 Constitutes a very heterogeneous group of neoplasms with varying clinical presentations, prognoses and responses to treatment.
Constitutes a very heterogeneous group of neoplasms with varying clinical presentations, prognoses and responses to treatment.
Approximately 80,000 new cases per year in US.
Incidence for all lymphoid neoplasms 33.6 per 100,00 persons per year, 26 for B-cell neoplasms and 1.79 for T-cell neoplasms, and 2.67 for Hodgkin lymphoma.
About one fourth of newly diagnosed patients will die of the disease.
Prognosis of lesions vary enormously and depends mostly on the subtype of lymphoma.
There is biologic and clinical heterogeneity of different types of lymphoma that is reflected in the prognosis, treatment, and cure rate among different types of lymphoma.
Diagnosis involves integration of multiple clinical, histological, and immunophenotypic findings as well as, cytogenetic and molecular results.
Treatment is predicated on appropriate identification of the lesion by a hematopathologist.
Clonal neoplasms characterized by abnormal lymphoid cells that may develop in any organ.
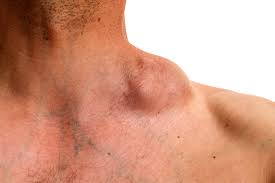
Most commonly involved sites are lymph nodes.
There are more than 70 distinct neoplasms according to the World Health Organization classification.
Classified generally as trauma to the biopsy specimen by compression and cauterization can lead to an artifacts and difficulty in interpretation of findings.
Diagnosis includes evaluation the architectural pattern larger biopsy specimens are pref2241ed.
Excisional biopsies of tissue frequently contain more diagnostic material than core needle biopsies and allow the pathologist more material to submit for testing that requires unfixed tissue.
Needle biopsies are increasingly being performed because of simplicity, fewer complications and lower cost than excisional biopsies.
Needle core biopsies may not provide a representative pattern of architectural abnormalities.
Deeply seated lymph nodes may require needle core biopsy is the best diagnostic option.
Clinical history is essential in evaluating the diagnosis of a lymphoma and includes age, gender, location, symptoms, associated medications, prior history of maligimmunosuppression or immunodeficiency, patient occupation, history of exposure to animals and tattoos
Lymph node architecture is evaluated for pattern of infiltration, such as nodular, diffuse, interfollicular, inttrasinoisoidal and the degree of alteration of normal architecture are reviewed at low magnification.
Cell distribution along with the histological characteristics such as size, shape, chromatin configuration, nucleoli, amount of cytoplasm are key factors for diagnostic and classification purposes.
Immunophenotypic analysis by Immunohistochemistry, flow cytometry or a combination help confirm the neoplastic nature of the process, and its subclassification.
Immunophenotypic evaluation is essential because the lineage of lymphoma cells cannot be determined by morphology alone.
The immunophenotype refers to the combination of proteins/markers expressed by cels e.g., CD20, CD3, TdT.
Immunohistochemistry is normally performed on formalin-fixed and paraffin-embedded tissue.
Flow cytometry can be evaluated only on fresh unfixed tissue.
The B-cell lymphomas have a variable and distinctive histological pattern.
Diffuse infiltrate of large mature cells are typical of diffuse large B cell lymphoma.
Nodular infiltrates of small, intermediate and/or mature large T cells indicates follicular lymphoma.
Mature T-cell lymphomas may have similar histologic features and are heterogeneous with an infiltrate composed of one predominant cell type or a mixture of small, medium, and large atypical lymphoid cells and a variable numbers of eosinophils, plasma cells, macrophages and B-cells.
Maturity of lymphoid cells determined by the nature of the chromatin which is fine and homogeneous when immature, whereas clumped, vesicular or hyperchromatic is generally associated with maturity.
When chromatin displays immature features, lymphoma differential diagnosis will include B- and T-cell lymphoblastic lymphomas, but also blastoid variants of mature neoplasms such as mantle cell lymphoma, and follicular lymphoma, as well as high-grade B- cell lymphomas.
Low-grade lymphomas such as follicular lymphoma , small lymphocytic lymphoma/chronic lymphocytic leukemia, marginal zone lymphoma , lymphoplasmacytic lymphoma include small cell morphology, mature chromatin, absence of significant number of mitoses or apoptic cells, and a low proliferation index as shown by immunohistochemistry for Ki67.
High-grade lymphomas, such as lymphoblastic lymphoma, Burkitt lymphoma, or certain large B-cell lymphomas show opposite features from above, and some of the mature entities are frequently associated with MYC rearrangements.
Immature lymphomas tend to be clinically high-grade, but not all clinically high grade lymphomas are immature.
Conversely the majority of low-grade lymphomas are usually mature.
Hodgkin’s lymphoma most commonly effaces lymph nodes with a nodular or diffuse infiltrate composed of reactive lymphocytes, granulocytes, macrophages, and plasma cells and usually a minority of large neoplastic Reed-Sternberg cells and or lymphocyte predominant cells.
Histological evaluation attempt to determine whether there are mature or immature features present, and whether low or high grade morphologic characteristics are present.
The most sensitive of all malignancies to radiotherapy.
48 or more subtypes are recognized.
Primary pulmonary involvement by lymphoma is rare with 0.5-1% of all lung neoplasms and 3.6% of all lymphomas.
Most lymphomas are FDG-avid.
The most common lymphomas including Hodgkin’s disease, diffuse large B-cell lymphoma, and follicular lymphoma are always avid at presentation.
FDG avidity related to tumor cells but also to environmental cells.
In Hodgkin’s disease the mass is about 1% of tumor cells and the FDG uptake is related to accessory cells amplify by cytokines produced by the Reed-Sternberg cells.
In diffuse large cell B-cell lymphoma the tumor cells makeup 90% of the mass and the FDG uptake results are from the tumor component.
The degree of avidity with the maximum standard uptake value (SUV) corresponds to aggressiveness of lymphomas and a SUV of 14 or more is suggestive of transformed lymphoma.
Lymphoma diagnosis should be considered in patients with cholestasis but no obvious biliary obstruction.
Lymphoma can affect liver function by intrahepatic cholestasid from infiltrative disease, extrahepatic cholestasis due to bulky lymph node disease and liver ischemia and liver failure from compression of extrahepatic for intrahepatic circulation and viral infections associated with immunosuppression of lymphoma.

One reply on “Lymphoma”
[…] large cell B-cell lymphoma is an aggressive extranodal non-Hodgkin’s […]