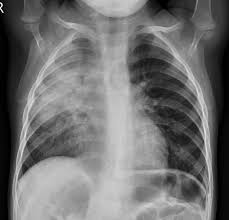
 Pneumonia is an invasion of the lower respiratory tract, below the larynx by pathogens either by inhalation, aspiration, respiratory epithelium invasion, or hematogenous spread.
Pneumonia is an invasion of the lower respiratory tract, below the larynx by pathogens either by inhalation, aspiration, respiratory epithelium invasion, or hematogenous spread.
Pneumonia is a leading cause of morbidity and mortality in children younger than the age of 5 years, worldwide.
Pneumonia accounts for 14% of all deaths of children under 5 years old.
Most of the deaths occurring in infants younger than one year of age.
The majority of deaths attributed to pneumonia in children are mostly in the developing world.
Approximately 83% of the 808,000 annual debts from pneumonia among children occur in sub Saharan Africa, south, Asia, and Latin America.
The etiology of pneumonia in the pediatric population can be classified by age-specific or pathogen-specific organisms.
Neonates are at risk for bacterial pathogens present in the birth canal, and this includes organisms such as group B streptococci, Klebsiella, Escherichia coli, and Listeria monocytogenes.
Streptococcus pneumoniae, Streptococcus pyogenes, and Staphylococcus aureus can be identified in late-onset neonatal pneumonia.
Viruses are the main cause of pneumonia in older infants and toddlers between 30 days and 2 years old.
In children 2 to 5 years old, respiratory viruses are also the most common causes of pneumonia.
In children 2 to 5 years old there is a rise of cases related to S. pneumoniae and H. influenzae type B is observed in this age group.
Mycoplasma pneumonia frequently occurs in children in the range from 5 to 13 years old,and S. pneumoniae is the most commonly identified organism.
Adolescents usually have the same infectious risks as adults.
Tuberculosis (TB) is considered in immigrants from high prevalence areas, and children with known exposures.
Children with chronic diseases are at risk for specific pathogens: cystic fibrosis with pneumonia secondary to S. aureus and Pseudomonas aeruginosa, while patients with sickle cell disease are at risk of infection from encapsulated organisms.
Children who are immunocompromised are evaluated for Pneumocystis jirovecii, cytomegalovirus, and fungal species, as the cause of pneumonia if no other organism is identified.
Unvaccinated children are at risk for vaccine-preventable pathogens related pneumonias.
Exposure to find particulate matter with aerodynamic diameter of 2.5 micro millimeters or less from incomplete combustion of solid fuel is a risk factor for pneumonia.
Almost 30% of the global pediatric deaths from pneumonia are attributed to household air pollution.
Approximately 2.4 billion people in predominantly and low and middle income countries use biomass daily for cooking or for heating their households: However, studies have shown the incident, severe of severe pneumonia among infants did not significantly significantly differ between those whose mothers were assigned to cook with liquefied petroleum gas and fuel, and those mothers were assigned to continue cooking with biomass stove (HAPIN investigators).
There are an estimated 120 million cases of pneumonia annually worldwide, resulting in as many as 1.3 million deaths.
Younger children under the age of 2 in the developing world, account for nearly 80% of pediatric deaths secondary to pneumonia.
The prognosis of pneumonia is better in the developed world.
The introduction of the pneumococcal vaccine has significantly lowered the risk of pneumonia in the United States.
Barriers to pneumonia infection include: anatomical structures of nasal hairs, turbinates, epiglottis, cilia, and humoral and cellular immunities.
Breaching these barriers results in infection, either by fomite/droplet spread (mostly viruses) or nasopharyngeal colonization (mostly bacterial), results in inflammation and injury or death of surrounding epithelium and alveoli.
Such breaching is accompanied by a migration of inflammatory cells to the site of infection, causing an exudative process, which in turn impairs oxygenation.
In the majority of cases, the microbe is not identified, and the most common cause is of viral etiology.
There are four stages of lobar pneumonia. The first stage occurs within 24 hours and is characterized by alveolar edema and vascular congestion. Both bacteria and neutrophils are present.
