Pneumonia in individuals who become ill outside the hospital or within 48 hours of admission.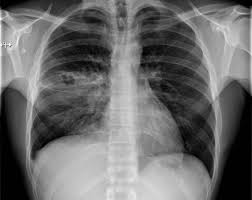
The leading infectious cause of hospitalization and death in developed countries and worldwide.
The most common infection leading to hospitalization and death in all age groups, especially the elderly.
It is associated with substantial, long-term illness and death, with death at one year occurring in approximately 30% of all hospitalized patients, and in approximately 50% of patients whose condition had resulted in an ICU admission.
Approximately 6 million cases are reported each year in the United States.
The annual incidence of hospitalization for CAP in the US is approximately 650 adults per 100,000 population, corresponding to 1.5 million unique hospitalizations for the disease each year.
Factors associated with increased risk of CAP include: advanced age, chronic lung disease, chronic heart disease, cardiovascular disease, diabetes mellitus, malnutrition, viral respiratory tract, infections, immunocompromising conditions, and lifestyle factors, such as smoking, and excessive alcohol consumption.
CAP development is influenced by: host susceptibility, pathogen variance, the inoculum of micro organisms organisms reaching the lower airways.
Numerous microorganisms can cause CAP and include bacteria and viruses, being most likely be etiologic agents.
Respiratory pathogen encounter defense mechanisms of the respiratory system before reaching the alveoli and include: mucus trapping, mucociliary clearance, coughing and swallowing.
The lungs have been considered sterile and healthy and individuals, however healthy lungs contain diverse communities of bacteria, mostly of oropharyngeal origin that are viable and metabolically active and contribute to the hosts dynamic immune defenses.
Presently rather than representing the invasion of sterile space by an overwhelming inoculum of an exogenous pathogen, bacterial pneumonia occurs when an organism emerges as a dominant one.
Pathogens can reach the alveoli by means of microaspiration, inhalation, macroaspiration, or hematogenous spread.
Microaspiration is the primary path for microorganisms into the lungs, and macro aspiration may lead to aspiration pneumonia.
The alveolar macrophages the primary defense mechanism in the lung.
CAP involves proliferation of bacteria, fungal, or viral pathogens with involvement in adjacent small airways, associated with inflammation, disrupted homeostasis, both locally within the lung and systemically.
Local changes in the lung result in dyspnea and cough, impaired gas exchange, and airspace consolidation, while systemic manifestations include fever, fatigue, altered mental status, and potentially sepsis.
CAP is typically treated as an outpatient, but up to 10% of patients are hospitalized.
The incidence of hospitalization due to CAP is approximately 24.8 per 10,000 person-years for all adults, with a higher incidence of 63 per 10,000 person-years in individuals older than 65 years.
30 day mortality after hospitalization for CAP ranges from 2.8% for adults younger than 60 years and 26.8% for those 60 years and older with comorbidity.
There are approximately 1.4 million emergency department visits, 740,000 hospitalizations, 41,000 deaths and $7.7 billion in in patient costs each year in the US.
There is evidence regarding positive outcomes from using oral steroid treatment in community acquired pneumonia.
In hospitalized adults with CAP, systemic corticosteroid therapy may reduce mortality by approximately 3%, need for mechanical ventilation by approximately 5%, and hospital stay by approximately 1 day
The number needed to treat for an additional beneficial outcome was 18 patients (95%) to prevent one death.
Corticosteroid therapy reduced morbidity, but not mortality, for adults and children with non-severe CAP and corticosteroid therapy was associated with more adverse events, especially hyperglycaemia, but the harms did not seem to outweigh the benefits
A systematic review found corticosteroid therapy is associated with a lower incidence of progression to requiring mechanical ventilation among patients hospitalized with CAP.
