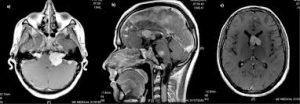
Reversible cerebral vasoconstriction syndrome (RCVS), is a disease characterized by a weeks-long course of thunderclap headaches, sometimes focal neurologic signs, and occasionally seizures.
The average age of onset is 42, but has been observed in patients aged from 19 months to 70 years.
These headaches are typically bilateral, very severe and peak in intensity within a minute.
Headaches may last from minutes to days, and may be accompanied by nausea, photophobia, phonophobia or vomiting.
Symptoms are thought to arise from transient abnormalities in the blood vessels of the brain.
Some patients have only one headache.
On average there are four attacks over a period of one to four weeks.
A milder, residual headache persists between severe attacks for half of patients.
It may be associated with childbirth, vasoactive or illicit drug use, or complications of pregnancy.
After delivery it is referred to as postpartum cerebral angiopathy.
Usually, symptoms disappear on their own within three weeks.
Deficits may persist in a small minority of patients.
Severe complications or death are very rare.
The key symptom of RCVS is recurrent thunderclap headaches.
Over 95% of patients experience recurrent headaches.
In two-thirds of cases, it is the only symptom of RCVS.
CSF Analysis is normal.
Associated with reversible vasospasm.
Angiography reveals cerebral artery vasoconstriction, with or without focal neurologic signs.
Reversibility of angiogram findings on removal of the trigger factor or after vasodilator therapy should be evident within 12 weeks of onset.
Autonomic in balance resulting in exaggerated sympathetic cerebral vascular tone is hypothesized as the pathophysiology.
The process is underdiagnosed.
Possible triggers include: drugs, hormones, but 50% are idiopathic.
Young adults between ages 20 and 50 years and most commonly affected.
Women are more than twice as likely to be affected than men.
No randomized trial has examed the effectiveness of any treatment.
Calcium channel antagonists are thought to be most effective in reducing the severity of headaches.
8–43% of patients show neurologic problems.
Such neurologic problems include: visual disturbances, hemiplegia, ataxia, dysarthria, aphasia, and numbness.
Patients may experience seizures (1-17%).
Typically, neurologic issues typically disappear within minutes or a few hours.
I these patients cerebral arteries can spontaneously constrict and relax back and forth over a period of time without intervention and without clinical findings.
Vasospasm is common post subarachnoid hemorrhage and cerebral aneurysm, but in RCVS only 25% of patients have symptoms post subarachnoid hemorrhage.
As many as two-thirds of RCVS cases are associated with an underlying condition or exposure of vasoactive or recreational drug use, or complications of pregnancy and the puerperium.
Vasoactive drug use is found in about 50% of cases of RCVS: selective serotonin reuptake inhibitors, weight-loss pills, alpha-sympathomimetic decongestants, acute migraine medications, pseudoephedrine, epinephrine, cocaine, and cannabis.
RCVS can follow blood transfusions, surgical procedures, swimming, bathing, high altitude experiences, sexual activity, exercise, coughing, SSRIs, uncontrolled hypertension, endocrine abnormality, and neurosurgical trauma.
Symptoms can take days or a few months to manifest after a trigger.
Differential diagnosis: subarachnoid hemorrhage, ischemic stroke, pituitary apoplexy, cerebral artery dissection, meningitis, spontaneous cerebrospinal fluid leak, posterior reversible encephalopathy syndrome.
Evaluation includes: CT scan, lumbar puncture, MRI, and other tests.
Posterior reversible encephalopathy syndrome os found in 10–38% of RCVS patients.
RCVS is diagnosed by detecting diffuse reversible cerebral vasoconstriction, by catheter angiography.
Computed tomography angiography and magnetic resonance angiography can identify about 70% of cases.
Multiple angiographic studies may be necessary, as it can only be conclusively diagnosed if vasoconstriction resolves within 12 weeks.
While all symptoms normally resolve within three weeks, and may only last days, permanent deficits are seen in a minority of patients, ranging from under 10% to 20%.
Fewer than 5% of patients experience progressive vasoconstriction, which can lead to stroke, progressive cerebral edema, or even death.
Reversible cerebral vasoconstrictions severe complications appear to be more common in postpartum mothers.
The condition is eventually diagnosed in 45% of outpatients with sudden headache, and 46% of outpatients with thunderclap headache.
Children are rarely affected.
It is more common in females, with a female-to-male ratio of 2.4:
Calcium channel blockers may help reduce the intensity and frequency of the headaches.
