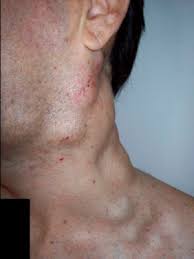
 Lymphadenopathy refers to the enlargement of lymph nodes which can be secondary to bacterial, viral, or fungal infections, autoimmune disease, and malignancy.
Lymphadenopathy refers to the enlargement of lymph nodes which can be secondary to bacterial, viral, or fungal infections, autoimmune disease, and malignancy.
The lymphatic system is a component of the immune system involved in filtering substances in the body, and lymphocytes are involved in searching for target proteins and travel through lymph nodes throughout the body.
Lymph nodes are small glands that filter fluid from the lymphatic system.
Lymph nodes are divided into follicles, which are subdivided into B zones and T zones, which represent the base location for lymphocytic maturation.
The proliferation of lymphocytes may be a result of inflammation, infection, or malignancy.
Inspecting for lymphadenopathy includes examine all pertinent anatomic regions, including the neck, supraclavicular, axillary, and inguinal regions.
In general, the size of a normal lymph node in the adult population should be less than 1 cm.
There are several potential causes of lymphadenopathy: infectious, autoimmune, malignant, and lymphoproliferative.
There is a wide range of infectious etiologies, including bacterial, fungal, viral, mycobacterial, spirochetal, and protozoal organisms.
Autoimmune disorders include:sarcoidosis, amyloidosis, systemic lupus erythematosus, rheumatoid arthritis, and eosinophilic granulomatosis with polyangiitis.
Malignant diseases: lymphoma, leukemia, metastatic cancer, and head and neck cancers are common causes of lymphadenopathy.
Lymphoproliferative disorders can also manifest with the enlargement of lymph nodes.
Lymphadenopathy can be localized or diffuse.
About 75% of most lymphadenopathies are localized, and about 50% of those occur in the head and neck regions.
Generalized lymphadenopathy, which involves two or more non-contiguous regions, is reported to occur in 25% of lymphadenopathies.
A history and physical exam are one of the most important steps in determining the underlying cause of lymphadenopathy.
Submental and submandibular lymphadenopathy commonly is infectious in origin, often presenting with viral prodromes.
Posterior cervical lymphadenopathy can arise from localized bacterial and viral infections, as well as lymphoma.
Axillary lymphadenopathy can also be related to lymphoma or breast malignancy but can be involved by infections such as cat-scratch disease.
Inguinal lymphadenopathy can be impacted by local sexually transmitted infections, lymphoma, and pelvic malignancies.
A majority of cases of lymphadenopathy have a benign etiology.
Age is an important factor in characterizing the epidemiology of lymphadenopathy.
Children more commonly appear to have benign causes of lymphadenopathy.
Among children who underwent a peripheral node biopsy, the most common etiology noted was reactive hyperplasia of unknown etiology, followed by granulomatous infections, cancer, and dermatopathic lymphadenopathy.
In a family practice setting where only 3% of 249 adult patients with lymphadenopathy underwent biopsies, no one was found to have a debilitating illness.
A Dutch study also revealed that of 2556 patients that presented with unclear lymphadenopathy, 10% were referred for a biopsy, and only 1.1% were found to be related to malignancy.
Endemic regions have increased rates of lymphadenopathy due to tuberculosis, parasitic infections, and HIV.
Lymph nodes are a part of the reticuloendothelial system, which includes monocytes of the blood, macrophages of the connective tissue, thymus, spleen, bone marrow, bone, mucosa-associated lymphoid tissue of visceral organs, lymphatic vessels, and lymphatic fluid found in interstitial fluid.
Lymphatic fluid moves throughout the lymphatic system, transitioning from the organs to lymphoid capillaries, lymphatic vessels, and finally lymph nodes for foreign antigen filtration.
Foreign substances are presented to the lymphoid cells, which may lead to cellular proliferation and enlargement: cellular proliferation in lymphoid follicles may be identified as several mitotic figures.
