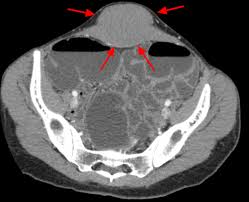
 Benign fibromatous soft tissue sarcomatous tumors with minimal metastatic potential that tend to invade locally and often recur after surgical resection.
Benign fibromatous soft tissue sarcomatous tumors with minimal metastatic potential that tend to invade locally and often recur after surgical resection.
Desmoid tumors are rare, monoclonal,locally aggressive, and highly recurrent, soft tissue tumors.
Aggressive fibromatosis.
Incidence 2-5 cases per million people per year.
Annual incidence is estimated to be 1000 patients in the United States, and the prevalence may be higher.
.03-0.1% of all solid tumors.
Most commonly arises between the ages of 15-and 60 years.
Peak age of 30 to 40 years and a predominance among females.
Typically affects young adults in their 20s and 30s, but can occur in children, adolescents, and older adults.
Desmoid tumors are associated with low mortality, but high morbidity.
The median age is between 30 and 40 years.
Most cases are sporadic, greater than 90% harbor CTNBB2 mutations.
Can occur at abdominal, intraabdominal, and extra abdominal locations and approximately 5 to 10% arise in the context of familial adenomatous polyposis.
Desmoid tumors are typically characterized by genetic mutations in the Wnt-adenomatous polyposis coli – beta -catenin pathway:approximately 90% in sporadic type desmoid tumors: APC in approximately 10% of there’s more tumors associated with familial adenomatous polyposis or Gardner’s syndrome.
A minority of tumors are associated with germline APC mutations and Gardner’s syndrome.
It is associated with an over expression of beta-catenin and highly express Notch1 with cross talk between these pathways contributing to proliferation of desmoid tumors.
Female predominance of 2-3 fold.
More common among women and most frequently occurs in the limb girdle.
Estrogenic influence demonstrated by association with pregnancy.
Extremely rare for a patients to present with multifocal disease.
Tumors can show rapid growth followed by periods of stabilization, spontaneous regression, or subsequent growth phases.
Compression of vital structures can cause pain, functional impairment, nerve damage, bowel obstruction or perforation.
Up to 20% of patients report spontaneous regression.
Incidence is about 1000 times in patients with familial adenomatous polyposis in which adenomatous polyposis gene (APC) is mutated.
Familial adenomatous polyposis associated desmoid tumor is more frequently abdominal tumor, especially in the Gardner variant which is characterized by intestinal polyposis, osteomas, fibrmoas, and epidermal inclusion cysts.
Desmoid- type fibromatosis develops in approximately 5-30% of patients with FAP usually in the mesentery.
Can arise in any anatomical location and infiltrate the mesentery, neurovascular structures, and visceral organs.
Common primary sites include the abdominal wall, mesentery, and neurovascular bundle of the extremities.
They do not metastasize.
With Gardner’s syndrome, but they can cause substantial complications.
Presentation ranges from a symptomatic to severe pain, swelling, deformity, loss of range of motion, bowel obstruction or perforation, or compromise of vital organs.
Desmoid tumors are difficult to manage due to their invasive nature and high rates of recurrence.
Among patients with progressive, refractory, or symptomatic desmoid tumors, sorafenib significantly prolonged progression free survival and induced durable responses: The progression free survival rate was 81% at two years vs, 36% in the placebo group (Gounder MM).
Historically, complete surgical resection was the first line treatment, now there has been a shift to the management of asymptomatic patients to active surveillance.
Patients with gastrointestinal complications of bleeding/bowel obstruction or tumor and abscess would require surgery and in the setting where gross tumor resection is not feasible the goal of the operation should be to manage the complication without necessarily resecting the entire tumor.
Patients who progress on medical treatment or surveillance may require surgery.
Pazopanib have similar activities as sorafenib.
Histological a poorly circumscribed proliferation of myofibroblast-like cells with variable collagen deposition.
Has been associated with trauma, pregnancy, and oral contraceptive use.
Trauma is a common inciting agent.
Surgery may sometimes promotes growth of desmoid tumors.
The natural history is highly variable.
Extra-abdominal tumors are usually sporadic and treated with surgery with or without surgery.
Surgery can be avoided using conservative approach 85% of patients with dermoid tumors of abdominal wall and in more than 90% of those in other sites.
For most patients active surveillance, or systemic therapy is now recommended as first line treatment.
Guidelines, recommend an initial period of active surveillance and continuous monitoring with imaging for asymptomatic tumors that do not cause functional limitations.
For patients with progressive, morbid or symptomatic tumors systemic therapy is now recommended as first line option.
If systemic therapies declined or effective, alternative local control strategies such as radiation ablation may be considered.
Surgery is now a less preferred option.
Radiation may also be effective for primary therapy for extra-abdominal tumor.
From 4-38% of patients with FAP develop desmoid tumors.
Median time of recurrence 23 months with 90% of recurrences by 5 years.
Overall survival rates 90% at 20 years.
Do not dedifferentiate to a high grade malignancy or metastasize.
Rate of local recurrence dependent upon type of resection performed, with a wide local excision offering a recurrence rate of 50% and a recurrence rate of 90% with incomplete resections.
Recurrence rate higher for women and patients over the age of 30 years.
Recurrence rates of 39-79%.
Overall 10 year actuarial recurrence rate 33%.
There is no standard of care.
Watching/ wait strategy is increasingly advocated.
Active surveillance has occurred because the behavior of tumors is unpredictable and spontaneous growth arrest and regression can occur.
Optimum therapy requires pain control.
A period of observation of 12-24 months of surveillance is advised prior to beginning active therapy.
In about half of patients initial progression is followed by tumor stabilization which subsequently can be followed by regression.
In the other half of patients surveilled, persistent disease progression or worsening of symptoms requires active therapy.
Wide local excision with negative margins is the treatment of choice.
Risk of local recurrence rate is greater than 40%.
Unresectable disease should be treated with radiation.
Systemic treatment options include hormonal blockade, cytotoxic chemotherapy, tyrosine kinase inhibitors with a response rate varying between zero and 40%.
Cryoabllation has been reported to be effective for small and moderately sized extraabdominal DT, as may high intensity focused ultrasonography.
Reports of trans arterial chemo embolization with doxorubicin have been reported to have successes.
Endocrine therapy with tamoxifen, and toremifen are to be considered a non-clinical anatomical site tumors.
Low dose chemotherapy with methotrexate and vinblastine/vinorelbine can cause regression or stabilization of disease in many patients.
Among patients with progressive, refractory, or symptomatic desmoid tumors, sorafenib significantly prolonged progression free survival and induced durable responses: The progression free survival rate was 81% at two years vs, 36% in the placebo group (Gounder MM).
Nirogacestat is the first drug approved for desmond tumor, and is associated with significant benefits with respect to progression free survival, objective response, pain, symptom burden, physical functioning, role functioning, and health related quality of life in adults with progressing desmoid tumors.
Nirogacestat is a reversible, gamma secretase inhibitor targeting Notch signaling.
