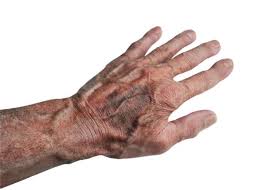
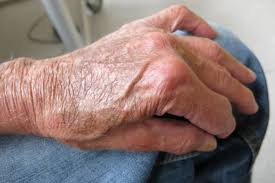
 Dermatoporosis is a clinical condition leading to chronic skin fragility.
Dermatoporosis is a clinical condition leading to chronic skin fragility.
It can be separated into primary and secondary subtypes.
Secondary dermatoporosis induced by medical drugs and environmental factors.
Dermatoporosis can be classified into 4 major stages with increasing morbidity and mortality with advancing stages.
Dermatoporosis is related to the epidermal hyalusome.
It is a cause of mortality in the intensive care unit.
Its prevention is of major importance, but therapeutic options are limited but available.
Cutaneous aging has been divided into intrinsic and extrinsic aging based upon the origin of changes.
Cutaneous aging is include pigmentary, vascular, connective tissue and adipose tissue aspects.
The skin aging process is genetically determined but can be largely be influenced by environmental factors such as ultraviolet radiation, air pollution and smoking.
Dermatoporosis is a loss of function that eventually results in a breakdown of the protective mechanisms of skin.
The primary form is due to increased age and extensive exposure to sunlight from secondary forms due to certain medications.
The prevalence of dermatoporosis in elderly French hospital in-patients aged between 60 to 80 years has been calculated as high as 32%.
A prospective trial of the department of dermatology at Helsinki University analyzed consecutive outpatients aged ≥ 60 years: Dermatoporosis was evident in 30.7% of patients, mainly on the upper limbs (94%).
Dermatoporosis was significantly associated with ultrapotent topical corticosteroids, oral corticosteroids, concomitant corticosteroid therapy, anticoagulants and chronic renal failure while age had only a marginal impact
Patients with bullous pemphigoid have the highest prevalence of dermatoporosis.
In a French study the estimated overall prevalence of dermatoporosis was 37.5% in subjects aged older than 65 years with a predominance of women.
Dermatoporosis has been staged into 4 stages.
Stage I: Skin atrophy, senile purpura and pseudo-cicatrices
Stage IIa: Localised and small superficial lacerations (< 3 cm) due to skin fragility
Stage IIb: Larger lacerations (> 3 cm)
Stage IIIa: Superficial hematomas
Stage IIIb: Deep dissecting hematomas without skin necrosis
Stage IV: Large areas of skin necrosis with potentially lethal complications
With corticosteroid-induced skin atrophy, the hyalurosome of filopodia of epidermal keratinocytes becomes weakened.
The hyalurosome of filopodia of epidermal keratinocytes organelle is composed of hyaluronic acid receptor CD44, heparin-binding epidermal growth factor (HB-EGF), HB-EGF receptor erbB1 and hyaluronic acid synthase 3.
The hyalurosome is involved in different functions such as secretion of hyaluronic acid and epidermal growth factor-receptors signalling.
The hyalurosome is anchored on F-actin fibers.
A mouse model suggested that the hyalurosome is the target of corticosteroids and involved in corticosteroid-induced epidermal atrophy and dermatoporosis.
Dermatoporosis skin demonstrates peculiarities in the viscoelastic properties of the affected skin, with residual deformation (RD) significantly increased.
Bateman purpura, or actinic purpura, is a classical sign of photo-aging, characterized by hemorrhagic areas with purpuric eruptions like petechial or confluent ecchymoses, by stellar scars, and a fragile skin due to thinness of the dermis .
Actinic purpura features are mainly localized on the back of the hands and the forearms.
In the the affected parts of the skin, there is a depletion of the photoprotective vitamin C due to chronic ultraviolet light (UV)-exposure.
From stage IIa onwards, laceration (skin tears) is a common feature of dermatoporosis, caused by blunt trauma.
Underlying mechanisms are age-related skin changes, dehydration, malnutrition, sensory changes, mobility impairment, pharmacological therapies and mechanical factors related to skincare practices.
Due to the delayed wound healing, dermatoporosis has a risk of soft tissue infections.
Deep dissecting hematoma is an emergency.
The legs were affected in all patients, most frequently in older women with a mean age 81.7 years.
Deep dissecting hematoma risk factors are long-term treatment with systemic corticosteroids and anticoagulation.
Deep dissecting hematoma presents with pain, swelling, erythema and edema without fever, with skin necrosis as a late symptom.
Treatment consisted of deep incision and/ or debridement followed by direct closure, skin grafting, or wound healing by second intention.
Skin failure, is an event in which the skin and underlying tissue die due to hypo-perfusion that occurs in concomitance with failure of other organs,
Skin failure is defined as loss of normal temperature control with inability to maintain the core body temperature, percutaneous loss of fluid, electrolytes and protein, and failure of the mechanical barrier to prevent penetration of germs.
Risk factors for acute skin failure were peripheral arterial disease, mechanical ventilation greater than 72 hours, respiratory failure, liver failure, and severe sepsis and/or septic shock
Dermatoporosis is a condition that can lead to acute skin failure in the ICU.
Dermatoporosis has a high prevalence in autoimmune bullous disorders such as pemphigoid, and bullous disorders are among the dermatological diagnoses that can lead to an ICU admission
Prevention of dermatoporosis is by limiting the exposure to known inducers of this skin condition: extrinsic factors like ultraviolet radiation, pollution or smoking, and medical drugs like topical and systemic corticosteroids.
Treatment of dermatoporosis had best results are obtained in stage I.
Topical treatment of atrophic forearm skin of dermatoporosis patients with hyaluronic acid 1% for 1 month resulted in a significant clinical improvement.
Other topical modalities to increase skin thickness include alpha-hydroxy acids twice daily for at least three months, or topical dehydroepiandrosterone 1% cream, in women, twice daily for four months.
Topical vitamin C led to a clinically apparent improvement of purpura and measurable improvement of skin elasticity or thickness.
