Young age does not appear to be a clinically negative risk factor for skin cancers.
Increased rates of metastases occur for cutaneous squamous cell cancers that arise in areas of chronic scarring.
Skin cancers with perineural involvement may be associated with pain, burning, paresthesias, facial paralysis, diplopia and blurred vision.
Skin cancers with desmoplastic cutaneous squamous cell cancer have increased risk for recurrence and metastases.
The use of oral retinoids may be effective in reducing the development of precancerous and skin cancers in patients with high risk disease.
Skin biopsy of suspected lesions should include deep reticular dermis tissue if the lesion is suspect to be more than a superficial one.
Basal and squamous cell cancers of the skin are most commonly treated with surgery or radiation therapy.
Surgical techniques include: curretage and electrodisiccation, excision with postoperative assessment of surgical margins, Mohs surgery and excision with complete circumferential peripheral and deep margin evaluation.
Curettage and electro-dissection are effective for low risk tumors, but should not be used in hair bearing sites, or If subcutaneous layer is reached with the technique, as both of these features may be associated with residual cancer cells.
Excision with postoperative margin assessment for basal or squamous cell tumors less than 2 cm in diameter with a 4 mm clinical margin should result in complete removal of such lesions.
Excision with postoperative margin assessment for basal and squamous cell carcinoma is can also be utilized for re-excision of low risk primary lesions of the trunk and extremities, if positive margins were seeing after the initial excision with post operative margin assessment and for the primary removal of larger tumors located in the trunk and extremities.
Mohs surgery or excision with complete circumferential peripheral and deep margin assessment is recommended for all high-risk tumors-using intraoperative frozen section assessment.
Radiation is an option for nonsurgical candidates utilizing orthovoltage x-ray or electron beam.
Electron beam therapy requires fields that are wider than that with orthovoltage.
Nicotinamide (Vitamin B3) can decrease the rate of development of basal and and squamous cell cancers of the skin by a significant amount in individuals with prior skin cancers (Damian D.
The presence of HPV was strongly correlated with non-melanoma skin cancers.
Ultraviolet radiation, as well as immunosuppression, lead to skin cancer, and that chronically sun-exposed skin is more likely to have HPV.
75% of tested non-melanoma skin cancer biopsies exhibited at least one of three viruses: HPV, Merkel cell polyomavirus, and Epstein-Barr virus(Baez et al).
Only 38% of non-cancerous skin biopsies, however, positive for these viruses.
HPV detection was common in non-melanoma skin cancers, 43%, but was nearly absent in non-cancerous biopsies.
Furthermore, Merkel cell polyomavirus is correlated with sites of increased exposure to ultraviolet radiation.
Epstein-Barr virus is significantly linked to immunocompromise.
Ultimately, HPV was strongly associated with non-melanoma skin cancer, while Epstein-Barr virus and Merkel cell polyomavirus were associated with other risk factors.
It is suggested that oncogenic viruses may play a role in non-melanoma skin cancers.
Multiple studies have shown a correlation between viruses and non-melanoma skin cancer, particularly HPV, squamous cell carcinoma, and basal cell carcinoma.
HPV vaccine is available for the prevention of cervical cancer, and this vaccine could possibly decrease non-melanoma skin cancer development in at-risk populations.
Increased intake of dietary vitamin A is associated with decreased risk of incident cutaneous squamous cell carcinoma.
Vitamin A is essential for the healthy growth and maturation of skin cells.
Eating a healthy diet rich in vitamin A may reduce risk of getting squamous cell skin cancer.
The diet and skin cancer results of participants in 2 large, long-term observational studies: the Nurses’ Health Study, which followed 121,700 women from 1984 to 2012, and the Health Professionals Follow-Up Study, which followed 51,529 men from 1986 to 2012 (Kim J).
Higher total vitamin A was associated with a reduction in squamous cell carcinoma risk.
Higher intakes of retinol and some carotenoids are associated with a reduction in squamous cell carcinoma risk.
The majority of vitamin A came from the participants’ diets, particularly from fruits and vegetables.
Treatment and Clinical Pathways for Skin Cancer
There are more diagnoses of skin cancer than all other cancers combined.
Skin cancer cases are increasing, in particular for basal cell carcinoma (BCC) and squamous cell carcinoma (SCC), due to increased awareness of disease but also due to UV exposure.