No association was found between corticosteroid therapy and mortality, treatment failure, or adverse events
Steroid therapy in adults who had been admitted to the intensive care unit (ICU) for severe CAP among patients with severe community-acquired pneumonia being treated in the ICU, those who received hydrocortisone had a lower risk of death by day 28 than those who received placebo.
A review of 18 RCTs found corticosteroids probably reduce mortality in more severe community-acquired pneumonia with moderate certainty and probably reduce risk of requiring invasive mechanical ventilation and ICU admission.
In patients with CAP in a low resource setting, adjunctive steroid therapy was associated with a lower risk of death than standard care (Lucinda R).
Annual cost in excess of $17 billion in the US.
Mortality among hospitalized patients still high, especially in those with severe pneumonia and those who experience treatment failure, which is observed in 10-20% of patients.
Incidence requiring hospitalization is highest among the oldest adults.
Worldwide, 489 million lower respiratory infections occurred in 2019.
In the US more than 1.5 million adults are hospitalized for a community acquired pneumonia annually.
in 2019, approximately 50,000 deaths in the United States, were a result of community acquired pneumonia.
Annual incidence of CAP requiring hospitalization 24.8 cases per 10,000 adults (EPIC).
The monthly death rate among patients who are hospitalized with community acquired pneumonia is approximately 10 to 12%.
Among patients who receive any type of mechanical ventilation, mortality may reach 30% for CAP.
Advanced age, the presence of altered mental status and and vital sign abnormalities increase risk of mortality.
Advanced age is the strongest risk factor for CAP.
Specific pathogens are not detected in most patients with CAP.
The organisms responsible as noted are usually not confirmed as noted, but S. Pneumoniae and mycoplasma pneumoniae are common causative pathogens.
Other pathogens include H. Influenzae, Moraxella catarrhalis,Chlamydophilia pneumonia, Legionella species, Staphylococcus aureus, and anaerobic mouth organisms.
Viral pathogens are common in CAP, but are considered to have bacterial pneumonia at the time of admission due to the absence of widely testing for the full range of pathogens
As a result of the above initiation of empirical antibiotic therapy covering the most likely bacterial pathogens is the standard of care.
Patients greater than 65 years hospitalized with CAP have a overall mortality in 30 days of 6.5%.
WHO estimates pneumonia is the most common infectious cause of death in the world, the third most common cause overall, with almost 3 1/2 million deaths yearly.
Accounts for approximately 5.6 million cases and 1 million hospitalizations yearly in the U.S.
Estimated 50,000 this into thousand and 10 attributed to pneumonia and this is probably an under estimate.
Medical costs exceeding $10 billion in 2011 for CAP.
Affects approximately 1% of adults annually.
Annual incidence of 12 episodes per 1000 persons.
More than 900,000 cases in adults over the age of 65 years annually with an incidence of 8.2 cases per 1000 person-years for individuals 65-69 years of age, 27.9 cases per 1000 persons-years for patients aged 75-79 years and 52.3 cases per 1000 person-years for those greater than 85 years of age.
Estimated incidences of hospitalization for CAP among adults 50-64 years, 65-79 years, and 80 years of age or older ARE approximately 4, 9, and 25 times as high, respectively, as the incidence among adults 18-49 years of age ( Etiology of Pneumonia in the Community (EPIC).
In the above study of 2488 patients pathogens were found in 38% with viruses detected and 27% and bacteria and 14%.
In the above study human rhinovirus, Influenza virus, and S. pneumoniae with the most common detected pathogens, with the highest burden occurring among older individuals.
In children pathogens are detected in approximately 80% of cases of hospitalized patients with CAP.
Amoxicillin is widely recommended as the first line antibiotic for CAP in young children.
Among children with CAP discharged from an ED or hospital a lower dose of outpatient oral amoxicillin was not inferior to a higher dose, and a three day duration was not inferior to seven days, with regard to need for antibiotic re-treatment.
