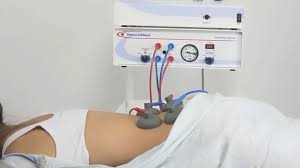
 Electroanalgesia is a form pain relief, that uses electricity to ease pain.
Electroanalgesia is a form pain relief, that uses electricity to ease pain.
Electrical devices can be internal or external, at the site of pain or throughout the whole body.
It interferes with the electric currents of pain signals, inhibiting them from reaching the brain and inducing a response.
It differs from traditional analgesics, such as opiates which mimic natural endorphins and NSAIDs that help relieve inflammation and stop pain at the source.
Electroanalgesia has a lower addictive potential and poses less health threats.
It works by delivering electric currents to specific areas of the body to modulate pain signals in the nervous system.
This form of therapy is based on the gate control theory of pain, which suggests that the sensation of pain can be altered or blocked by interfering with the transmission of pain signals to the brain.
Forms of electroanalgesia, include: Transcutaneous Electrical Nerve Stimulation (TENS), interferential therapy, neuromuscular electrical stimulation (NMES), and percutaneous electrical nerve stimulation (PENS).
Electroanalgesia is commonly used for both acute and chronic pain conditions, such as musculoskeletal pain, neuropathic pain, postsurgical pain, and arthritis.
It is considered a safe and non-invasive treatment option with minimal side effects when used appropriately.
Electroanalgesia can cause serious health problems, even death, in people with other electrical devices such as pacemakers or internal hearing aids, or with heart problems.
Transcranial electrostimulation mechanism of pain reduction by suggests that the electrical stimulation activates the anti-nociceptive system in the brain, resulting in β-endorphin, serotonin and noradrenaline release.
TCES can be used on people with cervical pain, chronic lower back syndrome, or migraines.
Transcranial electrostimulation is not used with orthopedic or radiological potentially serious spinal conditions, hydrocephalus, epilepsy, glaucoma, malignant hypertension, pacemaker or other implanted electronic device; recent cerebral trauma, nervous system infection, skin lesions at sites of electrode placement; oncological disease; patients undergoing any other treatments for pain; any invasive therapy within the last month.
The equipment used consists of a headset with three electrodes, two that go behind the ears and one that goes on the forehead, that release set frequencies of electricity at set intervals.
The mechanism of deep brain stimulation is unknown.
This method has mainly been used for chronic pain patients after all other options have failed due to potential of intracranial complications.
An electrode is guided to the site using magnetic resonance imaging and once in place, the electrode is activated by subcutaneous leads attached to a pulse generator under the skin.
It is effective in treating refractory post-stroke pain, atypical face pain, anaesthesia dolorosa, and pain such as in phantom limb or brachial plexus injury.
Electrical stimulation of nerves leads to inhibitory input to the pain pathways at the spinal cord level.
PNS is most effective in the treatment of neuropathic pain due to posttraumatic neuropathy, or diabetic neuropathy) when the nerve lesion is distal to the site of stimulation.
Percutaneous electrical nerve stimulation is used mainly in the treatment of intractable pain associated with chronic low back pain syndrome, cancer, and other disorders.
Percutaneous electrical nerve stimulation involves insertion of an ultra-fine acupuncture needle into the soft tissues or muscles to electrically stimulate nerve fibers in the sclerotomal, myotomal, or dermatomal distribution corresponding to the patient’s pain symptoms: Percutaneous neuromodulation therapy.
Transcutaneous electrical nerve stimulation, or TENS, involves the transmission of electrical energy from an external stimulator to the peripheral nervous system via cutaneously placed conductive gel pads.
TENS can be subclassified into two variants:
low-intensity high-frequency TENS; and
high-intensity low-frequency TENS.
Transcutaneous acupoint electrical stimulation, or TAES, is a variant of TENS therapy.
Transcutaneous acupoint electrical stimulation involves applying cutaneous electrodes at acupoints and stimulating with alternating high- and low-frequency electric current,
Acupoint stimulation is as effective as dermatomal stimulation in producing an analgesic-sparing effect after lower abdominal surgery.
H-wave therapy (HWT) is a form of electrical stimulation that produces a direct, localized effect on the conduction of underlying nerves.
H-wave therapy (HWT) has been used in the treatment of pain related to diabetic neuropathy, muscle sprains, temporomandibular joint disorders, type I complex regional pain syndrome as well as the healing of wounds such as diabetic ulcers.
Randomized controlled trial found analgesic effects of HWT were found to be short-lasting and identical to those provided by TENS therapy.
HWT is not effective in reducing pain in cases other than diabetic neuropathy, nor has it been shown effective in reducing edema or swelling, and it has specifically not been shown effective in treating chronic pain due to ischemia.
Interferential current therapy is another variant of TENS that uses the amplitude modulation to decrease the discomfort of stimulating deeper tissues (muscle) when using transcutaneously applied electric current.
It is used widely in the physiotherapy and rehabilitative medicine settings, but there is a dearth of rigorously controlled studies to justify its effectiveness in the management of either acute or chronic pain.
Piezo-electric current therapy, or PECT, is an analgesic technique based on the mechanical deformation of a motorized piezoelectric ceramic rod produces a burst of 10 electrical pulses, five positive and five negative, each lasting 2–3 ms, and is supposedly associated with the release of endogenous endorphins.
Electroanalgesia poses serious health problems in patients who need other electrical equipment in their bodies, such as pacemakers and hearing aids, because the electrical signals of the multiple devices can interfere with each other and fail.
These devices can throw off the normal electrical signal of the heart.
