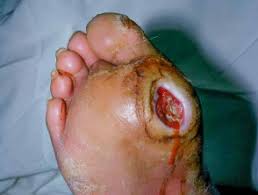
Diabetic foot ulcers affect approximately 1.6 million people in the US and 18.6 million people globally each year.
Such ulcers are associated with impaired physical function, reduced quality of life, and increased health costs.
Untreated foot ulcers can progress to soft tissue infection, gangrene, and limb loss.
Recurrence rate of an ulcer is 70%.
People with diabetes have a 12-25% lifetime risk.
Risk factors include diabetes for more than 10 years, male gender, poor diabetic control, the presence of cardiovascular disease, history of retinal disease, history of renal disease.
Approximately half of people with a diabetic foot foot ulcer have lower extremity peripheral arterial disease.
Other risk factors include the presence of peripheral motor, sensory, or autonomic neuropathy, peripheral vascular disease, impaired vision, previous amputation, impaired mobility, poor attention to protective care of the feet.
About 20% of people with a diabetic foot ulcer will undergo a lower extremity amputation, either minor or major.
Diabetic foot ulcers and amputations are more common among Blacks and Hispanics.
Blacks and Hispanics have more advanced diabetic foot ulcers and peripheral artery, disease at presentation and are more likely to undergo lower extremity amputation.
Comorbidities of foot ulcers in diabetics include diabetic neuropathy, peripheral vascular disease, deformity, and trauma.
Develop secondary to neuropathy, foot deformity,and previous foot ulceration.
Diabetic foot ulcers develop as a result of sensory, motor, and autonomic neuropathy.
Sensory neuropathy leads to loss of protective sensations, motor neuropathy causes foot deformity and biomedical abnormalities, and autonomic neuropathy leads to viscoelastic changes in the skin , such as dryness.
Abnormal pressures on the foot that are not felt during weight-bearing due to lack of sensation can lead to superficial callus formation.
Minor trauma or inflammation, can induce hemorrhage beneath the callus that presents as a ulcer with damage, extending below the epidermidis and dermis into the subcutaneous tissue on the removal of the callus.
Neuropathy results in decreased protection sensation of pain and temperature.
Autonomic neuropathy in diabetes results in foot anhydrosis with dry, brittle skin with fissures and calluses.
Autonomic tone dysfunction causes vascular shunting with a warm foot, distended veins, bounding pulses, impaired nutrition, increased susceptibility to localized gangrene, and poor healing.
Approximately 50% of ulcers become infected, and up to 20% of these patients require hospitalization.
Between 15 and 20% of moderate to severe diabetic foot infections eventually result in a lower extremity amputation.
Patients with a diabetic foot ulcer have a five year mortality rate of 30% and more than 70% for people with an above foot amputation.
Lower extremity ulcers account for 20% of diabetes related hospital admissions.
One in 6 patients with a foot ulcer will require an amputation.
More than 150,000 nontraumatic lower extremity amputations are performed every year in people with diabetes.
25% of diabetics will develop a foot ulcer in their lifetime.
Diabetics with foot ulcers, have a higher death rate than diabetics without foot ulcers.
Most important risk factor for lower extremity amputation.
85% of lower extremity amputations are preceded by a foot ulcer.
Healthcare costs $11,700-16,883 per patient with a foot ulcer.
The direct cause of treating diabetic foot ulcers in the US is estimated to be 9 to $13 billion annually.
Half of patients who develop an ulcer will develop another ulcer on the other side within 3 years.
Simple screening tests for peripheral neuropathy as a predictor of diabetic foot ulcers indicates that tuning fork has a specificity of 90% and sensitivity of 56%.
Stemmes-Weinstein monofilament determines pressure sensation with normal patients with intact can feel for 4.17 monofilament, which equates in 1 g of linear pressure.
Sensation is lost when patients cannot feel 5.07 monofilament with 10 g of linear pressure on the plantar surface of the foot.
Insensitivity of the monofilament increases eight patients likelihood of developing a foot ulcer on the plantar surface who even future lower extremity amputations.
Majority of patients with diabetic foot ulcers will heal with offloading and appropriate wound care, so the real measure for successful outcome is durability of the healing and restoration of function.
Maximum hyperemic response to foot skin microcirculation to heating or minor trauma is impaired in diabetic patients compared to healthy controls.
Hemoglobin oxygen saturation is reduced in the skin of patients with diabetes and this process is accentuated in the presence of neuropathy.
Foot muscle energy reserves are decreased in diabetics.
Endothelial and vascular smooth muscle function are impaired in the microcirculation of diabetics.
Nerve axon-related vasodilation which accounts for up to one third of maximum vasodilatory capacity in healthy individuals is absent in the feet of patients
Classified as neuropathic, ischemic or both.
The presence of peripheral neuropathy in patients with diabetes mellitus increases the risk of foot ulcers and diabetic foot infections 7 fold (Young MJ).
Neuropathic ulcers are the most common type of diabetic foot ulcers and result from tissue damaging mechanical loads on an insensate foot.
The development of diabetic foot ulcers is driven by the effects of sensory neuropathy on foot biomechanics, with foot deformity being associated with high pressures on specific weight bearing areas.
Almost half of patients with diabetic foot ulcers lack pain and numbness.
Injuries that can result in ulcers include trauma or mechanical stress that is repetitive or continuously applied.
Can result from thermal injuries, animal bites, restricted joint mobility, poor foot care, and foot deformities.
Treatment includes smoking cessation, glycemic control, diet management, treatment of hyperlipidemia, optimum blood pressure control and antiplatelet therapy.
To prevent new or recurrent diabetic foot ulcers requires patient education, foot skin and toenail care, and appropriate footwear selection with proactive surgical interventions.
For patients with moderate to severe infections frequently have aerobic gram positive cocci, often mixed with gram negative bacilli and sometimes obligate anaerobes.
Isolates from infections are increasingly resistant, even in individuals with community acquired infections.
The presence of immunosuppression impairs healing and eradication of infection, and increases the risk of amputation, such that the rate of amputation for diabetics with kidney transplantation is at least 15% and for those who survive 10 years the rate increases to 33%.
Foot ulcers and infections in diabetics have a causative role in up to 61% of lower extremity amputations (Ramsey SD).
Traditional therapy is based on cleansing, debridement and eliminating infections.
Standard topical approach includes debridement of non-eschar tissue and appropriate dressings that manage infection and moisture.
The use of hyperbaric oxygen has been reported to reduce the incidence of major amputations in patients with diabetic ischemic foot ulcers, but data is conflicting.
Platelet rich plasma gel may promote healing.
In a meta-analyses tretment with hyperbaric oxygen improved ratevf healing and reduced the ratenof major, but not minor amputations (Liu R et al).
Offloading approach with total contact casting to relieve pressure, and offers a moist environment for healing and allows the patient to ambulate.