Low percentage of diagnosis of pathogens possibly related to the inability to obtain lower respiratory tract specimens, the use of antibiotics before specimen collection, insensitive diagnostic tests, lack of testing for other types of pathogens, unidentified pathogens, and possible non-infectious causes.
For individuals greater than 85 years of age approximately 1 in 20 will have an episode of CAP each year.
Elderly often present with few classic respiratory signs and symptoms but frequently have delirium, progressive confusion and falling episodes.
Current diagnostic tests do not detect the pathogen in the majority of patients.
The biomarker procalcitonin may improve clinical judgment to diagnosis and course of a bacterial community acquired pneumonia, as synthesis a procalcitonin is triggered by specific cytokines in response to bacteria.
Respiratory viruses are detected more frequently than bacteria in acquired CAP hospitalizations among the US adults (Jain S et al).
Patients with severe CAP illness are more likely to have a bacterial cause.
Patients and younger patients who develop CAP are more likely to have viral infections or atypical pathogens such as chlamydia and mycoplasma.
CAP varies by region with pathogens that are considered according to seasonality and geographic regions.
Diagnosis is usually not difficult in patients who do not have underlying cardiopulmonary disease.
Findings include fever, chills, leukocytosis, cough, sputum production, shortness of breath, chest pain, abnormal pulmonary clinical findings, a new or changed lung infiltrate on chest x-ray are usual indications of community acquired pneumonia.
Diagnosis in patients with pulmonary fibrosis, other chronic infiltrative lung diseases, lung cancer, or congestive heart failure is difficult.
Diagnostic delay is common in patients with atypical presentations and you have comorbidities as noted above.
Chest x-ray infiltrates may show only subtle changes and a radiologist may miss findings in 15% of cases, and two radiologists reading the same chest x-ray disagree in 10% of cases.
CT scan of the chest is appropriate if chest x-ray does not support the diagnosis of CAP, but clinical suspicion exists.
because there is a lack of highly sensitive and specific clinical findings or diagnostic test for CAP there is a risk of substantial over diagnosis with approximately 10 to 30% of patients treated for CAP do not meet diagnostic criteria.
The differential diagnosis for pneumonia includes exacerbation of chronic cardiopulmonary diseases, COPD, acute upper airway disease, aspiration pneumonitis, malignancy, and pulmonary embolus.
Associated with a high incidence of silent aspiration in the elderly.
A leading cause of morbidity and mortality worldwide.
Cardiac complications occur in as many as 27% of patients hospitalized for CAP,
Cardiac complications are responsible for one third of clinical failures of treatment of CAP.
Excessive host inflammatory response is associated with treatment failure during ICU admission and mortality.
Cardiac complications are the direct or underlying cause of death and one fourth of CAP associated fatalities.
Approximately 15% of patients require hospitalization.
Chest x-ray is considered the standard for diagnosing the presence of pneumonia.
Most common cause Streptococcus pneumoniae.
Streptococci implicated in nearly 500,000 cases/year.
Approximately 10% of patients over the age of 64 admitted to the hospital die before discharge and many more die within one month of discharge.
Approximately 40% of such infections in the elderly require hospitalization and a mortality rate of 40% occurring within 1 year has been reported.
Most patients treated as outpatients.
Death due to pneumonia in the elderly as high as 20% (Riquelme).
Except for viral testing, only patients with severe CAP or risk factors for methicillin-resistant Staph or Pseudomonas, or those who did not improve with the course of typical antibacterial medications should be evaluated for etiology.
As many associated 59% of elderly patients are readmitted within 18 months.
Overall case-fatality rate of about 5%.
Mortality substantially greater, about 13.6%-among hospitalized patients.
Cardiac complications that develop in CAP patients result in an increase short-term mortality by 60-200%.
