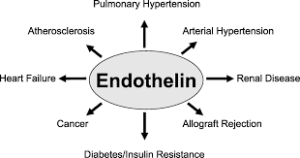
 Endothelins are peptides with receptors and effects in many body organs.
Endothelins are peptides with receptors and effects in many body organs.
Endothelins are a group of peptides that are produced by the cells that line the inner surface of blood vessels, called endothelial cells.
Endothelin constricts blood vessels and raises blood pressure.
The endothelins are normally kept in balance, but when overexpressed, they contribute to hypertension, heart disease, and potentially other diseases.
They play a significant role in regulating various physiological processes, including vascular tone, blood pressure, cell growth, and inflammation.
Endothelins are 21-amino acid vasoconstricting peptides produced primarily in the endothelium.
Endothelins have a key role in vascular homeostasis, and are
implicated in vascular diseases of several organ systems, including the heart, lungs, kidneys, and brain.
There are three isoforms of the peptide (identified as ET-1, -2, -3), each encoded by a separate gene, with varying regions of expression and binding to at least four known endothelin receptors, ETA, ETB1, ETB2 and ETC.
The human genes for endothelin-1 (ET-1), endothelin-2 (ET-2), and endothelin-3 (ET-3) are located on chromosomes 6, 1, and 20, respectively.
Endothelin functions through activation of two G protein-coupled receptors, endothelinA and endothelinB receptor.
The two types of ET receptor are distributed across diverse cells and organs, but with different levels of expression and activity, indicating a multiple-organ ET system.
Most endothelin receptors in the human cerebral cortex, about 90%, are of the ETB subtype.
Endothelin-1 is the most powerful endogenous chemical affecting vascular tone across organ systems.
Secretion of endothelin-1 from the vascular endothelium signals vasoconstriction and influences local cellular growth and survival.
ET-1 has been implicated in the development and progression of several cardiovascular diseases, such as atherosclerosis and hypertension.
Endothelin also has roles in mitogenesis, cell survival, angiogenesis, bone growth, nociceptor function, and cancer onset mechanisms.
Clinically, anti-ET drugs are used to treat pulmonary arterial hypertension.
Endothelin-2 differs from endothelin-1 by two amino acids.
Endothelin-2 sometimes has the same affinity as endothelin-1 for ETA and ETB receptors.
Endothelin-2 plays a significant role in ovarian physiology and could impact the pathophysiology of heart failure, immunology, and cancer.
Endothelins are the most potent vasoconstrictors known.
Overproduction of endothelin in the lungs may cause pulmonary hypertension.
Endothelins have involvement in cardiovascular function, fluid-electrolyte homeostasis, and neuronal mechanisms across diverse cell types.
Endothelin receptors are present in the pituitary, which displays increased metabolic activity when exposed to ET-1 in the blood or ventricular system.
ET-1 contributes to the vascular dysfunction associated with cardiovascular disease, particularly atherosclerosis and hypertension.
The ETA receptor for ET-1 is primarily located on vascular smooth muscle cells, mediating vasoconstriction, whereas the ETB receptor for ET-1 is primarily located on endothelial cells, causing vasodilation due to nitric oxide release.
The binding of platelets to the endothelial cell receptor LOX-1 causes a release of endothelin, which induces endothelial dysfunction.
Among numerous diseases potentially occurring from endothelin dysregulation are:
several types of cancer
cerebral vasospasm following subarachnoid hemorrhage
arterial hypertension, pulmonary hypertension, and other cardiovascular disorders
pain mediation
cardiac hypertrophy and heart failure
Dengue haemorrhagic fever
Type II diabetes
Some cases of Hirschsprung disease
In insulin resistance the high levels of blood insulin results in increased production and activity of ET-1, which promotes vasoconstriction and elevates blood pressure.
ET-1 impairs glucose uptake in the skeletal muscles of insulin resistant subjects, thereby worsening insulin resistance.
Receptors for endothelin-1 exist in brain neurons, indicating a potential role in neural functions.
Peptides with vasoconstrictor activity.
Higher concentrations associated with worse prognosis in congestive heart failure.
