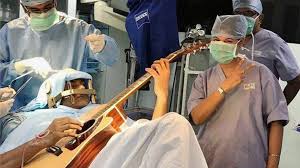
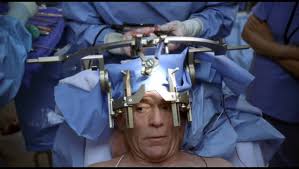
 Awake craniotomy is a neurosurgical technique and type of craniotomy that allows a surgeon to remove a brain tumor while the patient is awake to avoid brain damage.
Awake craniotomy is a neurosurgical technique and type of craniotomy that allows a surgeon to remove a brain tumor while the patient is awake to avoid brain damage.
The neurosurgeon performs cortical mapping to identify vital areas.
These vital areas are called the eloquent brain, that should not be disturbed while removing the tumor.
short term transient deficits are regular part of surgical treatment of lesions in eloquent areas because of the proximity to relevant subcortical white matter and potential functional re organization occurring in the first few weeks after surgery.
Permanent surgical related deficits should be avoided under all circumstances.
It is particularly useful for awake craniotomy to map the cortex to avoid causing language or movement deficits with the surgery.
The technique is associated with improved outcomes in patients with glioma, most notably neurological outcomes, functional and cognitive outcomes, radiological outcomes, and survival outcomes.
The extent of resection, overall survival, and neurological outcomes are better in patients undergoing awake craniotomy than in patients who have asleep resection in glioblastoma (Gerritsen JK).
Patients with better pre-operative performance status and younger patients have fewer neurologic deficits postoperatively and the best chance of attaining improved results.
It is more effective than surgeries performed under general anesthesia in avoiding complications.
Awake craniotomy can be used in a variety of brain tumors, including glioblastomas, gliomas, and brain metastases.
Awake craniotomy can also be used for epilepsy surgery to remove a larger amount of tissue causing the seizures without damaging function.
Awake craniotomy can be used for deep brain stimulation placement, or for pallidotomy.
Awake craniotomy reduces recovery time.
Its purpose is to with reduce iatrogenic brain damage from surgery
The patient is given anxiolytic medications, and then positioned in a neurosurgical head restraint that holds the head completely still and given general anesthesia.
Local anesthetics are used to numb the skin and bone of the head and neck.
The surgeon removes an area of the skull over the tumor and cutting into the meninges.
Before removing any brain tissue, the patient is awakened and a a cortical map, using a small electrical stimulation device to observe the changes in the patient’s condition when an area is stimulated is created.
Vital areas so identified are not removed or cut through to access a tumor.
There are two variations on the technique: awake-asleep-awake (AAA), and monitored anesthetic care (MAC), also called conscious sedation.
In an AAA surgery, the patient is only awake during the cortical mapping; whereas in an MAC surgery the patient is awake the entire time.
With deep brain stimulation placement is similar, but a burr hole is drilled for the electrodes instead and the MAC surgery is more common.
The complications of awake craniotomy: seizures during the operation, nausea, vomiting, loss of motor or speech function, hemodynamic instability with hypertension, hypotension, or tachycardia, cerebral edema, hemorrhage, stroke or air embolism, and death.
Seizures are the most common complication.
Awake craniotomy is not appropriate for patients with anxiety disorders, claustrophobia, schizophrenia, low pain tolerance, and obstructive sleep apnea.

One reply on “Awake craniotomy”
This Blog Is Very Helpful And Informative For This Particular Topic. I Appreciate Your Effort That Has Been Taken To Write This Blog For Us. Craniotomy nursing care, craniotomy post operative care, craniotomy nursing management, craniotomy after care, post operative nursing care for craniotomy, craniotomy physical therapy, physical therapy after craniotomy, craniotomy patient care, nursing care of craniotomy patient, post operative care of craniotomy patient. physiotherapy in Hyderabad