As lymphatic capsules stretch due to increased activity, patients may experience localized tenderness.
The development of B-cells originates from pluripotent stem cells from the bone marrow.
B cells that successfully build their immunoglobulin heavy chains migrate to the germinal centers to allow for antibody diversification by somatic hypermutation.
B-cell lymphomas are believed to be a result of alternations in somatic hypermutation and chromosomal translocations.
The development of T-cells also begins from pluripotent stem cells, which mature within the thymic cortex.
While in the thymic cortex, T cells begin specific rearrangements at the T-cell receptor.
Chromosomal translocations at the level of T-cell receptors lead to T-cell lymphomagenesis.
Lymph node histology can provide further information regarding the cause of lymphadenopathy when etiology is not clear during history and physical examination.
When palpating lymphadenopathy, one must keep in mind location, size, firmness, and pain.
Location:
Anterior cervical lymph nodes are superior and inferior to the sternocleidomastoid muscle.
Posterior cervical lymph nodes are posterior to the sternocleidomastoid muscle.
One should also inspect for supraclavicular, axillary, and inguinal lymphadenopathy bilaterally.
Local lymphadenopathy suggests a more localized disease as compared to widespread lymphadenopathy.
Size: Cervical lymph nodes and axillary nodes are atypical if > 1 cm, as compared to supraclavicular > 0.5 cm, and inguinal nodes >1.5 cm.
Firmness: Generally, if a lymph node is readily mobile, it is less concerning for a malignant condition.
Pain: Pain can be a sign of inflammation, an acute reaction to an infection, and is less concerning for a malignant process.
Diagnostic approach to evaluate lymphadenopathy:
1. Laboratory evaluation: blood chemistries including complete blood count with differential, complete metabolic panel, lactate dehydrogenase, fungal serologies (histoplasmosis, blastomycosis, coccidioidomycosis, cryptococcosis), laboratory evaluation of Syphilis, HIV, CMV, EBV, HSV, HBV, QuantiFERON for tuberculosis.
2. Imaging: Computed Tomography (CT) of the chest, abdomen, and pelvis can be used to further substantiate the location of lymphadenopathy, pattern, and size.
This can also guide a biopsy if needed.
3. Lymph node biopsy: The need for a lymph node biopsy depends on the etiology of lymphadenopathy.
An excisional node biopsy is the gold standard for diagnosis.
Treatment differs depending on the etiology of lymphadenopathy.
1. Malignant: Surgery +/- radiation therapy +/- chemotherapy.
2. Autoimmune: Immune therapy, systemic glucocorticoids.
3. Infectious: Antibiotic therapy, antiviral therapy, or antifungal therapy.
4. Medication: Discontinuation of medication with re-evaluation is necessary.
Causes of lymphadenopathy include but are not limited to:
Malignant:
Autoimmune:
Infectious: Many different infections can contribute to benign changes in the lymph nodes.
Consider several different subcategories of infection, including bacterial, viral, and other: Bacterial: brucellosis, cat-scratch disease, bacterial pharyngitis, syphilis, tuberculosis, tularemia, typhoid fever Viral: cytomegalovirus, hepatitis, herpes simplex, HIV, mononucleosis, rubella, viral pharyngitis. Other: bubonic plague, blastomycosis, coccidioidomycosis, cryptococcosis, histoplasmosis, toxoplasmosis
Medications: Allopurinol, hydralazine, penicillin, phenytoin, primidone, pyrimethamine, quinidine, sulfonamides, and sulindac
Generally, lymph node enlargement in younger populations tends to be benign and usually related to infection.
There are exceptions to the rule: chronic infection, malignancy, or autoimmune conditions.
Risk factors that may be poor prognostic indicators include but are not limited to advanced age, length of duration of lymphadenopathy (> 4 weeks is concerning), generalized lymphadenopathy, male sex, lack of resolution of node size, and systemic signs of fever, night sweats, weight loss, hepatosplenomegaly.
