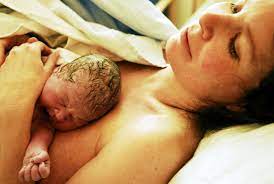
The postpartum period begins after childbirth and is typically considered to end within six weeks.
There are three distinct but continuous phases of the postnatal period;
The acute phase, lasting for six to twelve hours after birth;
The subacute phase, lasting six weeks;
The delayed phase, lasting up to six months.
Some delayed changes to the genitourinary system takes much longer to resolve and may result in conditions such as urinary incontinence.
The postnatal period is the most critical and most neglected phase in the lives of mothers and babies; most maternal and newborn deaths occur during this period.
A woman giving birth in a hospital may leave as soon as she is medically stable, which can be as early as a few hours postpartum.
The average hospital stay for a vaginal birth is one to two days.
The average caesarean section postnatal stay is three to four days.
During this time, the mother is monitored for bleeding, bowel and bladder function, and baby care.
The infant’s health is also monitored.
Early postnatal hospital discharge is typically defined as discharge of the mother and newborn from the hospital within 48 hours of birth.
In the subacute postpartum period, 87% to 94% of women report at least one health problem.
Long-term health problems, persisting after the delayed postpartum period are reported by 31% of women.
Acute phase
Postpartum uterine massage helps the uterus to contract after the placenta has been expelled in the acute phase.
The first 6 to 12 hours after childbirth the mother is typically monitored by nurses or midwives as complications can arise.
The greatest health risk in the acute phase is postpartum bleeding.
Following delivery, where the placenta was attached to the uterine wall bleeds, and the uterus must contract to prevent blood loss.
After uterine contraction takes place the fundus of the uterus can be palpated as a firm mass at the level of the navel.
Uterine massage is commonly used to help the uterus contract.
Following delivery if the mother had an episiotomy or tearing at the opening of the vagina, it is stitched.
The routine episiotomy, with a normal delivery without complications or instrumentation, does not offer benefits in terms of reducing perineal or vaginal trauma.
Selective use of episiotomy does result in less perineal trauma.[
Within about 10 seconds the infant takes its first breath and the caregiver places the baby on the mother’s chest.
The infant’s condition is evaluated using the Apgar scale.
The Apgar score is determined by evaluating the newborn baby on five criteria: Appearance, Pulse, Grimace, Activity, Respiration (APGAR).
It is suggested that early skin-to-skin contact by placing the naked baby on the mother’s chest is of benefit to both mother and infant. (Skin to skin contact).
The World Health Organization (WHO) also encourages skin-to-skin contact for the first 24 hours after birth to help regulate the baby’s temperature.
The subacute postpartum starts after the acute postpartum period concludes and can last for two to six weeks.
In the first few days following childbirth, the risk of a deep vein thrombosis (DVT) is relatively high as hypercoagulability increases during pregnancy and is maximal in the postpartum period.
This is particularly for women with C-section with reduced mobility.
Anti-coagulants or physical methods such as compression may be used in the hospital, particularly if the woman has risk factors, such as obesity, prolonged immobility, recent C-section, or first-degree relative with a history of thrombotic episode.
For women with a history of thrombotic event in pregnancy or prior to pregnancy, anticoagulation is generally recommended.
The increased vascularity and edema of the vagina gradually resolves in about three weeks.
The cervix gradually narrows and lengths over a few weeks.
Postpartum infections can lead to sepsis and death.
Postpartum urinary incontinence is experienced by about 33% of all women.
Women who deliver vaginally are about twice as likely to have urinary incontinence as women who give birth via a cesarean.
Urinary incontinence in the postpartum period increases the risk of long term incontinence.
In the subacute postpartum period, 87% to 94% of women report at least one health problem.
Kegel exercises are recommended in the postpartum period to strengthen the pelvic floor muscles and control urinary incontinence.
Adult diapers may be worn in the subacute postpartum period for lochia, as well as urinary and fecal incontinence.
Discharge from the uterus, called lochia, will gradually decrease and turn from bright red, to brownish, to yellow and cease at around five or six weeks.
