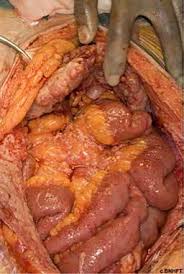
Mesothelioma is a rare cancer originating in mesothelial surfaces of the peritoneum, pleura, and other sites that is estimated to occur in approximately 3,500 people in the United States every year.
Mesotheliomas are now defined as malignant.
Peritoneal mesothelioma is much less common than pleural mesothelioma and accounts for approximately 15% of cases.
While most mesothelioma occurs in the pleura (approximately 85%), it can also occur very rarely in other sites, such as the pericardium and tunica vaginalis testis.
It is estimated that PM occurs in approximately 300 to 400 people in the US every year, but the true incidence may be higher as it may be misdiagnosed with other cancers involving the peritoneum.
The incidence of mesotheliomas are decreasing in the United States because asbestos use has decreased since the 1970s.
Mean age is 69 years at diagnosis.
One year overall survival approximately 46% and in five year overall survival about 20%.
The diagnosis of PeM may be delayed because it mimics other diseases and conditions and because the disease is so rare.
To diagnose PeM: CT imaging of the chest/abdomen/pelvis and laparoscopy to obtain a biopsy of the abdominal mass/nodule.
Laparoscopy is also performed to assess whether complete CRS is possible.
Fine-needle aspiration of the nodule/mass is not recommended for diagnosis, because fine-needle aspiration cannot differentiate between the different histologic subtypes of PeM, including epithelioid, sarcomatoid, and biphasic.
Most patients have diffuse mesothelioma.
Localized pleural mesothelioma may occur, but it is very rare.
Treatment options depend on histology.
Using paracentesis fluid cytology is also not recommended for diagnosis, as invasion cannot be detected using cytology.
Measurement of soluble mesothelin-related peptide and CA-125 levels may correlate with disease status.
Cure is rare.
Survival is improved by complete cytoreductive surgery with intraperitoneal chemotherapy.
Histologic subtypes include epithelioid, the most common, sarcomatoid, and biphasic or mixed.
Patients with epithelioid histology have better outcomes than those with either biphasic or sarcomatoid histologies.
Epithelioid subtype is associated with a longer median overall survival (39 months) compared with patients who have a biphasic subtype (14 months).
The median survival is improved if patients are able to undergo cytoreductive surgery (55 months for epithelial histology vs 13 months for biphasic).
For a diagnosis of mesothelioma, the lesion needs to be diffuse, mesothelial, and malignant, with no single IHC marker to diagnosis.
While pleural mesothelioma is more common in males, there are equal numbers of males and females with pleural mesothelioma.
Patients with peritoneal mesothelioma are generally younger than patients with pleural mesothelioma.
Pleural mesothelioma is typically caused by asbestos exposure, but peritoneal mesothelioma is less frequently associated with asbestos.
The incidence of pleural and peritoneal mesothelioma is decreasing because of decreased asbestos use.
PeM is found in equal numbers of males and females, while pleural mesothelioma is more common in males.
PeM may occur in younger patients, whereas pleural mesothelioma typically occurs in older patients.
Many patients with PeM have idiopathic disease.
Pleural mesothelioma is typically caused by asbestos exposure.
PeM is less frequently associated with asbestos exposure than pleural mesothelioma.
Patients present in an indolent fashion with abdominal pain, distention, ascites, and weight loss with a median time of 4 to 6 months between symptom onset and diagnosis.
Radical resection with cytoreductive surgery, and hyperthermia, intraperitoneal chemotherapy are the primary curative measures for malignant peritoneal mesothelioma,and the strongest predictor of long-term survival is complete removal of all visible disease.
Cytology has limited sensitivity for diagnosis, ranging from 30 to 75% and is not recommended for diagnosis.
Adequate biopsy is recommended for histologic diagnosis and immunohistochemistry.
Such biopsies can be attained at the time of diagnostic laparoscopic exam or by image guided biopsy in the setting of a mass.
Sarcomatoid subtype accounts for 20% of cases, and has more aggressive disease process, with local invasion, and spread beyond the peritoneal cavity.
Sarcomatoid subtype has a universal poor prognosis with prompt recurrences and immediate survival of less than six months, and is a contraindication to curative intense surgery.
Evaluation includes CT of the chest, abdomen and pelvis at the time of diagnosis and findings can help rule out bicavity involvement, which is a relative comfort indication for upfront surgery.
