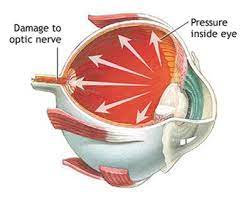
 The internal pressure of the eye, is regulated by resistance to the flow of aqueous humor through the fine sieve of the trabecular meshwork.
The internal pressure of the eye, is regulated by resistance to the flow of aqueous humor through the fine sieve of the trabecular meshwork.
Contraction or relaxation of the longitudinal muscles of the ciliary body affects the size of the opening in the meshwork.
Normal intraocular pressure as that between 10 mmHg and 20 mmHg.
The average value of intraocular pressure is 15.5 mmHg with fluctuations of about 2.75 mmHg.
Intraocular pressure varies throughout the night and day.
Tonometry measurements can, for example, vary between examiners differing by approximately 10% per individual, which can translate to a difference in IOP measurement of 1 mmHg to 2 mmHg.
An individual’s corneal thickness or diurnal variations of IOP (e.g., higher IOP in early morning hours or other time of the day, or variability in the time of day of maximal IOP between patients) can also have a tremendous effect on the accuracy of IOP measurements.
Multiple measurements should be taken in any patient suspected of having an elevated IOP, while correlating measurements with both optic nerve and visual field examinations.
Different instruments may capture different values of IOP.
The diurnal variation for normal eyes is between 3 and 6 mmHg.
Variation in intraocular pressure may increase in glaucomatous eyes.
During the night, intraocular pressure usually decreases because there is slower production of aqueous humour.
Intraocular pressure also varies with heart rate, respiration, exercise, fluid intake, systemic medication and topical drugs.
Alcohol consumption decreases intraocular pressure and caffeine may increase it.
Ocular hypertension is defined by intraocular pressure being higher than normal, in the absence of optic nerve damage or visual field loss.
Ocular hypertension is the most important risk factor for glaucoma.
Differences in pressure between the two eyes may be clinically significant, and potentially associated with certain types of glaucoma, iritis or retinal detachment.
Some forms of refractive surgery, such as photorefractive keratectomy, can cause traditional intraocular pressure measurements to appear normal when in fact the pressure may be abnormally high.
Intraocular pressure may become elevated due to inflammation of the eye, genetic factors, as a side-effect from medication, and exercise.
Increases with age and is genetically influenced.
In the elderly the trabecular meshwork may become sclerotic and obstructed, preventing the normal flow of aqueous humor from passing out at the proper rate and causing an increase in the intraocular pressure.
Low intraocular pressure, hypotony, or ocular hypotony, is typically defined as intraocular pressure equal to or less than 5 mmHg.
Ocular hypotony could indicate fluid leakage and deflation of the eyeball.