BCC alone is the most common cancer in the United States, with an estimated 2 million people diagnosed per year.
SCC is the second most common, with half the incidence.
In immunocompromised patients, BCC is at least three times more common than SCC.
Localized SCC is highly curable, at a rate of 95% for patients in the early stages.
Death from Nonmelanoma skin cancers account for less than 0.1% of all cancer deaths.
Deaths from BCC and SCC range from 2000 to more than 15,000 each year in the United States.
Individuals most vulnerable to BCC and SCC are the elderly patients with a delayed diagnosis or are immunocompromised, including those with organ transplants.
Merkel cell carcinoma (MCC) cases are around 2488 cases per year, and has increased its incidence by about 2.5-fold over 10 years, 3-fold over 15 years, and 5.4-fold over 18 years.
Merkel cell carcinoma increased incidence is attributed to an aging population.
Merkel cell carcinoma is a more aggressive cancer than other types of nonmelanoma skin cancers, with rapid growth and early metastases.
Prior to diagnosis, 63% of the primary lesions grew rapidly in the preceding 3 months.
26% to 36% of cases have lymph node involvement on presentation, with up to half eventually developing metastases.
A smaller portion, 6% to 16%, have distant metastases on presentation, with up to one-third subsequently spreading.
Approximately 25% to 50% of patients with MCC experience disease recurrence.
Depending on the stage at presentation, the 5-year specific survival rates are 41% to 77%.
For patients with MCC who receive chemotherapy, prognosis is poor, with about 10% surviving 3 years after systemic treatment initiation.
It is estimated that 96,480 new cases of melanoma will be diagnosed in 2019, with about 7230 patients dying of melanoma in the Unites States in the same year.
Melanoma incidence continues to increase dramatically, with rates increasing in men more rapidly than any other malignancy and in women more rapidly than any other malignancy expect lung cancer.
It is estimated that 84% of patients with melanoma initially present with localized disease, 9% with regional disease, and 4% with distant metastatic disease.
Prognosis is good for patients with localized disease or smaller primary tumors of 1.00-mm thickness or less: with more than 90% of patients achieving 5-year survival.
With larger tumors (>1.0-mm thickness), survival ranges from 50% to 90%, depending on tumor thickness, ulceration, and mitotic rate.
When regional nodes are involved, survival rates are roughly halved.
Long-term survival in patients with distant metastatic melanoma has historically been less than 10%, although the emergence of effective immunotherapy has made long-term remission possible for a larger proportion of patients.
NCCN Guidelines for Cutaneous Melanoma, patients with stage 0, stage 1, or stage 2 disease should have the cancer removed by wide excision, with or without sentinel nodel biopsy.
If node positive, patients should undergo nodal basin ultrasound surveillance or complete lymph node dissection.
Adjuvant treatment include systemic therapy with the following preferred regimens: novolumab, pembrolizumab, or dabrafenib/trametinib for patients with BRAF V600-activating mutation.
Both nivolumab and pembrolizumab have shown clinically significant improvement in relapse-free survival compared with ipilimumab, though their impact on overall survival has not yet been reported.
Patients with clinically positive nodes should undergo wide excision of the primary tumor as well as complete therapeutic lymph node dissection.
Radiation therapy to the nodel basin may be considered as an option in selected high-risk patients, based on location, size, and number of involved nodes.
Options for systemic therapy include novolumab, pembrolizumab, or dabrafenib/trametinib for patients with BRAF V600-activating mutation.
First-line systemic therapy options for metastatic or unresectable disease include anti-PD-1 monotherapy (pembrolizumab or nivolumab) or combination targeted therapy if the patient has BRAF V600-activitating mutation (dabrafenib/trametinib, vemurafenib/cobimetinib, or encorafenib/binimetinib).
Local therapy options include: surgical excision; intralesional injection with talimogene laherparepvec (T-VEC), Bacillus Calmette-Guerin, interferon, or IL-2; topical imiquimod for superficial dermal lesions; or radiation therapy for unresectable disease.
Regional therapy would consist of isolated limb infusion/perfusion with melphalan.
Basal cell carcinoma patients who have low risk of recurrence could have the cancer removed by electrodesiccation and curettage, with no adjuvant treatment.
Basal cell carcinoma patients who have low risk of recurrence could also be excised surgically with 4-mm clinical margins and a postoperative margin assessment.