The presence of metastatic lymphadenopathy has a poor prognosis and is present in 7 to 13% of patients.
Imaging studies often underestimate the peritoneal cancer index, the extent of disease for prognosis and operability.
The studies are important, however, to avoid unresectable disease and non-therapeutic laparotomy.
Genetic factors play a role in some patients with families carrying the germline mutation in the BRCA, 1 associated protein– one gene, and a few patients with somatic mutation, such as anaplastic lymphoma kinase (ALK) rearrangements.
Patient presents with abdominal signs and symptoms: ascites(77%) pain (69%), distention, and abdominal mass (30%).
Patients frequently have weight loss, fatigue, anorexia, asthenia, and nausea, along with early satiety and intestinal obstruction.
Diagnosis may be delayed because of non-specific symptoms.
Many patients have advanced disease at diagnosis with extensive intraabdominal spread, and commonly the disease metastasizes beyond the abdominal cavity.
Diagnosis evaluation include CT examination of the chest, abdomen and pelvis, and laparoscopic exam to obtain a biopsy of the mass or nodules.
Fine needle, aspiration, and paracentesis are not adequate for diagnosis.
Measurement of soluble, mesothelin related peptide and CA125 levels are considered.
Tissue biopsy is essential for accurate diagnosis as other studies are not specific.
Localized, peritoneal mesothelioma is extremely rare.
Epithelioid subtype peritoneal mesothelioma has a median survival of 39 months compared with biphasic subtype of 14 months.
The median survival is of patients is improved if they can undergo cytoreductive surgery.
For diagnosis, the lesion needs to be diffuse, mesothelial, and malignant.
There is no single immunohistochemistry marker for diagnosis.
Different IHC markers need to be used to distinguish PeMs from other carcinomas, such as gynecologic malignancies or renal cell carcinomas.
Positive markers include calretinin, podoplanin and PAX8 are recommended.
BAP1, a tumor suppressive gene loss is a useful molecular marker for diagnosing mesothelioma.
Aberrant BAP1 protein expression defined as absence of nuclear BAP1 IHC staining, occurs in about 50% to 70% of patients with epithelioid mesothelioma but in fewer than 20% of those with sarcomatoid mesothelioma.
BAP1 IHC is useful for distinguishing mesotheliomas from benign mesothelial tumors.
It is important to note that IHC markers for diagnosing PeM differ slightly from those for diagnosing pleural mesothelioma.
For example, TTF-1 and D2-40 are not useful for diagnosing PeM, although they are useful for diagnosing pleural mesothelioma.
MANAGMENT:
Treatment options for diffuse, peritoneal mesothelioma include surgery and/or systemic therapy.
Radiation is reserved for selective patients for palliation.
Cytoreductive surgery and intraperitoneal chemotherapy are standard approaches for patients eligible for surgery.
Patients with medically operable diffuse PeM and good performance status are candidates for multimodality therapy, including those with epithelioid histology and unicavitary disease.
Surgery is typically contraindicated with bicavity disease and those with biphasic or sarcomatoid histology.
Complete cytoreduction is recommended for patients with epithelioid histology and unicavity peritoneal mesothelioma who are medically operable.
Complete macroscopic resection, while removing all visible or palpable tumors frequently involves a total peritonealectomy.
Cytoreductive surgery should be aborted if it is not possible to have a complete or near complete cytoreduction.
In patients with complete cytoreduction and hyperthermia inta5 peritoneal chemotherapy, the overall median survival was 53 months with three and five years survival rates of 60 and 47% respectively.
Intraperitoneal agents include cisplatin, doxyrubicin, or mitomycin C.
Systemic therapy regimens are considered for patients with mesothelioma who are not eligible for surgery and include agents like platinum and pemetrexed.
Best supportive care is recommended for patients with a performance status PS of 3–4.
Radiation therapy is not recommended as a primary therapy for PeM but can be used selectively for palliation.
No phase randomized trials to determine the best treatment for patients with PeM exist because it is so rare.
Because PeM and pleural mesothelioma are similar, systemic therapy recommendations for PeM are based on extrapolating data from clinical trials in pleural mesothelioma.
Data show good outcomes for eligible patients with PeM who have cytoreductive surgery and intraperitoneal chemotherapy.
Laparoscopy surgical evaluation is done to assess whether patients are candidates for surgery.