Women are advised in this period to wear adult diapers or nappies, disposable maternity briefs, maternity pads or towels, or sanitary napkins.
The use of tampons or menstrual cups are contraindicated as they may introduce bacteria and increase the risk of infection.
An increase in lochia between 7–14 days postpartum may indicate delayed postpartum hemorrhage.
In the subacute postpartum period hemorrhoids and constipation in are common, and stool softeners are routinely given.
Some women feel uterine contractions, called afterpains, during the first few days after delivery: similar to menstrual cramps and are more common during breastfeeding, due to the release of oxytocin.
The cramping is the compressing of the blood vessels in the uterus to prevent bleeding.
At two to four days postpartum, a woman’s breastmilk will generally come in.
Maternal sleep is often disturbed as night waking is normal in the newborn, and newborns need to be fed every two to three hours, including during the night.
During the subacute postpartum period, psychological disorders may emerge: postpartum depression, posttraumatic stress disorder, and in rare cases, postpartum psychosis.
Postpartum mental illness can affect both mothers and fathers.
Approximately 70–80% of postpartum women will experience the “baby blues” for a few days, and 10 and 20 percent may experience clinical depression.
Clinical depression is seen with a a higher risk among those women with a history of postpartum depression, clinical depression, anxiety, or other mood disorders.
The prevalence of PTSD following normal childbirth (excluding major complications) is estimated to be between 2.8% and 5.6% at six weeks postpartum.
It is recommend that all women have contact with their obstetric provider within the first three weeks postpartum to address acute issues, with subsequent care as needed.
A more comprehensive postpartum visit should be done
At 4 to 12 weeks postpartum a comprehensive postpartum visit should be done to address the mother’s mood and emotional well-being, physical recovery after birth, infant feeding, pregnancy spacing and contraception, chronic disease management, and preventive health care and health maintenance.
Women with hypertensive disorders should have a blood pressure check within three to ten days postpartum.
More than one half of postpartum strokes occur within ten days of discharge after delivery.
Women with chronic medical conditions: hypertensive disorders, diabetes, kidney disease, thyroid disease and psychiatric conditions should continue to follow with their obstetric or primary care provider for ongoing disease management.
Women with pregnancies complicated by hypertension, gestational diabetes, or preterm birth should undergo counseling and evaluation for cardiometabolic disease, as lifetime risk of cardiovascular disease is higher in these women.
The WHO recommends postpartum evaluation of the mother and infant at three days, one to two weeks, and six weeks postpartum.
The delayed postpartum period starts after the subacute postpartum period and lasts up to six months.
During the delayed postpartum period the muscles and connective tissue return to a pre-pregnancy state.
Recovery from childbirth complications: urinary and fecal incontinence, painful intercourse, and pelvic prolapse, are typically very slow and in some cases may not resolve.
Symptoms of PTSD drop from 2.8% and 5.6% at six weeks postpartum to 1.5% at six months postpartum.
During this delayed postpartum period, infant sleep during the night gradually increases and maternal sleep generally improves.
Approximately three months after giving birth estrogen levels drop and large amounts of hair loss is common, particularly in the temple area, known as postpartum alopecia.
Typically, the hair grows back normally and treatment is not indicated.
Factors attributing the likelihood of post natal problems include: the size of the infant; the method of delivery, such as c-section, or of forceps; perineum trauma from either an episiotomy or natural tearing; and the physical condition of the birth mother.
Postnatal complications include: uterine prolapse, cystocele, rectocele, fecal incontinence, and urinary incontinence.
Long-term health problems that persist after the delayed postpartum period are reported by 31% of women.
In the post partum period cardiovascular health behavior counseling should include a Mediterranean diet, resumption of physical activity, return to pre-pregnancy weight, smoking cessation, screening for diabetes, blood pressure screening, and lipid analysis.
The American College of Obstetricians and Gynecologists (ACOG) recommends women take at least six weeks off work following childbirth.
The United States is the only country in the Organization for Economic Co-operation and Development (OECD) that does not to provide paid maternity, paternity, and parental leave.