Red hepatization is the second stage, and it has the consistency of the liver. The stage is characterized by neutrophils, red blood cells, and desquamated epithelial cells. Fibrin deposits in the alveoli are common.
The third stage of gray hepatization stage occurs 2-3 days later, and the lung appears dark brown. There is an accumulation of hemosiderin and hemolysis of red cells.
The fourth stage is the resolution stage, where the cellula infiltrates is resorbed, and the pulmonary architecture is restored. If the healing is not ideal, then it may lead to parapneumonic effusions and pleural adhesions.
In bronchopneumonia, there is often patch consolidation of one or more lobes. The neutrophilic infiltrate is chiefly around the center of the bronchi.
In many cases, complaints associated with pneumonia are nonspecific, including cough, fever, tachypnea, and difficulty breathing.
Young children may present with abdominal pain.
History obtained includes the duration of symptoms, exposures, travel, sick contacts, baseline health of the child, chronic diseases, recurrent symptoms, choking, immunization history, maternal health, or birth complications in neonates.
Examination includes observation for signs of respiratory distress, including tachypnea, nasal flaring, lower chest in-drawing, or hypoxia on room air.
Infants with pneumonia may present with inability to feed, with grunting or apnea.
Lung auscultation for rales or rhonchi in all lung fields aids in diagnosis.
No isolated physical exam finding can accurately diagnose pneumonia.
The combination of symptoms, including fever, tachypnea, focal crackles, and decreased breath sounds together, raises the sensitivity for finding pneumonia on x-ray.
Pneumonia is a clinical diagnosis, with consideration the history of present illness, physical exam findings, adjunct testing, and imaging modalities.
Laboratory evaluation in children suspected of having pneumonia should ideally start with non-invasive, rapid bedside testing including nasopharyngeal swab assays for influenza, respiratory syncytial virus, and human metapneumovirus when available and appropriate.
It is necessary to minimize unnecessary imaging and antibiotic treatment in children with influenza or bronchiolitis.
Children who present with severe disease and appear toxic should have complete blood count (CBC), electrolytes, renal/hepatic function testing, and blood cultures performed, but are generally not required in children who present with mild disease.
Viral and bacterial pneumonia cannot be distinguished by inflammatory markers in the pediatric population.
However,these tests may be obtained to trend disease progression and serve as prognostic indicators.
In areas endemic to TB, or have exposure history, and present with signs and symptoms suspicious for pneumonia should have sputum samples or gastric aspirates collected for culture.
Sputum gram stain and culture are not productive as the samples are often contaminated by oral flora.
Blood cultures can be done but are often negative.
Today, serology is being used to determine the presence of mycoplasma, legionella, and chlamydia species.
PCR is available but still, the results take 24-48 hours.
No clear guidelines exist for the routine use of chest x-ray in the pediatric population.
The chest x-ray can be helpful in diagnosis and confirmation of pneumonia,, but it carries with it risks, including radiation exposure, healthcare-associated costs, and false-negative results, increasing the use of unwarranted antibiotics.
CXR imaging should be restricted to children who appear toxic, those with the recurrent or prolonged course of illness despite treatment, infants ages 0 to 3 months with a fever, suspected foreign body aspiration, or congenital lung malformation.
Imaging can also be considered in children younger than 5 years old, who present with fever, leukocytosis, and no identifiable source of infection.
Imaging may also be useful in those with acute worsening of upper respiratory infections or to rule out underlying mass.
Treatment is targeted to a specific pathogen that is suspected based on history and physical exam.
Supportive care includes supplemental oxygen for hypoxia, antipyretics for fever, and fluids for dehydration, especially for non-infectious pneumonitis and viral pneumonia for which antibiotics are not indicated.
Cough suppressants are not recommended in pediatric pneumonia.
When a bacterial pneumonia is suspected, empirical treatment with antibiotics is appropriate based on history and bacterial pathogens that are common to specific age groups.
Neonates should receive ampicillin plus an aminoglycoside or third-generation cephalosporin.
Ceftriaxone is not used on neonates as it can displace bound bilirubin and lead to kernicterus.
Atypical pneumonia is common in infants 1 to 3 months old, and this group should have additional antibiotic coverage with erythromycin or clarithromycin.
