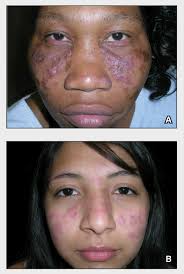
 Discoid lupus erythematosus is the most common type of chronic cutaneous lupus.
Discoid lupus erythematosus is the most common type of chronic cutaneous lupus.
It is an autoimmune skin condition on the lupus erythematosus spectrum of illnesses.
Discoid lupus has an unknown incidence, although it is two to three times more common than systemic lupus erythematosus.
IT tends to affect young adults, and women are affected more than men in a 2:1 ratio.
It presents with red, painful, inflamed and coin-shaped patches of skin.
Skin lesions first present as dull or purplish red, disc-shaped flat or raised and firm areas of skin.
Subsequently these lesions develop increasing amounts of white, adherent scale, and develop extensive scarring and/or atrophy, as well as pigment changes.
On darker skinned people the lesions often lose skin pigmentation in the center and develop increased, dark skin pigmentation around the rim.
On lighter skinned individuals the lesions often develop a gray color or have very little color change.
Rarely, the lesions are bright red and like hive-like.
Most lesions are on the scalp, cheeks, and ears.
Hair loss may occur if the lesions on the scalp.
Severe scarring can develop.
Skin lesions can last for years without treatment.
Patients with systemic lupus erythematous develop discoid lupus lesions frequently.
Patients who present initially with discoid lupus, only infrequently develop systemic lupus.
Discoid lupus can be divided into localized, generalized, and childhood discoid lupus.
Diagnosis requires biopsy of lesions.
Treatment:
Initial treatment with sunscreen and topical steroids.
If this does not work, hydroxychloroquine or a related medication is tried.
Skin lesions are most often in sun-exposed areas above the neck, with favored sites being the scalp, bridge of the nose, upper cheeks, lower lip, and ear and hands.
24% of patients also have lesions in the mouth, especially the
palate, nose, eye, or vulva, which are all mucosal parts of the body.
More rarely, lesions on the head and neck as well as the arms and trunk may appear.
Discoid lupus on the scalp starts as a red flat or raised area of skin that then loses hair and develops extensive scarring.
The lesions often lose skin pigment and become white, with or without areas of redness, and have a sunken appearance.
When discoid lupus lip, involvement it may appear grey or red colour with hyperkeratosis, with erosion, and a surrounding rim of redness.
Skin lesions may be itchy, tender, or asymptomatic.
Other findings include: swelling and redness around the eyes, as well as blepharitis.
Complications of discoid lupus:
Darker-skinned patients often have severe scarring and skin color changes, and an increased, though small, risk for aggressive skin squamous cell carcinoma.
Discoid lupus erythematous is triggered by sun exposure.
Genetics may predispose certain people to disease.
DLE is considered an autoimmune disease.
It is speculated, UV light damages skin cells, to release nuclear material which diffuses to the dermoepidermal junction, where it binds to circulating antibodies, thereby leading to a series of inflammatory reactions by the immune system, or dysfunctional T cells may lead to the disease.
Diagnosis is confirmed through biopsy.
Findings include: deposits of IgG and IgM antibodies at the dermoepidermal junction on direct immunofluorescence.
These findings are 90% sensitive;.
False positives can occur with biopsies of facial lesions.
Other findings include T helper cells, around the follicles and blood vessels in the dermis.
The epidermis is thin and has effaced rete ridges, and excess amounts of keratin clogging the openings of the follicles.
The basal layer of the epidermis sometimes have holes in it.
Dead skin cells are visible in the upper layer of the dermis and the basal layer of the epidermis.
Differential diagnosis: actinic keratoses, sebborheic dermatitis, lupus vulgaris, sarcoidosis, drug rash, Bowen’s disease, lichen planus, tertiary syphilis, polymorphous light eruption, lymphocytic infiltration, psoriasis, and systemic lupus erythematosus.
Classifidied into localized discoid lupus and generalized discoid lupus based on the location of the lesions.
Patients who develop discoid lupus in childhood also have their own sub-type of disease.
Hypertrophic lupus and lupus profundus are distinguished by their characteristic morphological findings.
Many patients with systemic lupus also develop discoid lupus lesions.
Most people with discoid lupus only have lesions above the neck and therefore have localized discoid lupus erythematosus.
Rarely, patients may have lesions above and below the neck; these patients have generalized discoid lupus erythematosus.
Patients with generalized discoid lupus often have lesions on the thorax and the arms, and are often bald, with abnormal skin pigment on their scalp, and have severe scarring of the face and arms.
Patients with generalized discoid lupus often have an elevated ESR or a low white blood cell count, auto-antibodies, such as ANA or anti-ssDNA antibody.
Discoid lupus in childhood affects boys and girls are equally, and these patients later develop SLE more often.
Childhood patients typically do not have any abnormal sensitivity to the sun.
Hypertrophic lupus consists of lesions covered by a very thick, keratin-filled scale.
Lupus profundus is discoid lupus lesions on top of lupus panniculitis, with firm, nontender nodules with defined borders underneath their discoid lupus lesions.
Individuals with discoid lupus who have only skin disease and no systemic symptoms have a genetically distinct disease from patients with SLE.
25% of patients with SLE get discoid lupus lesions at some point as part of their disease.
TREATMENT:
smoking cessation and a sunscreen that protects against both UVA and UVB light as well as very strong topical steroids or intralesional steroids.
Topical treatments, tacrolimus or pimecrolimus can also be used, as well as hydroxychloroquine or chloroquine.
Additionally, oral medications include retinoids, dapsone, thalidomide, azathioprine, methotrexate, or gold.
Pulsed dye laser is also an effective treatment for patients with localized discoid lupus.
DLE is a chronic condition, and lesions will last for several years without treatment.
50% of patients with discoid lupus will get better on their own.