Risk factors with increased mortality: age >65 years, COPD, diabetes mellitus, chronic renal failure, congestive heart failure, chronic liver disease, suspicion of aspiration, altered mental status, postsplenectomy, chronic alcohol abuse, malnutrition, respiratory rate >30, diastolic blood pressure < 60 mm Hg, systolic blood pressure <90 mm Hg, temperature >38.3?C, extrapulmonary sites of infection, WBC <4000mm3, Pao2 < 60 mm Hg, Pco2> 50 mm Hg, need for mechanical ventilation, abnormal renal function, rapid radiographic spreading, presence of a pleural effusion, hematocrit < 30%, evidence for sepsis and evidence for DIC.
The Pneumonia severity index (PSI) uses a scoring system to predict 30 day mortality and assignment of care as an in or out-patient with 5 risk classes I-V based on 19 variables in demographic factors, comorbid processes, physical examination findings and laboratory findings.
PSI includes factors such as gender, nursing home resident, presence of altered mental status, types of co morbid illnesses, respiratory rate > 30/min, blood pressure less than 90 mm HG, temperature <35 degrees centigrade or >40 degrees centigrade, pulse rate >125 beats/min, pH <7.35, serum sodium less than 130 mEq/L, BUN > 0 mm/L, hematocrit <30%, PA02 < 60 mm HG and the presence of pleural effusion.
Bacteremia caused by Streptococcus pneumoniae documented in up to 26% of hospitalized patients.
Bacteremia caused by Streptococcus pneumoniae associated with a mortality of 19-28%.
Blood cultures should be done in only the sickest patients with community acquired pneumonia, as routine blood cultures for such patients who are hospitalized have limited utility and false-positive results lead to inappropriate antimicrobial use and longer hospital stays.
The Infectious Diseases Society of America/American Thoracic Society guidelines recommend empirical antibiotics for all hospitalized patients that covers most common typical as well as atypical pathogens.
It is recommended that the first antibiotic dose be administered within six hours after presentation for CAP.
Current recommendations for the duration of antibiotic therapy is 5-7 days for CAP.
Retrospective studies suggest a combination of antibiotics is associated with better outcomes, especially with lower mortality and particularly in patients with severe disease.
Macrolide antibiotics are frequently identified as the key component of combination treatment regimens.
Recommendation for patients who have hypotension is that antibiotics should be given within one hour of presentation.
In patients with septic shock and CAP, a decrease in survival rates of 8% occurs for each hour of delay in the administration of antibiotics (Kumar A et al ).
Fluoroquinolone monotherapy or Beta-lactam plus macrolide combination recommended for hospitalized patients.
Infectious Diseases Society of America and American Thoracic Society guidelines recommend either a beta-lactam plus a macrolide or a respiratory fluoroquinolone.
In a randomized crossover trial patients with suspected CAP admitted to non-ICU wards a strategy of empirical treatment with beta-lactam monotherapy was not inferior to strategies with the beta-lactam-macrolide combination or fluoroquinolone monotherapy with regard to 90 day mortality(Postma DF et al).
The administration to hospitalized patients of either a respiratory fluoroquinolone or the combination of the second-generation or third-generation cephalosporin and a macrolide indicate decrease mortality and length of hospital stay.
Three decisions are made simultaneously when a patient presents with CAP: the choice of antibiotics, the extent of testing to determine the cause, and location of treatment site.
The key initial therapy is to adequately cover for Streptococcus pneumonia and the atypical bacterial pathogens such as mycoplasma, chlamydophylia, and Legionella.
Outpatient coverage of atypical bacterial pathogens is required, especially for young adults, in the agents of choice are macrolides, doxycycline and fluoroquinolones.
For mild to moderate CAP in hospitalized patients antibiotics for 3-5 days is equivalent to longer courses of therapy (Uranga A et al).
Streptococcal pneumonia is still the most common cause of severe community acquired pneumonia requiring ICU admission, the combination of a cephalosporin with either a fluoroquinolone or macrolide is recommended.
In the above setting, results with macrolides may be associated with better outcomes.
