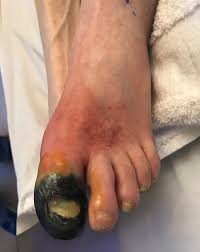
 Chronic limb threatening ischemia (CLTI), is an advanced stage of peripheral artery disease (PAD).
Chronic limb threatening ischemia (CLTI), is an advanced stage of peripheral artery disease (PAD).
It is defined as ischemic rest pain, arterial insufficiency ulcers, and gangrene.
There is surface damage to the limb tissue due to the most severe stage of ischemia.
Atherosclerotic plaque below the knees tends to contain more calcium and luminal thrombus than atherosclerotic lesions above the knees and affects the response to therapies that are more commonly applied when treating arteries above the knee.
CLTI is associated with a high risk of amputation.
The adverse limb outcomes associated with CLTI, affect quality of life and life expectancy: the prognosis is apparently worse than that for most cancers.
In the US the prevalence and incidence of CLTI are estimated to be 1.3%, and 0.35%, respectively, which translates to up to 1 million persons in the Medicare population alone.
Compared to intermittent claudication, CLTI has a negative prognosis within a year after the initial diagnosis, with 1-year amputation rates of approximately 12% and mortality of 50% at 5 years and 70% at 10 years.
CLTI affects up to 11% of the population of peripheral artery disease worldwide.
CLTI prevalence is 15% among Medicare patients who present for treatment of peripheral arterial disease.
CLTI, affects more than 230 million people globally, including 7 to 12,000,000 people in the US alone.
The estimated cost of CLTI is approximately $12 billion annually in the US.
The limb threat includes the risk of amputation associated with severely infected and non-healing wounds.
Rest pain is characterized by continuous burning pain of the lower leg or feet.
Rest pain begins, or is aggravated, after reclining or elevating the limb and is relieved by sitting or standing.
It is more severe than intermittent claudication.
Tissue loss occurs with the development of arterial insufficiency ulcers or gangrene due to peripheral artery disease
Amputation for a chronic limb threatening ischemia is associated with a 50% mortality within a year after amputation in patients over the age of 65 years.
Major amputation for chronic limb, threatening ischemia is highest among patients with coexisting cardiovascular conditions.
Diagnosis:
Critical limb ischemia is diagnosed by the presence of ischemic rest pain, and an ulcers that will not heal or gangrene due to insufficient blood flow.
Insufficient blood flow may be confirmed by ankle-brachial index (ABI), ankle pressure, toe-brachial index (TBI), toe systolic pressure, transcutaneous oxygen measurement or skin perfusion pressure, a capillary refill of more than 15 seconds or diminished or absent pulses.
Acute limb ischemia is a sudden lack of blood flow to the limb, for example caused by an embolus whereas critical limb ischemia is a late sign of a progressive chronic disease.
Without prompt revascularization, the incidence of limb amputation is approximately 25% at one year after diagnosis.
Treatment:
Modifying risk factors, revascularization via vascular bypass or angioplasty, and with tissue loss, wound debridement.
Surgical bypass and endovascular therapy of the principal revascularization strategies used to treat CLTI.
Surgical revascularization with saphenousvein bypass increases the likelihood of limb salvage in highly selected patients.
With open surgery an autologous vein or prosthetic tubes are used to bypass the occluded artery, and percutaneous endovascular procedures, in which balloon angioplasty angioplasty is used to open a blocked vessel.
Among patients with CLTI who had adequate great saphenous vein for surgical revascularization, the incidence of major adverse limb event or death was significantly lower in a surgical group than in an endovascular group (Farber A).
In another trial the frequency of amputation free survival was 57% among patients in the surgical group and 52% among those in the angioplastic group at three years.
Overall, studies suggest that surgical revascularization is optimum compared to angioplastic procedures.
Both surgical and percutaneous approaches to critical limb ischemia connect artery to artery and require a downstream target of an unobstructed vessel in the lower leg or foot, on which to land the treatment.
About 20% of patients with chronic limb threatening ischemia have no revascularization options, leading to above ankle amputation.
CLTI, of the infra popliteal artery system is associated with frequent reintervention and adverse limb outcomes from restenosis.
Transcatheter arterialization of the deep veins is a percutaneous approach, creating an artery to vein connection to deliver oxygenated blood by means of the venous system to the ischemic foot to prevent amputation.
Oxygenated blood is diverted from the tibial arteries to the tibial veins to bypass the severely diseased arterial vasculature, and the venous system is leveraged to deliver oxygenated arterial blood to the foot through the pedal veins.
This potentially averts major, amputation, and promotes healing.
Transcatheter arterializaation of the deep veins is safe and successful in patients with chronic limb, threatening ischemia and no conventional surgical or endovascular revascularization treatment options (ShishrhborMH).
Endovascular therapy in arterial vessels below the knees has limitations, which include elastic recoil, dissection, and stenosis of the artery, reducing the durability of the procedure.
Among patients with CLTI due to infra popliteal artery disease the use of a everolimus eluding resorbable scaffold produced superior results to angioplasty.
Resorbable scaffolds provide support to vessel walls and prevent acute and subacute artery closure.
Overtime such devices are reabsorbed and fosters more natural artery remodeling.
These devices may provide a platform for drug elution, as well.
