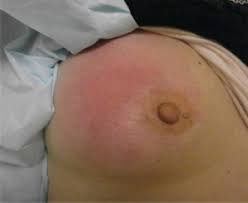
 Mastitis is inflammation of the usually associated with breastfeeding.
Mastitis is inflammation of the usually associated with breastfeeding.
The incidences vary between 2.6% and 33%, the prevalence globally is approximately 10% of breastfeeding women.
Symptoms typically include local pain , redness, often associated fever and general soreness.
Onset is typically fairly rapid.
Usually occurs within the first few months of delivery.
Most mothers who develop mastitis usually do so within the first few weeks after delivery.
Most breast infections occur within the first or second month after delivery or at the time of weaning.
Rarely affects women who are not breastfeeding.
Complications can include abscess formation.
Occurs in 10% of breastfeeding women.
Risk factors include poor latch, cracked nipples, use of a breast pump, and weaning.
The bacteria most commonly involved are Staphylococcus and Streptococci.
Gram-negative bacilli such as Escherichia coli. Salmonella spp., mycobacteria, and fungi such as Candida and Cryptococcus have been identified in rare instances.
Diagnosis is typically based on history, symptoms and clinical findings.
Ultrasound may be useful for detecting a potential abscess.
Prevention occurs with proper breastfeeding techniques.
When infection is present, antibiotics may be recommended.
Breastfeeding should typically be continued, as emptying the breast is important for healing.
Tentative evidence supports benefits from probiotics.
When it occurs in breastfeeding mothers, it is known as puerperal mastitis, lactation mastitis, or lactational mastitis.
When it occurs in non breastfeeding women it is known as non-puerperal or nonlactational mastitis.
Mastitis can, in rare cases, can occur in men.
The symptoms are similar for puerperal and nonpuerperal mastitis but predisposing factors and treatment can be very different.
Puerperal mastitis is the inflammation of the breast in connection with pregnancy, breastfeeding or weaning.
The tension and engorgement of the breast, it is thought to be caused by blocked milk ducts or milk excess.
Estimates range between 5–33%, but only about 0.4–0.5% of breastfeeding mothers develop an abscess.
Proper breastfeeding technique, frequent breastfeeding and avoidance of stress are the most important factors that can influenced the presence of mastitis.
Nonpuerperal mastitis
describes inflammatory lesions of the breast occurring unrelated to pregnancy and breastfeeding.
Periductal mastitis is a form of nonlactational mastitis, and is characterized by inflammation of the subareolar ducts.
Its cause is unknown, but smoking may be related.
This condition is mainly seen in young women but can also be seen in men.
Lactation mastitis usually affects only one breast.
Lactation mastitis symptoms can develop quickly;
There are three stages: the initial stage, the pus formation stage, to the restoration stage.
The signs and symptoms:
Breast tenderness or warmth to the touch
General malaise
Swelling of the breast
Pain or a burning sensation continuously or while breast-feeding
Skin redness
Fever of 101 F or greater
The affected breast can then start to appear lumpy and red.
Some experience flu-like symptoms such as:
Aches
Shivering and chills
Feeling anxious or stressed
Fatigue
A breast abscess is a collection of pus.
During lactation, breast abscess develops only rarely, most sources cite about 0.4–0.5% of breastfeeding women.
Breast abscess risk factors are age over 30, primiparous and late delivery.
Antibiotics are not shown effective in prevention of lactation abscess.
Mastitis typically develops when the milk is not properly removed from the breast.
Milk stasis can lead to the milk ducts in the breasts becoming blocked, as the breast milk is not being properly and regularly expressed.
Mastitis may occur when the baby is not appropriately attached to the breast while feeding, when the baby has infrequent feeds or has problems suckling the milk out of the breast.
The presence of cracks or sores on the nipples increases the likelihood of infection.
Tight clothing or ill-fitting bras may also cause problems as they compress the breasts.
