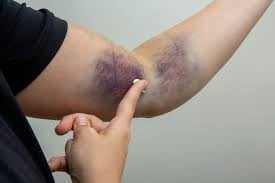
A bruise, also known as a contusion, is a type of hematoma of tissue.
the most common cause being capillaries damaged by trauma, causing localized bleeding that extravasates into the surrounding interstitial tissues.
Most bruises occur close enough to the epidermis such that the bleeding causes a visible discoloration.
Bruises remain visible until the blood is either absorbed by tissues or cleared by immune system action.
Bruises which do not blanch under pressure can involve capillaries at the level of skin, subcutaneous tissue, muscle, or bone.
RICE: rest, ice, compression, and elevation is management.
Bruises are not to be confused with similar-looking lesions: Such lesions include petechia (less than 3 mm (0.12 in), resulting from numerous and diverse etiologies such as adverse reactions from medications such as warfarin, straining, asphyxiation, platelet disorders and diseases such as cytomegalovirus and purpura (3–10 mm (0.12–0.39 in)), classified as palpable purpura or non-palpable purpura and indicating various pathologic conditions such as thrombocytopenia.
Many terminology schemas treat an ecchymosis of more than 1 cm (0.39 in)) as synonymous with a bruise, but in some other schemas, an ecchymosis is differentiated by its remoteness from the source and cause of bleeding, with blood dissecting through tissue planes and settling in an area remote from the site of trauma or even nontraumatic pathology, such as in periorbital ecchymosis arising from a basilar skull fracture or from a neuroblastoma.
Trauma sufficient to cause bruising can occur from: accidents, falls, and surgeries.
Disease states such as insufficient or malfunctioning platelets, other coagulation deficiencies, or vascular disorders, such as venous blockage can lead to the formation of purpura which is not to be confused with trauma-related bruising/contusion.
If the trauma is sufficient to break the skin and allow blood to escape the interstitial tissues, the injury is not a bruise but bleeding, a different variety of hemorrhage.
Such injuries may be accompanied by bruising elsewhere.
Bruises often induce pain immediately after the trauma that results in their formation.
Sometimes bruises can be serious, leading to other more life-threatening forms of hematoma.
Minor bruises may be easily recognized in people with light skin color by characteristic blue or purple in the days following the injury.
Hematomas can be subdivided by size:
Ecchymoses are 1 centimetres in size or larger, and are therefore larger than petechiae, which are less than 3 millimetres in diameter or purpura 3 to 10 millimetres in diameter.
Ecchymoses also have a more diffuse border than other purpura.
Ecchymosis is the escape of blood into the tissues from ruptured blood vessels.
Ecchymosis term also applies to the subcutaneous discoloration resulting from seepage of blood within the injured tissue.
Bruise colors vary from red, blue, or almost black, depending on the severity of broken capillaries or blood vessels within the bruise site.
Broken venules or arterioles often result in a deep blue or dark red bruise, respectively.
Darker colored bruises may result from a more severe bleeding from both blood vessels.
Older bruises may appear yellow, green or brown.
Many causes of subcutaneous hematomas including ecchymoses.
Coagulopathies such as hemophilia A may cause ecchymoses.
Steroids can have the adverse effect of causing ecchymoses.
The presence of bruises may be seen in patients with platelet or coagulation disorders, or those who are being treated with an anticoagulant.
Unexplained bruising may be a warning sign of child abuse, domestic abuse, or serious medical problems such as leukemia or meningoccocal infection.
Long-term steroid therapy can cause easy bruising.
Bruising present around the navel with severe abdominal pain suggests acute pancreatitis.
Connective tissue disorders such as Ehlers–Danlos syndrome may cause relatively easy or spontaneous bruising.
Spontaneous bruising or bruising with minimal trauma in the absence of other explanations and together with other minor or major criteria suggestive of vascular Ehlers–Danlos Syndrome (vEDS) .
Bruises often become more prominent as time lapses.
In soft tissues, a larger area can be bruised than would be allowed by firmer tissue due to ease of blood to invade tissue.
Age: elderly skin and other tissues are often thinner and less elastic and thus more prone to bruising.
Gender: More bruising occurs in females due to increased subcutaneous fat.
Skin tone: Discoloration caused by bruises is more prominent in lighter complected people.
Coagulation, platelet and blood vessel diseases or deficiencies can increase bruising due to more bleeding.
More extensive vascularity at a site causes more bleeding.
Areas such as the arms, knees, shins and the facial area are especially common bruise sites.
Greater striking forces cause greater bruising.
Natural redheads have been shown to bruise more: perhaps due to greater visibility on commonly associated lighter complexion.
Bruises can be rated on a scale from 0–5 to categorize the severity and danger of the injury.
0 Light bruise No damage
1 Mild bruise Little damage
2 Moderate bruise Some damage
3 Serious bruise Dangerous
4 Extremely serious bruise Very dangerous
5 Critical bruise Risk of death
Capillaries vary in strength, stiffness and toughness, which can also vary by age and medical conditions.
Severe bruising may be dangerous or cause serious complications.
Bleeding and excess fluid may accumulate causing a hard, fluctuating lump or swelling hematoma.
This has the potential to cause compartment syndrome in which the swelling cuts off blood flow to the tissues.
The trauma that induced the bruise may also have caused other severe and potentially fatal harm to internal organs.
Increased distress to tissue causes capillaries to break under the skin, allowing blood to escape and build up.
As time progresses, blood seeps into the surrounding tissues, causing the bruise to darken and spread.
Nerve endings within the affected tissue detect the increased pressure, which, depending on severity and location, may be perceived as pain or pressure or be asymptomatic.
Damaged capillary endothelium releases endothelin, a hormone that causes narrowing of the blood vessel to minimize bleeding.
With endothelium destruction, underlying von Willebrand factor is initiates coagulation, which creates a temporary clot to plug the wound and eventually leads to restoration of normal tissue.
Larger bruises may change color due to the breakdown of hemoglobin from within escaped red blood cells in the extracellular space.
The striking colors of a bruise are caused by the phagocytosis and sequential degradation of hemoglobin to biliverdin to bilirubin to hemosiderin, with hemoglobin itself producing a red-blue color, biliverdin producing a green color, bilirubin producing a yellow color, and hemosiderin producing a golden-brown color.
When these products are cleared from the area, the bruise disappears.
Treatment for light bruises is minimal: RICE (rest, ice, compression, and elevation), painkillers and, later in recovery, light stretching exercises.
The immediate application of ice may reduce or completely prevent swelling by restricting blood flow to the area and preventing internal bleeding.
Messaging techniques should not be applied until at least three days following the initial damage to ensure all internal bleeding has stopped, because although increasing blood flow will allow more healing factors into the area and encourage drainage, if the injury is still bleeding this will allow more blood to seep out of the wound and cause the bruise to become worse.
In most cases hematomas spontaneously revert.
In cases of large hematomas or those localized in certain organs performing a puncture of the hematoma to allow blood to exit.
