 A disease of articular cartilage, with cartilage degeneration and erosion being the main identifying features.
A disease of articular cartilage, with cartilage degeneration and erosion being the main identifying features.
The most common and persistent cause of mobility dependence and disability.
On average, patients with OA live more than 26 years.
Subchondral bone resorption and turnover contribute to the pathogenesis of osteoarthritis.
There is an increased prevalence of osteoarthritis, do in part to the aging population and the growing obesity epidemic.
A disabling disease that affects multiple joint components, including articular cartilage, subchondral bone, and the synovial joint lining.
Presents with joint pain and stiffness.
Begins with degradation of the articular cartilage in a focal and nonuniform manner.
Accompanied by subchondral thickening, bone outgrowths at the joint margin and juxta-articular bone cysts.
Growths at joint margins referred to as osteophytes.
Initiating events probably due to abnormal signals altering chondrocyte phenotype synthesizing proteins that degrade cartilage matrix and cause joint degeneration.
Most common joint disorder in the U.S.
It is the most common form of arthritis, affecting 250, million people worldwide.
Approximately 46 million people in the US have symptomatic osteoarthritis.
Approximately 10-12% of the adult population in the US have symptomatic osteoarthritis.
Affects an estimated 250 million people worldwide.
Almost 1 in 2 people will develop symptomatic OA of the knee by age 85.
In 2010 OA accounted for 2.2% of global years lived with disability.
1in 4 will develop painful hip arthritis in their lifetime.
The fastest increasing major health condition accounting for 17 million years lived with disability in 2010 reflecting a 64% increase from 1990-2010.
64% of people are of working age, 15-64 years, and 11% of the workforce is made up of people who have osteoarthritis.
Most costs associated with OA are indirect and associated with loss of work, productivity, sick leave, premature retirement, and quality-of-life.
A significant component of healthcare costs for managing osteoarthritis is related to hip and knee replacements, with osteoarthritis accounting for about 95% of surgical volume for these procedures.
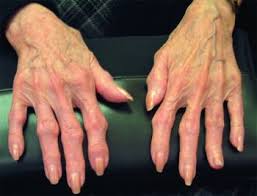
The distal interphalangeal and first carpometacarpal joints of the hand are commonly affected.
Typically affects the smaller joints of the fingers, weight beating joints of the legs and movable portions of the spine, although any diarthrodial joint can be affected.
Clinical symptoms often do not correlate with objective findings.
Rare before age 40, yet by age 75 eighty five percent of the population have radiographic or clinical evidence of disease.
Third National Health and Nutrition Examination survey estimates that 37.4% of adults in the U.S. who are 60 years of age or older have radiographic evidence of this process.
Leading cause of arthritis.
Up to 6% of adult population.
80% of patients have movement limitation, and 25% have difficulty performing major activities of daily living.
Osteoarthritis-estimated $60 billion per year economic burden.
Acetaminophen is the initial drug of choice.
NSAIDs are the main theme of four pharmacologic therapy as a result of their efficacy, onset of action, and low cost.
Leading indication for knee and hip replacements.
Present in most people older than 65 years.
All patients with OA of the knee should be taught quadriceps-strengthening exercises.
Weight reduction program should be recommended for all overweight patients.
Pain can originate in the synovium, the joint capsule, intra-articular ligaments, from edematous bone marrow as well as in the muscles and soft tissues but not in the cartilage since the latter has no nerves.
The two major treatment goals are: alleviating pain and preventing structural damage progression.
Physical activity benefits patients with OA by preventing additional loss of motion, stiffness and progressive weakness.
Randomized control studies show appropriate exercise is important in the management of knee OA.
Exercise aids in weight loss in OA.
Exercise prevents weight gain, atrophy of muscle, and loss of joint mobility.
Exercise programs result in reduction of pain in arthritis.
Physical therapy with strengthening, acquatic and resistance training recommended for hip and knee OA.
Aerobic walking and strengthening of quadriceps for knee OA improves pain and disability.
Presently, there are no approved disease modifying therapies that prevent structural progression of arthritis of the knee.