Negative margins : would be no adjuvant treatment.
Positive margins: the patient could receive an additional excision or undergo Mohs micrographic surgery.
Patients who are not surgical candidates may receive radiation treatment.
For those with high-risk BCC, the NCCN Guidelines recommend patients receive Mohs surgery with complete circumferential margin assessment.
If margins are positive, the patient would receive radiation therapy.
If negative, adjuvant treatment of radiation therapy would only be considered if there were extensive perineural involvement.
Those with positive margins who were treated with Mohs surgery or resection and have residual disease present, but for whom additional surgery and radiation therapy are contraindicated, should receive possible systemic treatment with Hedgehog pathway inhibitors (vismodegib or sonidegib).
Other treatment options appropriate for early stage BCC, include cryosurgery, photodynamic therapy, and medicated creams (such as imiquimod or 5-fluorouracil).
Those with at least one BCC lesion are at higher risk for developing others.
Lesions on the nose and scalp typically recur within 2 years after surgery.
BCCs that are diagnosed and treated early are usually cured.
Patients with metastases or nodal involvement could receive radiation therapy, surgery, and potential treatment with a Hedgehog inhibitor, or enter a clinical trial.
For local squamous cell carcinoma (SCC), the patient should undergo a standard excision with 4 to 6 mm clinical margins and a postoperative margin assessment, as recommended by the NCCN Guidelines for SCC.
If margins are negative, no further treatment is indicated.
If margins are positive, the patient should undergo Mohs micrographic surgery with complete circumferential margin assessment or radiation therapy for non-surgical candidates.
Alternatively, the patient could also undergo electrodesiccation and curettage, with no adjuvant treatment.
With local high-risk SCC should undergo Mohs surgery or resection with complete circumferential margin assessment.
If margins are positive, the patient should receive adjuvant radiation therapy.
If margins are negative but there is extensive paraneural or large nerve involvement, adjuvant radiation therapy is advised.
Patients can have standard excision with wider surgical margins and a postoperative margin assessment.
Those with negative margins would receive adjuvant radiation if extensive paraneural or large nerve involvement.
Positive margins would lead to a Mohs surgery with complete circumferential margin assessment or radiation therapy, or re-excision if clinically feasible.
If the patient is a nonsurgical candidate for initial excision or Mohs surgery, then radiation therapy with or without systemic therapy is advised.
Operable disease in the head and neck would involve tumor excision and indicated nodes, as well as radiation therapy, observation, and concurrent systemic therapy.
Inoperable disease would lead to radiation therapy with or without
systemic therapy to radiation or clinical trial.
Treating local recurrence would be the same as an initial local treatment.
Cemiplimab may be considered as a systemic therapy option for patients with locally advanced or metastatic cutaneous SCC who are not surgical or radiation therapy candidates.
Adjuvant cemiplimab therapy led to to longer disease free survival than placebo among patients at high risk for recurrence of cutaneous squamous cell carcinoma.
Merkel cell carcinoma treatment depends on the histopathological interpretation and microstaging of the primary lesion and regional disease.
A wide excision of the primary tumor and adjuvant radiation therapy at the tumor site, or observation, for negative sentinel nodal disease.
If sentinel nodal disease is identified in Merkel cell carcinoma patients should receive a node dissection and/or radiation therapy to the nodal basin.
For regional disease, preferred systemic therapy may be useful, as well as immunotherapy with avelumab, pembrolizumab, or nivolumab.
Chemotherapy is indicated if the patient is immunocompromised or checkpoint immunotherapy is contraindicated.
MCC often recurs within 6 to 12 months after diagnosis.
Pembrolizumab or other immune checkpoint inhibitors, may be considered for patients with recurrent locally advanced or metastatic MCC, most often those with weakened immune systems and older people.
Standard of care is now to use the immune checkpoint inhibitors as first-line treatment, instead of chemotherapy.
A sustained response is 10 times greater for immunotherapy if given before chemotherapy.
Organ transplant patients suffer disproportionately from squamous cell cancer.

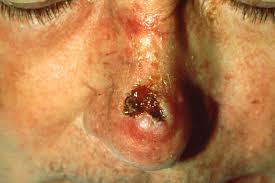 See cutaneous cell squamous cell carcinoma
See cutaneous cell squamous cell carcinoma