There is a possibility that infants carrying infectious pathogens in their noses can infect their mothers.
Mastitis and breast abscesses can also be caused by direct trauma to the breast.
It can also develop due to contamination of a breast implant or any other foreign body:after nipple piercing.
Breastfeeding women are at risk for developing mastitis especially if they have sore or cracked nipples or have had mastitis before while breastfeeding another baby.
Chances of getting mastitis increased if women use only one position to breastfeed or wear a tight-fitting bra, which may restrict milk flow.
Difficulties in getting a nursing infant to latch on to the breast can also increase the risk for mastitis.
There is a higher susceptibility to the development of mastitis with diabetes, chronic illness, AIDS, or an impaired immune system.
Approximately 15% of cases of mastitis will require antibiotic treatment for infection which is usually caused by bacteria from the skin or the baby’s mouth entering the milk ducts through skin lesions of the nipple or through the opening of the nipple.
Most detected pathogens are very common species that are natural part of the breast fauna and simple detection of their presence is not sufficient to prove a causative role.
Indications are that treatment with antibiotics may have minimal impact.
There is insufficient evidence to confirm or refute the effectiveness of antibiotic therapy for treating lactational mastitis.
Diagnosis:
The diagnosis of mastitis and breast abscess can usually be made based on a physical examination.
Am ultrasound may be helpful in distinguishing between simple mastitis and abscess or in diagnosing an abscess deep in the breast.
In cases of infectious mastitis, cultures may be needed in order to determine what type of organism is causing the infection.
Cultures may be taken either from the breast milk or of the material aspirated from an abscess.
Mammograms or breast biopsies are performed on women who do not respond to treatment or on non-breastfeeding women.
Differential diagnosis
Breast cancer.
Mastitis episodes do not appear to influence lifetime risk of breast cancer.
Breast cancer may coincide with mastitis or develop shortly afterwards.
All suspicious symptoms that do not completely disappear within 5 weeks must be investigated.
Breast cancer incidence during pregnancy and lactation is the same as in control, with similar prognosis for age matched controls.
Some studies suggest noninflammatory breast cancer incidence is increased within a year following episodes of nonpuerperal mastitis.
Inflammatory breast cancer presents with similar symptoms as mastitis, both puerperal and nonpuerperal.
Treatment:
In lactation mastitis, frequent emptying of both breasts by breastfeeding is essential, and adequate fluid supply for the mother and baby are required.
For breastfeeding women with light mastitis, massage and application of heat prior to feeding may aid unblocking the ducts.
In more severe cases of mastitis heat or massage could make the symptoms worse and cold compresses are better suited to contain the inflammation.
Nonpuerperal mastitis is treated by medication and possibly aspiration or drainage.
Antibiotics are generally to be used in all nonpuerperal mastitis cases, with replacement of the antibiotics by an antifungal agent such as fluconazole in cases of deep fungal infections, and corticosteroids are to be used in case of granulomatous mastitis.
In lactational mastitis, antibiotics are not needed in the overwhelming majority of cases and should be used only for bacterial infections.
For people with nonsevere infections, dicloxacillin or cephalexin are recommended.
For people with severe infections, vancomycin is recommended.
The length of antibiotic treatment ranges anywhere from 5–14 days.
An abscess in the breast may be treated by ultrasound-guided fine-needle aspiration or by surgical incision and drainage; each of these approaches is performed under antibiotic coverage.
In case of puerperal breast abscess, breastfeeding from the affected breast should be continued where possible.
For small breast abscesses, ultrasound-guided fine needle aspiration such as to completely drain the abscess is widely recognized as a preferred initial management.
The exudate is then sent for microbiological analysis for identification of the pathogen and determination of its antibiotic sensitivity profile, which may in turn give an indication for changing the antibiotics.
Nonpuerperal breast abscesses have a higher rate of recurrence compared to puerperal breast abscesses.
There is a high statistical correlation of nonpuerperal breast abscess with diabetes mellitus.