After a diagnosis of diffuse PeM, PET/CT is done to determine whether patients have unicavitary or bicavitary disease.
Surgery is typically contraindicated in patients with bicavitary disease and those with biphasic or sarcomatoid histology.
Complete cytoreduction is recommended for patients with epithelioid histology and unicavitary PeM.
The surgical goal for PeM is cytoreduction to achieve macroscopic complete resection by removing all visible or palpable tumors, which frequently involves a total parietal peritonectomy.
If macroscopic complete resection or near complete cytoreduction is not possible, surgery should be aborted.
Palliative surgery and/or HIPEC can be considered.
There is no accepted staging system for PeM.
A multi-institutional study assessed CRS and HIPEC in 401 patients with PeM; 46% had complete or near complete cytoreduction and 92% received HIPEC: The median overall survival was 53 months, 3-year and 5-year survival rates were 60% and 47%, respectively.
Grade 3–4 complications occurred in 31%.
A meta-analysis assessed CRS and intraperitoneal chemotherapy in 1,047 patients with PeM.
Complete cytoreduction was done in 67% of patients (46%–93%). Survival estimates were 84% at 1 year, 59% at 3 years, and 42% at 5 years.
In a single-institution study, 108 patients with PeM had CRS and HIPEC with cisplatin and either doxorubicin or mitomycin-C.
The median overall survival was 63.2 months.
Nineteen patients survived more than 7 years and appeared to be cured.
Major morbidity was 38.9%; 2 patients died perioperatively.
In another single-institution study, 84 patients with PeM had CRS and HIPEC with cisplatin plus doxorubicin; 66 patients had complete or near complete cytoreduction.
Almost all patients had epithelioid histology.
The median overall survival was 38.4 months, 5-year survival was 42%.
The NCCN recommends CRS and HIPEC for eligible patients with PeM based on trials for PeM and pleural mesothelioma.
Complete cytoreduction and HIPEC are recommended for patients with unicavitary PeM and epithelioid histology who are medically operable ia complete cytoreduction is achievable.
Perioperative systemic therapy should be considered if patients have high-risk features (such as Ki-67 >9%, nodal metastases, high tumor burden, biphasic disease, or bicavitary disease.
After perioperative therapy, patients may be eligible for CRS and HIPEC. Systemic therapy alone is recommended for patients with PS of 0–2 who are medically inoperable or refuse surgery.
Intraperitoneal preferred chemotherapy regimens: 1) cisplatin plus doxorubicin; (2) cisplatin; (3) carboplatin; or (4) cisplatin plus mitomycin.
Pemetrexed regimens: Median survival was not reached for patients receiving first-line therapy with either pemetrexed alone or pemetrexed plus cisplatin; response rate was 25%.
Median survival was 13.1 months for patients with PeM receiving second-line therapy with either pemetrexed alone or pemetrexed plus cisplatin; response rates were 23.3%.
Immune checkpoint inhibitors in patients with PeM have an overall response rate of 19%, And a median duration of overall survival was 19 months.
Patients responded to ICIs regardless of whether they had responded to previous platinum-based chemotherapy, and a median duration of overall survival was 19 months, with a 1-year overall survival rate was 68%.
Systemic therapy alone is recommended for patients with a PS of 0–2 and diffuse PeM, including those who are medically inoperable, for whom a complete CRS cannot be achieved, or who refuse surgery, with bicavitary disease regardless of histology and stage, with sarcomatoid or biphasic histology regardless of stage; or with recurrence after previous CRS and HIPEC.
Surgery may be considered in select patients with bicavitary disease or low-volume biphasic disease.
About 50% of patients with PeM have positive PD-L1 expression levels.
The preference stratified the first-line systemic therapy regimens for eligible patients with PeM and epithelioid histology who are not eligible for surgery are the following regimens are preferred options: (1) pemetrexed plus cisplatin plus bevacizumab; (2) pemetrexed plus cisplatin; or (3) nivolumab plus ipilimumab.
Carboplatin is recommended if patients are not candidates for cisplatin, regardless of histology.
The preference first-line systemic therapy regimens for eligible patients with PeM and biphasic or sarcomatoid histology who are not eligible for surgery and voted that nivolumab plus ipilimumab is the preferred option: other recommended regimens: (1) pemetrexed plus cisplatin plus bevacizumab; or (2) pemetrexed plus cisplatin.