Initial intravenous antibiotic therapy may be switched to oral therapy once the patient shows clinical stability even if bacteremia caused by Streptococcus pneumoniae was initially documented.
Sputum culture, Gram stain and pretreatment blood culture recommended for patients hospitalized for CAP but in general treatment is empiric and based on patients age, underlying illness, clinical history and radiographic appearance.
After extensive testing a causative agent is not determined in 50% of cases.
Microbiological testing for bacterial causes is generally not recommended for most patients being treated as an outpatient, since empirical anabiotic therapy is largely successful.
More comprehensive microbiological work up is performed for patient based on previous exposures, patient characteristics and level of immuno suppression.
Mortality low in patients who can be managed as and outpatient but may be 25% or greater in hospitalized patients, especially if they require admission to the ICU.
Evaluation for ambulatory patients include a CXR, CBC and chemistries.
Evaluation for hospitalized patients include CXR, CBC, chemistries, pulse oximetry/arterial blood gas, and blood cultures.
Evaluation for patients with severe CAP include all the above plus Gram stain, sputum culture and Legionella antigen studies.
Differential diagnosis with an abnormal chest x-ray includes: congestive heart failure with associated viral syndrome, aspiration pneumonia, pulmonary infarction, exacerbation of fibrosis, exacerbation of bronchiectasis, eosinophilic pneumonia, hypersensitivity pneumonitis, pulmonary vasculitis, and cocaine induced lung injury.
Pneumonia is diagnosed by a combination of two or more signs temperature greater than 38°C, leucocytosis, new or increased cough or dyspnea of pneumonia in conjunction with radiographic findings without an alternative explanation for the signs, symptoms of radiographic findings.
Severe community acquired pneumonia is associated is a major cause of mortality and despite effective antibiotic therapy 12-36% of patients admitted to the ICU die within a short period of time.
Patients with risk class V for Pneumonia severity Index also have a high mortality risk.
Increased serum levels of cytokines IL-6, IL-8, and IL-10 in severe community acquired pneumonia.
Excess serum levels of IL-6 and IL-10 are associated with high mortality rate among patients with community acquired pneumonia.
Use of corticosteroids remains controversial except in patients patients with severe pneumonia and high inflammatory responses, defined as CRP level greater than 150 mg/L at admission.
In the above situation that acute administration of methylprednisolone is associated with less treatment failure and lower inflammatory response.
Among patients with severe community acquired pneumonia, being treated in an ICU, those who received hydrocortisone, had a lower risk of death by day 28, than those who receive placebo.
Treatment:
Empirical antibacterial therapy is selected according to the disease severity and likely pathogen.
Infectious Diseases Society of America
For hospitalized patients with non-severe bacterial CAP empirical treatment with a beta lactase such as triaxone in combination with the macrolide such as erythromycin or fluoroquinoline monotherapy is recommended.
Because of adverse affects floroquinone monotherapy is not recommended.
Ambulatory patients younger than 65 years of age, and otherwise healthy, antibiotics are recommended: amoxicillin, doxycycline, or a macrolide.
For patients who have taken antibiotics within the past three months or have serious, coexisting underlying diseases, amoxicillin – clavulanate is recommended.
For hospitalized patients, and those risk factors for MRSA or pseudomonas a beta lactam plus a macrolide or doxycycline or a fluoroquinolone is recommended.
The use of steroids has been shown to be beneficial for patients with severe CAP and respiratory insufficiency/mechanical ventilation.
Antibiotic therapy is typically continued until the patients have become afebrile and stable for at least 48 hours, with treatment continued for a minimum of three to five days.
Patients with a history of CAP have a higher rate of recurrence and should avoid smoking and assume alcohol cessation and relevant vaccination management.
Patients should be counseled about good oral hygiene management and have underlining cardiac and pulmonary conditions managed appropriately.
Patients with a history of aspiration should have behavioral strategies to reduce such processes.
