 Sensitivities in the general population estimated to be between 1% and 6%.
Sensitivities in the general population estimated to be between 1% and 6%.
Latex allergy is a medical term encompassing a range of allergic reactions to the proteins present in natural rubber latex.
Latex allergy generally develops after repeated exposure to products containing natural rubber latex.
Latex-containing medical devices or supplies come in contact with mucous membranes, and the membranes may absorb latex proteins.
In susceptible persons, the immune system produces antibodies that react immunologically with these antigenic proteins.
Rubber latex is found in shoe soles, pen grips, hot water bottles, elastic bands, rubber gloves, condoms, baby-bottle nipples, and balloons.
So there are many possible routes of exposure that may trigger a reaction.
People with latex allergies may also have or develop allergic reactions to some fruits, such as bananas.
Allergic reactions to latex range from Type I hypersensitivity, the most serious form of reaction, to Type IV hypersensitivity.
The rate of onset is directly proportional to the degree of allergy: Type I responses will begin showing symptoms within minutes of exposure to latex, while Type IV responses may take hours or days to appear.
Most commonly, latex allergy presents with hives at the point of contact, followed by rhinitis.
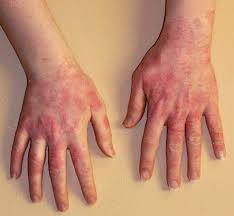
The most common physiological reaction to latex exposure is dermatitis at the point of contact.
Dermatitis causes soreness, itching, and redness.
Angioedema is also a common response to oral, vaginal, or rectal contact with latex.
Symptoms of more severe hypersensitivity include both local and generalized hives; feelings of faintness or impending doom; angioedema; nausea and vomiting; abdominal cramps; rhinitis; bronchospasm;
and anaphylaxis.
Type IV responses typically include erythema, blistering itching, and crusting at the point of contact.
This contact dermatitis is considered a nonimmune reaction to latex.
The degree of reaction is directly proportional to the duration of exposure, as well as skin temperature.
Latex allergy: 40% will experience irritant contact dermatitis; 33% will experience a Type I allergic reaction; 20.4% will experience Type IV allergic contact dermatitits; and 6.5% will experience both Type I and Type IV symptoms.
Occupational populations that frequently utilize latex gloves as barrier protection such as healthcare professionals and hospital staff have high levels of allergy.
Such occupational environmental exposures to latex occur through direct skin contact and from contaminated aerosolized powder from gloves, toy balloons, or any other dusted latex material.
When individuals frequently put on and pulling off powdered latex gloves, such as hospitals and other health care settings, there is an increase the rate of airborne latex allergens and subsequent sensitivity.
Hospital workers are particularly at risk due to the prevalence of latex in gloves, tourniquets, elastic bandages, bag valve masks, and urinary catheters.
Additional occupations that have increased exposure to latex gloves and other supplies, and have higher rates of latex allergy or irritation compared to the general population, include: hairdressers,housekeepers, service workers, and manufacturers in the
industrial rubber industry.
Individuals with chronic health problems have a greater exposure to latex containing materials and a higher risk of late allergy.
Latex allergy may develop in athletes whose sports equipment includes natural rubber, such as swimsuits or running shoes.
Rubber basketballs, may lead to contact dermatitis on the hands and fingertips.
The sensitization to latex in athletes may be accelerated by the use of topical analgesics and other agents that diminish the skin barrier.
Young children may develop a latex allergy due to exposure to from objects such as rubber balloons, boots, gloves, and toys.
People with spina bifida often have latex allergies.
People with latex allergy also may have or develop an allergic response to some plants and/or products of these plants:
known as the latex-fruit syndrome.
Fruits involved in this syndrome include banana, avocado, chestnut, kiwifruit, mango, passionfruit, fig, strawberry, papaya, apple, melon, celery, potato, tomato, carrot, and soy.
The proteins in these fruits are similar to latex proteins: Hevein-like protein domains are a possible cause for allergen cross-reactivity between latex and banana or fruits in general.
Natural rubber latex contains several conformational epitopes located on several enzymes such as Hev type.
FITkit is a latex allergen testing method for quantification of the major natural rubber latex (NRL) specific allergens of Hev types.
Prevention: best accomplished primary prevention towards latex sensitization is limiting or completely avoiding contact with latex.
Reducing exposure to powdered latex glove in hospital settings is an effective primary prevention strategy among adult health care workers.
Estimates suggest a worldwide prevalence of latex allergy is around 4.3% among the general population.
In the US 1%-6% of the general population has latex allergy.
Antibody levels in the blood suggest that 2.7 million to 16 million Americans are affected by some form of latex sensitivity.
Females are approximately three times as likely as males to have latex allergies: increased employment in high-risk occupations and enhanced histamine release caused by female hormones.
There are numerous alternatives to latex include:
Synthetic rubbers, Products made from guayule natural rubber emulsions
which reduce exposure to latex allergens while otherwise retaining the properties of natural rubber, and polyurethanes.
These products are made using chemical treatment to reduce the amount of antigenic proteins in Hevea latex.
Some people are so sensitive that they may still have a reaction to replacement products made from alternative materials, when the alternative products are manufactured in the same facility as latex-containing products, leaving trace quantities of natural rubber latex on the non-latex products.
High risk groups include healthcare workers, spina bifida patients, and patients who have multiple surgeries.
Should be considered when unexplained cardio-respiratory compromise occurs during surgery.
Airborne exposure to latex can lead to systemic reactions in sensitized individuals, including anaphylaxis.
