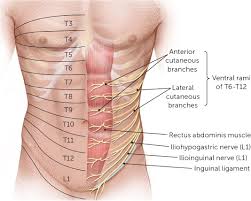
 Anterior cutaneous nerve entrapment syndrome (ACNES) is a nerve entrapment condition that causes chronic pain of the abdominal wall.
Anterior cutaneous nerve entrapment syndrome (ACNES) is a nerve entrapment condition that causes chronic pain of the abdominal wall.
It occurs when nerve endings of the lower thoracic intercostal nerves (7–12) are entrapped in abdominal muscles, causing a severe localized nerve pain that is usually experienced at the front of the abdomen.
Its pathophysiology is related to compression and irritation of the intercostal nerve endings the pass through the rectus abdominus muscle and innervate the oblique muscles.
Subsequent abdominus muscle spasms result in progressive nerve entrapment and perpetuates pain.
Approximately 1/3 of patients have had and inciting event such as surgery on the abdomen, abdominal trauma or sports related injury, pregnancy, or influenza infection.
Most patients, however, do not report a clear precipitating event.
ACNES occurs spontaneously in 75% of adolescents who develop the condition.
ACNES is frequently overlooked and unrecognized.
The incidence is estimated to be 1:2000 patients.
In the study of patients presenting to the ED with acute abdominal pain, 2% were diagnosed with ACNES.
Median interval between symptom onset and diagnosis is 18 months.
One study suggested diagnosis be delayed for more than five years in 12% of patients, and many have been misdiagnosed with IBS, fibromyalgia, appendicitis, complex regional pain syndrome, or rheumatoid arthritis.
Pain is typically related to tensing the abdominal wall muscles, so any type of movement is prone to aggravate pain.
Most patients report that they cannot sleep on the painful side.
Many complain of visceral symptoms of nausea, vomiting and bloating.
Diagnosis:
Based on the patient’s history, and physical examination: looking for a painful spot, which worsens by tensing the abdominal muscles with lifting the head and straightened legs, the Carnett’s sign.
A positive Carnett test has been reported in 87% of patients.
78% of patients have severe pain with skin pinching, and 68% have altered skin perception to light touch or cold temperatures in the affected area.
Almost always, a small area of maximal pain is covered by a larger area of altered skin sensibility with somatosensory disturbances such as hypoesthesia as well as hyperesthesia or hyperalgesia and change of cool perception. Pinching the skin between thumb and index finger is extremely painful compared to the opposite non-involved side.[8]
The diagnosis is made on the basis of history and characteristic clinical findings.
Abdominal pain is in an area of 1 cm or less at the lateral border of the rectus abdominus muscle.
Confirmation of a diagnosis of ACNES is warranted using an abdominal wall infiltration with a local anesthetic agent near the painful spot: 86% have reduced pain.
10 to 20% of patients with ACNES have persistent pain relief after a single injection.
Most patients with ACNES develop recurrent abdominal pain typically treated with up to two additional injections of lidocaine.
Radiofrequency therapy decreases abdominal in 50% of patients.
Neurectomy consisting of surgical removal of the intercostal nerve branches may relieve pain for patients with recurrent or refractory discomfort despite lidocaine injections.
Four times more common in females than males.
Median age at diagnosis is 40-50 years.
Can affect individuals of any age and typically causes abdominal pain below the level of the umbilicus.
It is more frequent on the right side.
Up to 50% of patients with ACNES have symptoms such as nausea, bloating, abdominal swelling and loss of appetite.
Treatment:
Anesthetic injections, sometimes combined with corticosteroids, yields persistent pain relief in two-thirds of patients.
The volume of the injection may also break apart the adhesions or fibrosis responsible for the entrapment symptoms.
Refractory patients can be offered a surgical approach whereby terminal branches of an intercostal nerve are removed at the level of the anterior sheath of the rectus abdominal muscle.
This procedure is an anterior neurectomy.
73% of the patients who underwent a neurectomy were pain free, compared to 18% in the non-nerve resected group.
This syndrome is predominantly found in young women.
It does occur in children, teenagers and octogenarians.
