The mediastinum cavity separates the lungs from the rest of the chest.
It contains the heart, esophagus, trachea, thymus, and aorta.
Greater than 60% of masses are thymomas, neurogenic tumors, benign cysts and lymph nodes.
All patients with the mediastinal mass should be evaluated to determine the type of mass and extent of disease before treatment.
It is essential to differentiate between thymine malignancies and other lesions, such as lung metastasis, lymphoma, goiter, germ cell tumors, before treatment as management differs.
More than half of the primary cancers in the anterior mediastinum or thymomas.
The most common mediastinal masses are neurogenic tumors (20% of mediastinal tumors), usually found in the posterior mediastinum, followed by thymoma (15–20%) located in the anterior mediastinum.
Lung cancer typically spreads to the lymph nodes in the mediastinum.
Most common lesions in children, greater than 80%, are neurogenic, germ cell tumors or foregut cysts.
Most common lesions in adults are lymphomas, lymph nodes thymomas, and thyroid masses.
Do not contain air bronchograms.
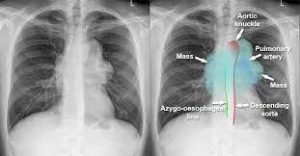
Mediastinal lines such as azygoesophageal recess, anterior junction lines and posterior junction lines are disrupted.
The mediastinum has three main parts: the anterior mediastinum (front), the middle mediastinum, and the posterior mediastinum (back).
Masses in the anterior portion of the mediastinum can include thymoma, lymphoma, pheochromocytoma, germ cell tumors including teratoma, thyroid tissue, parathyroid lesions, lung metastasis or nonneoplastic conditions, such as intrathoracic goiter, thymic, cysts, lymphangioma, and aortic aneurysms.
Masses in the anterior mediastinum area are more likely to be malignant than those in other compartments.
Masses in the posterior portion of the mediastinum tend to be neurogenic in origin, and in adults tend to be of neural sheath origin including neurilemomas and neurofibromas.
It is essential to differentiate between thymic malignancies and other conditions in the mediastinum: more than half of the primary cancers in the anterior mediastinum are thymomas.
THYMOMA:
Most common primary anterior mediastinal tumor (20%) in adults but rarely seen in children.
Tonofibrils seen under electron microscopy can differentiate thymoma from other tumors such as carcinoid, Hodgkin’s, and seminoma.
Patients are usually asymptomatic but can present with myasthenia gravis-related symptoms, substernal pain, dyspnea, or cough.
Invasive tumors can produce compression effects such as superior vena cava syndrome.
Thymomas are diagnosed with CT or MRI revealing a mass in anterior mediastinum.
Therapy in stage I tumors consists of surgical resection with good prognosis. Stage II–III requires maximal resection possible followed by radiation.
Stage IV disease requires addition of cisplatin-based chemotherapy in addition to those in stage II and III.
For those with invasive thymoma, treatment is based on induction chemotherapy, surgical resection, and post-surgical radiation.
5-year survival for invasive thymoma is between 12 and 54% regardless of any myasthenia gravis symptoms.
Lymphoma
Primary mediastinal large B-cell lymphoma, a rare type of lymphoma that arises in the mediastinum.
It is the second most common primary anterior mediastinal mass in adults.
Most are seen in the anterior compartment and rest are seen in middle compartment.
Hodgkin’s lymphoma usually present in 40–50’s with nodular sclerosing type, and non-Hodgkin’s appears in all age groups.
There is also primary mediastinal B-cell lymphoma with exceptionally good prognosis.
Symptoms of a mediastinal lymphoma of include fever, weight loss, night sweats, and compressive symptoms such as pain, dyspnea, wheezing, Superior vena cava syndrome, pleural effusions.
Diagnosis usually by CT showing lobulated mass.
Confirmation done by tissue biopsy of accompanying nodes if any, mediastinoscopy, mediastinotomy, or thoracotomy.
FNA biopsy is usually not adequate.
Treatment of mediastinal lymphoma is dependent upon the histologic type and involves chemoimmunotherapy and/or radiation.
