 1664
1664
A rare hereditary blistering skin disease.
Usually appears in the third or fourth decade, although it can occur at any age.
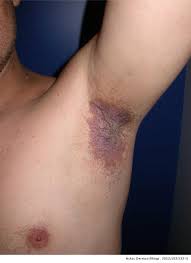
Painful erosive skin rash in the skin folds, with common sites include the armpits, groins, and neck, under the breasts and between the buttocks.
The lesions have a tendency to come and go, leave no scars, but leaves a typical ring shape.
Lesions may become thickened, macerated, cracked and secondarily infected.
Commonly localized to the skin folds, including the neck, axilla, groin, and inframammary area.
Fingernails mat have white bands and the palms may be pitted.
Worsened by heat, sweat, and friction and is worse in the summer.
Inherited skin disorder, but occasionally sporadic in onset.
The defect responsible is on the gene ATP2C1 found on chromosome 3q21-24, which codes for the protein SPCA1 (Secretory Pathway Calcium/manganese-ATPase), a calcium and manganese pump.
The above gene codes for calcium/manganese ATPase pump that helps desmosomes to function properly.
Desmosomes which cause skin cells to stick together do not work properly with insufficient calcium.
Desmosome decompensation results from this gene mutation leading to loss of cohesion between epidermal keratinocytes, a process known as acantholysis.
No diagnostic test available to family members.
Diagnosed by its appearance and the family history, but may require biopsy to distinguish it from other blister disorders.
Histologic characteristic changes demonstrate with layers of detached skin cells.
Acantholysis leads to recurrent flaccid vesiculobullous lesions.
The above lesions erode into plaques with a fissured appearance.
These lesions develop crusts, scales, and hypertrophic vegetations.
Lesions have a tendency to become secondarily infected with bacteria and fungi.
Differential diagnosis includes pemphigus, herpes simplex infection, and Darier’s disease.
Onset usually begins in the third and fourth decades and is usually inherited in an autosomal dominant fashion with variable expression.
About 30% of cases are due to de novo mutations.
The immunofluorescence test for antibodies is negative.
The disease process waxes and wanes and is known to flare due to trauma, pregnancy, infection, drugs, excessive ultraviolet light, and sweating.
No cure available.
Treatment is aimed at reducing symptoms and preventing flares.
Avoiding trigger factors such as sunburn, sweating and friction.
Corticosteroid creams are effective in treating lesions and preventing exacerbations.
Topical or oral antiobiotics useful for treating and preventing secondary infections.
First-line therapy includes highly potent topical steroids and topical calcineurnin inhibitors.
Secondary infection should be treated with topical or oral anti-microbials.
Avoiding sunburn, conditions that cause friction and sweating is recommended.
Refractory caese have been treated with carbon dioxide laser or dermabrasion.
Cyclosporine, methotrexate, photodynamic therapy or other treatments are available.
Botulinum A toxin injection may be beneficial.
Patients have long remissions and an improvement with age.