For infants and children over 3 months old, S. pneumoniae is the most common bacterial pneumonia for which the drug of choice is high-dose oral amoxicillin or another beta-lactam antibiotic.
In children older than 5 years old with bacterial pneumonia, atypical agents have a more important role, and macrolide antibiotics are usually first-line therapy.
Special attention should be given to children with chronic illnesses, as these might alter choices for antibiotics: sickle cell anemia, cystic fibrosis.
Treatment of fulminant viral pneumonia depends on the virus identified.
For Varicella, use acyclovir and for the respiratory syncytial virus (RSV), use ribavirin for high-risk patients.
Patients with HIV should be treated with sulfamethoxazole/trimethoprim and prednisone, and for Cytomegalovirus, ganciclovir and gamma globulin are the preferred agents.
If methicillin-resistant Staphylococcus aureus (MRSA) is suspected, clindamycin or vancomycin may be given.
Neonates and infants younger than 90 days old should be hospitalized for treatment, in addition to children who are immunocompromised or have other underlying chronic diseases like sickle cell anemia or cystic fibrosis.
Admission is often required for patients with respiratory distress/ low oxygenation.
The presence of a parapneumonic effusion usually requires hospital admission.
For most children, the prognosis of pediatric is good.
Viral pneumonia tends to resolve without treatment, and long-term sequelae are rare.
Staphylococcal and varicella pneumonia have guarded outcomes in children.
Each year, roughly 3 million children die from pneumonia and the majority of these children also have other comorbidities like congenital heart disease, immunosuppression, or chronic lung disease of prematurity.
Pediatric pneumonia is often undertreated or missed, leading to high morbidity and mortality.
Pediatric pneumonia complications:
Empyema
Pleural effusion
Lung abscess
Necrotizing pneumonia
Sepsis
Pneumonia can be caused by viruses, bacteria or fungi.
Pneumonia can often be prevented by immunization, adequate nutrition, and by addressing environmental factors.
Pneumonia caused by bacteria can be treated with antibiotics, but only one third of children with pneumonia receive the antibiotics they need.
Pneumonia is caused by several infectious agents, including viruses, bacteria and fungi.
The most common are the following.
Streptococcus pneumoniae is the most common cause of bacterial pneumonia in children.
Haemophilus influenzae type b is the second most common cause of bacterial pneumonia.
Respiratory syncytial virus is the most common viral cause of pneumonia.
In infants infected with HIV, Pneumocystis jiroveci is one of the most common causes of pneumonia, responsible for at least one quarter of all pneumonia deaths in HIV-infected infants.
The presenting features of viral and bacterial pneumonia are similar.
The symptoms of viral pneumonia may be more varied than the symptoms of bacterial pneumonia.
Wheezing is more common in viral infections.
Very severely ill infants may be unable to feed or drink and may also experience unconsciousness, hypothermia and convulsions.
Children whose immune systems are compromised are at higher risk of developing pneumonia.
A child’s immune system may be weakened by malnutrition or undernourishment, especially in infants who are not exclusively breastfed.
Pre-existing illnesses, such as symptomatic HIV infections and measles, also increase a child’s risk of contracting pneumonia.
Environmental factors also increase a child’s susceptibility to pneumonia:
indoor air pollution caused by cooking and heating with biomass fuels
living in crowded homes
parental smoking.
Pneumonia should be treated with antibiotics.
The antibiotic of choice for first line treatment is amoxicillin dispersible tablets.
Hospitalization is recommended only for severe cases of pneumonia.
Preventing pneumonia in children is an essential component of a strategy to reduce child mortality. Immunization against Haemophilus influenzae, pneumococcus, measles and whooping cough (pertussis) is the most effective way to prevent pneumonia.
Adequate nutrition is key to improving children’s natural defences, starting with exclusive breastfeeding for the first 6 months of life.
Providing affordable clean indoor stoves, and encouraging good hygiene in crowded homes also reduces the number of children who fall ill with pneumonia.
In children infected with HIV, the antibiotic cotrimoxazole is given daily to decrease the risk of contracting pneumonia.
